The following is an excerpt taken from The Fear of Doing Nothing: Notes of a Young Therapist by Valery Hazanov, published by Sphinx, an imprint of Aeon Books © 2019 and reprinted with permission of the publisher.
My First Private Patient
Climbing up the stairs from the subway stop on 13th Street, I reached for my phone and saw a text from a former classmate. It was August 2015; I had just received my license.
“Val, it’s been ages!” she wrote. “How are you? Did you start your practice already? Someone asked me for a referral: a professor from Moscow who’s looking for a Russian-speaking therapist in the city. I don’t know him, but his son works with Daniel and sounds really nice … Would you be interested? Let me know and we need to get drinks!”
“The man, I learned from his son, was a microbiology researcher in his seventies who came to New York for an experimental treatment of cancer”, with which he had been diagnosed a few months earlier.
“We would like you to work with him on themes of positive thinking and optimism,” the son told me over the phone. “We understand that it might be crucial for the success of his treatment.”
I did not have a practice, but quickly (Israeli style) arranged something for the following Friday: John, the leader of the men’s group, lent me his place near Central Park. It was a good-looking room with many ancient artefacts, an enormous sofa, and a window that looked onto a leafy courtyard with two benches.
I came thirty minutes early and as I was waiting for Mikhail Alekseyevich to arrive, I photographed the room with my phone camera and sent it to my mom and a few friends in Israel.
“Look at you, Doctor!”
“Beautiful, Valery …”
“Can we come for a session?”
I was standing by the window, trying to imagine who I would meet, reflecting on the irony of my first private patient being from Moscow, thinking about the type of Russian he might be – in what sociological box from my past would he fit …
A buzz at the door. We begin.
***
“Here?” an older woman asked nervously as she was wheeling in Mikhail, who seemed disinterested, slumped in his wheelchair, looking very thin, turning his gaze to the window – away from me.
“Hi, I’m Valera. Nice to meet you.” I shook their hands.
They introduced themselves.
“Welcome to New York, Mikhail Alekseyevich,” I said after his wife had left the room.
“Puzzling city …” he replied in a pensive voice.
“How so?”
“I don’t know. Who are you? I didn’t quite comprehend from my son. He keeps taking me to all these appointments. Are you a doctor?”
“I’m a psychologist.”
“A psychologist? He didn't mention…I’m surprised he brought me here, I never understood what psychologists do.”
“Me neither.”
““You tell people that everything will be alright?””
I laughed. “Something like that.”
“How old are you?”
“Thirty-three.”
“Young, young … And where are your parents? In Moscow? Here?”
“My mom lives in Colorado and my dad is in Israel, where I grew up.”
“My God. You have no one here. How do you manage?”
“I run a lot.”
“I see. That’s good. So tell me, psychology, is it even scientific?”
“I don’t think it’s scientific.”
“You see, Valery, my cousin’s daughter in Moscow is a psychologist,” he said with a grimace. “She tried to explain many times … She’s a singer, she does yoga, she lights candles that smell nice. She told me that there are three ways to be happy, but I can’t remember them … What’s a psychologist then? What exactly do you do?”
“Have you read The Grapes of Wrath?”
“Yes. Many years ago.”
“Remember the guilt-ridden uncle who’s dying to talk to someone and ends up drinking instead?”
“Vaguely.”
“The family needs to keep moving, if you remember. There’s no time for what he needs. He keeps bugging them, wants to tell somebody, anybody, what happened to his wife and how it was all his fault. He’s breaking down, he’s feeling ashamed. He’s lonely and misunderstood. I talk to people like him.”
“And?”
“Sometimes it helps. Sometimes it doesn’t do anything.”
“What will it do to me?”
“I’m not sure yet.”
““How will you ‘cure’ me? Tell me to forget that I have cancer and look at the positive things in life?””
Checkmate against the psychologist by the Russian researcher, by generations of people who did it all by themselves, who withstood Stalin and the World War and the Gulag and never complained and kept on going. No need for therapists, thank you very much, we’ll manage by ourselves. But tell me, psychologist, what is your plan? Will you tell me that everything will be fine and I’ll whine a little and feel sorry for myself?
“I don’t think I’ll do that. It sounds like a terrible idea,” I said.
“What then?”
“You tell me: maybe you want to fight, maybe you want to let go.”
“Oh, I don’t know. Honestly, I don’t even know what I’m doing here. ‘It’s a new treatment,’ they said to lure me. ‘You don’t have it in Russia!’ Big deal. All I wanted was to die in Moscow and that’s not going to happen. But I don’t want to talk about that…I don’t want to talk about myself. I’m gone, I’m not interesting anymore. In a moment I’ll be back to dust: a forgotten man in a forgotten place. You, on the other hand! You’re young, so young … You have a future, you have something to look forward to, something to hope for, something to wake up to in the morning that is not a CT scan or a blood transfusion or a ‘lab analysis’ or a ‘Mr. Barsky, have you given a urine sample this morning? Was it too yellow, Mr. Barsky? We’re a little worried, Mr. Barsky.’ ‘Oh, are you?! A little worried?’ I don’t want to talk about that nonsense. I want to talk about you.”
“I understand. What would you like to know?”
“For example, where do you live?”
“I live in Brooklyn, by a park that’s called Fort Greene.”
“A big park?”
“Not too big, I see it from my living room window.”
“Nice. Who do you live with? You’re married?”
“I used to be … I live with my best friend.”
“Well, that’s not the worst.”
“It’s not.”
“Do you like New York?”
“Not particularly.”
“Why not?”
“Because it’s a place that’s good at separating people; not so good at bringing them together.”
“Interesting. What’s your favourite city then?”
“I like Jerusalem.”
“Why?”
“It’s chaos, it’s the Middle East, everyone’s in your face. That’s more to my liking.”
“You’re an interesting type, Valery…I wonder what’s behind the mask, though!” he said, smiling.
I laughed. “”Behind the mask of a psychologist there’s another psychologist, and then there’s another one – until there’s a person.””
He laughed too. “Another question: what did you have for breakfast?”
“I had coffee and toast with strawberry jam.”
“I can’t have that, you know? Dietary restrictions,” Mikhail said, sighing.
“Mikhail Alekseyevich,” I said after a pause. “Your son told me that your cancer is at the fourth stage.”
“That’s right.”
“How has it been?”
The ping-pongy nature of our conversation never stopped. Mikhail didn’t want to tell me how it had been, but he also didn’t want to leave. He lingered in the office even after I had told him that our time was up. He wanted to talk about music, about places in New York that I liked, about where I grew up in Moscow.
John’s cozy room, the garden outside, my life’s story – it was all a respite from his painful reality: torn from his home, dying from cancer, treated by people whose language he did not understand.
Was it a psychotherapy session if I told him more about my life than he told me about his?
As we said our goodbyes, I wasn’t sure if he wanted to return or not. “Let’s be in touch,” he said as his wife was wheeling him out.
“I left the session feeling that I had met Nabokov’s Pnin” – a Russian intellectual in exile, never fitting into his surroundings, not quite sure what to do in America, how to be. Clearly not a person who would voluntarily stumble into a psychotherapist’s office asking for help. Smart, witty, playful: I really hoped I would see him again. I hoped that I had placed enough hooks, dismantled the psychologist stereotype he had had in his mind – it was the only way in, I felt. One word of jargon, one “It must be so hard for you,” one “I feel that you are experiencing some ambivalence about seeking help, Mikhail Alekseyevich,” one “There is something scary about opening up and talking about ourselves,” and he would have walked away, never coming back. “Americans,” he would have thought, “psychologists,” he would have told himself, “why can’t they talk in a normal way?”
A few days after the session, I called him.
“Yes, dear,” Mikhail answered in a soft voice. “I’m listening.”
“Your son told me that you haven’t been feeling too well.”
“Oh, you know, it’s to be expected with my diagnosis. But how are you? Did you have a nice weekend? Did you spend it in the city?”
“It was alright.”
“What did you do?”
“Went for a run, wrote in the library, met up with a friend.”
“Nice, very nice. Good for you.”
“Will I see you again, Mikhail Alekseyevich?”
“Sure, why not? But there is a small problem: I can’t leave the place I’m at anymore because of my condition. That’s what they told me, I’m stuck here.”
“I’ll come over.”
Three days later I appeared at the treatment facility in which Mikhail had been hospitalized. It was one of those modern places that are part hospital, part living apartments. There were inspirational quotes on the walls and names of donors. The rooms were given names like “Mist” and “Four Winds”. It looked like a getaway hotel by the hot springs, except that all the residents had cancer.
Mikhail was sitting in a wheelchair when I came, his tiny body covered with an enormous woolen blanket, pointing to the table next to his bed with medical equipment: “Needles, stupid needles …”
“Only a week had passed since our first meeting, but he looked much weaker and sicker”.
“First things first,” he said. “Are you hungry? Would you like to eat something?”
“No, I’m fine, thank you.”
“Well, at least allow me to pour you some tea.”
Drinking tea together, we eased into a conversation about Russia. Mikhail was dismayed by what was going on, telling me about how politics had ruined science, how people didn’t feel free anymore, how it all looked familiarly scary.
“Why does it feel like a damn cycle?” he wondered. “A predetermined fall to the abyss.”
“It does feel like a tragedy … We know how it will end but can’t do anything about it.”
“Exactly,” he nodded.
“When I think of Russia,” I said, “I only think about the very distant past, and about Moscow, which I absolutely love. It’s not the ‘right’ approach for immigrants, we’re supposed to hate it, to bemoan the glitzy, materialistic behemoth that Moscow has become. ‘Oh, how terrible! They only have Gucci boutiques all over, what happened to our Moscow?’ But beneath it, beside it, apart from it…You have the little squares, the theatres, and they renovated nicely, and I just love the feeling of walking there. It’s a funny thing to go back. You know they have this train from the airport that goes to the centre? Then you can take the metro, two stops to Kiyevskaya, around where I grew up. Last time I was there I got out of the train and was amazed: it’s like it hasn’t been twenty-five years, it’s like I never left. Strange feeling.”
“You’re a nostalgic person, my friend.”
“That’s true. But…there is this idea of a Country, of what it stands for, its values, etc. Living here, I’ve been thinking a lot about the bubbles, the niches in which we live; the Tuesday mornings and the Sunday afternoons. And sometimes they have nothing to do with the Idea, with Putin, with the ‘political situation’. It’s either good or bad. It’s a texture of living that either works or doesn’t.”
“I know what you mean.”
“I talk a lot for a psychologist.”
“I wouldn’t know.”
“Tell me something.”
“I was thinking about my family when you were talking. How we all spread around, like birds who flew to find warmer climates and never came back. My two sons are here: one in New York, as you know, the other one in Boston. They did well, I think, I hope.”
“How often do you see them?”
“Once a year, maybe twice. Tatyana and I visit occasionally, stay for the summer, spend some time with the grandchildren. Sometimes they would come visit us in Moscow. But it’s a peculiar feeling: after all this time, all this flying around, I am sitting in Four Winds ready to die and be buried, and where? Where do they bury people here?”
“I think in Queens, maybe in the Bronx.”
“Okay, ‘Queens’. What the hell is Queens? What does it have to do with me, with what I have done in my life?”
“It has something to do with your children and their children.”
“True. But it’s still odd, this whole thing. What is a place? What does it mean to be from somewhere, to live somewhere? I don’t know anymore.”
“Me neither …”
We never met at John’s place again. “Every week, at varying times, based on Mikhail’s medical procedures and condition, I would come to sit with him by his bed”, or take him to the porch outside Four Winds.
We did many things together. We watched YouTube (a scene from Tarkovsky’s Sacrifice with Bach’s St Matthew Passion superimposed was his favourite), we talked about his research and what he thought needed to happen to it, about the papers he wanted to finish but felt he would never be able to. We talked about Russian literature, about immigration, about Israel. We ate fruit and snacks. I brought him a ginger ale once (he had a sudden craving), and a chocolate bar another time – I don’t remember if he was allowed to eat that …
“Thank you for coming,” Mikhail would always say when he saw me. “What’s the news?”
He liked when I described, in detail, a certain place in New York, like a park, or a building.
His face would light up. “What do you see when you enter it? How big is it? What is its exact circumference?”
I never knew, of course, but I would google it in his presence and we would talk about that and I would learn things like the area of Riverside Park (266.791 acres) or the year the Avery Library at Columbia was founded (1890).
With time, and only after starting with the perimeters and context of his life, we were able to go deeper – dreams, regrets; soul stuff.
“What do you miss the most?”
“I miss my sofa in Moscow! I’m serious! We just bought it, it felt like a big achievement …”
“Funny.”
“I miss being needed.”
“Yeah …”
“No one needs me now. Who am I? An old man who’s waiting…waiting to end this.”
“What exactly do you mean by needed though?”
“Someone calls: ‘Prof Barsky, what do you think we should do with this experiment, this paper?’ etc.”
“What about your family, how do they need you?”
“I don’t know. Now, I don't know. I feel like I’m just a bit of a nuisance.”
“Judging by their relentless attempt to keep you alive, it doesn’t feel that way.”
“True. Maybe they got attached.”
“What do you mean, ‘maybe’?”
“Well, yeah, definitely.”
“It’s just that the work was at the centre of your life…Now that it’s been taken away you probably wonder what’s left.”
“You’re right. Not much. And let me be completely honest: I don’t know how to face this, Valery. I really don’t. Can modern psychology help us here?”
“I’m not sure.”
“Have you ever worked with dying patients?”
“No, I haven't.”
“So, what do you think, how should I do it?”
“Big question…Words like ‘meaning’ or ‘acceptance’ – you know them, you don’t need me to repeat them. But then how else can we talk about it? I’m not sure…Maybe reduction of bitterness? Making it a project of extreme gratitude to what’s around, to who’s around? I mean, it’s true for me as well – can’t hurt.”
““Coming to terms, coming to terms,” he said with a smile. “I’ve never done it!””
“We all suck at this. But tell me stories, it helps.”
Often when we sat on the porch he would put his hand on mine and we would be silent for a few minutes. Then, he would remember something recent or very distant, associatively it seemed, and tell me about it.
“There was this type, what was his name…Ah! Igor Bogdanov, yes, yes. Anyway, it must have been in the Seventies. We were just starting out, he was at my department then and we had a trip together to Nizhny Novgorod, to give a talk or something at the local university. We took the train from Moscow, seven or eight hours, I don’t remember, and delved into a conversation about the department, its politics – the usual stuff. And then he turns to me, I still remember it, and says: ‘Misha, you know what? You’re too gentle for science.’ That’s what he said: ‘too gentle’.”
“Are you?”
“I don’t know. Sometimes I think I was. Science, you see, you need to fight there, you need to push, forget about everything, about everyone. I am not sure I was able to do that. I have regrets, Valery. I live with certain regrets; I think I could have done more. Publish more, teach more, forgive me for the pathos: discover more.”
“Yeah…”
“I can’t shake these feelings off. I understand in my head: ‘You’ve done a lot, stop!’ But it doesn’t feel like that, it doesn’t feel enough.”
“How will we get you there?”
“I thought you were the expert!”
“I thought we had agreed it’s not scientific!”
He smiled and shook his head.
“There is this question in psychotherapy that I frequently think about: whether it is a process that’s supposed to make us feel better about who we are or to change who we are.”
“And what do you think?”
“I think, ultimately, it’s about acceptance.”
“Okay. But it bothers me, it does. It’s such a childish thing to be bothered with. I mean, how infantile: I am sitting here thousands of kilometres away, forty-five years later, ready to die, still thinking about that comment.”
“But what bothers us always feels childish. That’s inherent in ‘bother’.”
“How so?”
“‘How un-Stoic of me, why can’t I regulate myself, how am I swayed by stupid emotions…’ That’s what we think when we are ‘bothered’ by something, no? But what’s an emotion? It’s the basics, it’s us as a kid, it is childish.”
“Okay.”
“I have a friend in Israel who told me a story once. During his reserve service in the army he was stuck for weeks in a remote base somewhere. One of his friends came to him there in the camp, I think he was doing the dishes or something, and his friend goes: ‘Yona, you know what I realised? You’re a lone wolf.’ My friend told me that he could never forget that comment. It’s nothing, right? Completely innocuous. But that’s the thing: it’s always simple. A word, a sentence that hits something real. And then we obsess over it and feel foolish, or, if we’re lucky, relieved – in psychotherapy…”
“Was he a lone wolf?”
“Probably.”
“And if he were your patient would you have tried to change that?”
“I would have told him: when you hunt, hunt together sometimes, brother.”
Mikhail laughed, but then stopped. “And what would you tell me?” he asked, closing his eyes halfway. “Do you think I was too gentle?”
“I don’t know,” I said. “But if I had to guess, I would guess that your gentleness was a gift from God that made you the scientist that you are.”
***
The treatment facility in which Mikhail had been hospitalized was in a constant state of buzz. There were doctors and nurses and relatives and other patients in perpetual movement. There were many TVs and they were always on and for some reason it was CNN and the news, most of the time. There were people with different-sounding professions that would come, every couple of minutes, it seemed, to the room and talk about physiotherapy that needed to be done, “management of care” that had to be managed, financial decisions that needed to be made, Mikhail’s diet, furniture that could be brought in or out according to Mikhail’s wishes, books that they were able to order for him in Russian and he should explore this opportunity because not in every place was it possible but it was possible there and if he would only ask…
Is the mobile phone working okay? Is the Wi-Fi signal strong enough? Would he prefer a vegetarian option for dinner? Does he need more channels in his cable? There are now options in Russian.
Mikhail, weary, deaf to this all, was motionless in reaction to this spinning around him. “Why can’t they leave me alone for a moment?” I imagined him thinking. “Why all these questions?”
“I don’t know if it’s true, but I felt that his life had been about protecting his sanity”, his focus, from the intrusion of this energy of mundane concerns. I don’t think that just because he had cancer that was slowly killing him, he became a person who could not stand any of that, who could not bring himself to care about that non-important nonsense. And I sympathized with him, obviously, and felt that it was appropriate that we were meeting at that frantic facility and not in a secluded office, because suddenly it emphasized an essential part of psychotherapy: its fending off of corrosive distraction – standing firm in the face of the never-ending attacks on the things that matter. Sorry for the clichés, but it did feel like we were creating an island, and we tried to protect that island together. And he was not just a patient, but rather a collaborator in that process, which was as much mine as his, I believe.
Whatever was going on in my life in the months of August and September of 2015, wherever I was – Mikhail was with me, transcending the confinements of the “consulting room”. Like a good friend who becomes a part of your daily existence, to whom you say that you feel tired, or that you like your tea with no sugar but with lemon, or that your back has been bothering you recently and it’s annoying. Somehow, he became that person. “He liked to call me on the phone, between our sessions, to tell me a story, or a joke, or ask for my “opinion” about something”. “Valera, milenkiy,” [my dear, in Russian] he would frequently conclude the conversation, “I miss you.”
Gradually, it became difficult for Mikhail to talk. He would take long breaks between sentences, holding his head as he tried to say something. “Valera,” he would say, “do you think we can fully be known by another person?”
“I think there are parts of ourselves that remain forever only ours.”
“Yes, yes. It’s true … And that’s what remains?”
“What do you mean?”
“That’s what we take with us?”
“I think we take more.”
“Maybe. It’s just that sometimes I think, what was it all for …?”
“You’re in a bad mood today.”
He laughed, weakly. “You’re right. It’s just … I don’t know how I can accept this. I had visualized something different.”
“What?”
“First of all, yes, and forgive me if it sounds infantile, but this was supposed to be happening in Moscow, in my apartment. I mean for heaven’s sake, I spent forty years there.”
“What else?”
“I didn’t achieve enough. I just didn’t. I was okay, I was a good researcher, but I could have done more. Much more. And it bothers me. Why didn’t we meet twenty years ago, Valery? This isn’t relevant anymore…What can you tell me now that will change that? Nothing!”
“Twenty years ago I was thirteen.”
“You know what I mean.”
“You mean that I was a top therapist at thirteen. I think you’re right.”
“Be serious.”
“There’s nothing to be serious about. It’s a bunch of thoughts in your head. It’s a fantasy that you created because you had thought that life is measured by some yardsticks that kept evading you, that kept getting higher and becoming unreachable. We make ourselves miserable believing in this nonsense, myself included, but it’s all about letting it go. And it’s never too late and you know it. You know it’s not too late because you can still think and you can still feel and you can look around and say, ‘Thank you very much world, God, universe, fate, me…’ – whatever you believe in – ‘for giving me my wife who has cared for me all my life, my two great sons, and their children who will be coming to my grave because that’s how they were raised. And thank God for at least one article or paper or invention that actually mattered for something and wasn’t just a bunch of words.’ You can do it right now.”
“Valera…”
***
A few more weeks had passed when I came to his room and saw that he couldn’t get out of bed anymore. He would lie, eyes closed, hand on his forehead, in pain, mumbling something to himself. He would try to get up on his elbows when I came, sometimes succeeding, sometimes not.
“Well, that’s what it’s come to,” he said in a shaking voice. “What should we talk about?”
“How is your pain?”
“Oy…” he sighed. “Look at my hands,” he said. They were all pink and swollen. He was dying.
And “I remember looking at him, understanding how ridiculous my thought was, but also that I couldn’t help but think – “Why? Why is he going? In what way is that fair?””
“Did you get some sleep tonight?”
“I did, I think.”
“Can you eat at all?”
“A little bit …”
“Can I bring you something?”
“No, no, I am okay.”
“Do you want me to read you something?”
“Yes, please.”
“Okay. Believe it or not, I’m reading you this from my mobile phone.”
“Wonderful.”
“‘And there in the middle, high above Prechistensky Boulevard, amidst a scattering of stars on every side but catching the eye through its closeness to the earth, its pure white light, and the long uplift of its tail, shone the comet, the huge, brilliant comet of 1812, that popular harbinger of untold horrors and the end of the world. But this bright comet with its long, shiny tail held no fears for Pierre. Quite the reverse: Pierre’s eyes glittered with tears of rapture as he gazed up at this radiant star, which must have traced its parabola through infinite space at speeds unimaginable and now suddenly seemed to have picked its spot in th
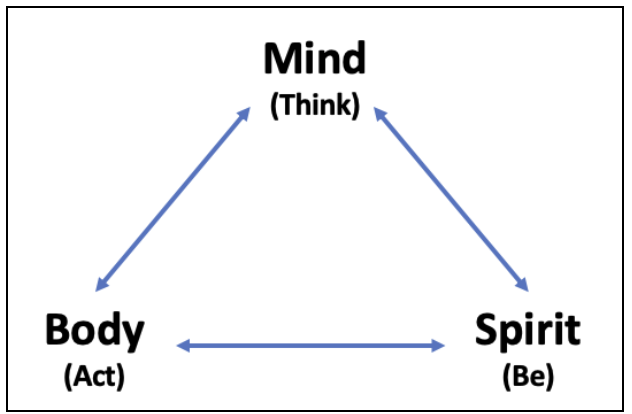 When I’m working with clients I often ask myself which of these paths might be most helpful to them at this point in their treatment.
When I’m working with clients I often ask myself which of these paths might be most helpful to them at this point in their treatment. We also worked toward taking care of tasks around the house that he’d been putting off and on building positive interactions with others since his relationships had suffered. Given his health challenges, we worked on ways to improve his sleep and eat more healthfully.
We also worked toward taking care of tasks around the house that he’d been putting off and on building positive interactions with others since his relationships had suffered. Given his health challenges, we worked on ways to improve his sleep and eat more healthfully.