A Woman Named Charlie
I tend to think of the initial few sessions with clients as a delicate endeavor, not so different from cooking a soufflé. If I ask them to dive too fully into a painful topic, or challenge their defenses too soon, the person may fold in on themselves, and the therapeutic process, like a rising cake whose oven door is opened too soon, haplessly deflates. But when we proceed gently and slowly during this early phase, a client who is in real trouble may allow her reality to surface, even revealing a serious crisis that might otherwise have been missed.
“My most delicate soufflé was a woman named Charlie”. I was just five years post-practicum when Charlie, ten years my senior, sat across from me for her first appointment. She held a strong, upright posture and bravely deliberate eye contact that didn't square with her disheveled appearance. It was as if her combination of long, scraggly hair, wrinkled clothes, slouched posture and no make-up were deliberate tools used to give the middle finger while at the same time beckoning for help. Her voice was menacing with this tone that was a combination of critical professor and sincere consumer. As we got to know each other, she rattled off effortless soundbites about her position as a president of research development with one of the world's largest technology corporations. She then detailed an exhausting list of stressors, including frequent eighteen-hour workdays, nightmares, loneliness, bereavement from a recently ended relationship and admitting that she knew, given the way she lived and what she did, that there might be no end to the pressures.
The more we talked, the more I marveled at how my conversation-style intake questions were answered with explicit brags about her academic and career accomplishments. This chance to let a new client explain why she’d come to therapy started to feel like a verbal tennis match, with each volley of words leaving me a little more bowled over by her intelligence and concerned that I had nothing to offer her.
And yet, I could hear in her voice a tinge of high-pitched panic just beneath the surface. It surfaced in response to her commenting about my arms being crossed. My gut told me this was a test to see if she could put me in the spotlight so that she might feel safe and no longer the focus. I responded by asking her what her incentive was for investing her precious little surplus time and energy in therapy. What was in her life or what did she want to have in her life that would make this worthwhile? “She stared at me for just a second, but looked right into my eyes and said, “I want to not want to die.”” She then said, “I ‘m not sure you can handle this, and, in a way, I apologize for being here.” My gut told me not to bluff and so I told her what was true; “I can handle hearing about your hell here on earth. I can handle learning what that is like for you. There is an unknown beyond this, because we are just starting, and the work and the process remains to be seen. I can handle someone feeling like giving up. But to handle you actually giving up is something I will do my best work to spare us both from.” Now I had the most important piece of information that was so well hidden under layers of success. This super-powered woman was in desperate pain, and for this, I vowed she would get my best efforts. Even if she did scare the crap out of me.
Playing Emotional Poker
One of the perks of being a therapist is that honesty and transparency are prime capital. I like how free clients and I are to ask each other deep questions, and I think there is something inherently optimistic about a conversation focused on learning how to heal and grow. In that first session, Charlie seemed to tune into that optimism herself. She said she was surprised that she didn’t feel like leaving, adding with a grimace, “at least not yet.” Soon she was telling me about her father's death when she was twelve, and how her mother reacted by shutting down, quitting her job, and beginning a new existence of voluntary confinement to her house.
Charlie sat forward and exhaled slowly before saying, "My mother made me promise not to go out after school so instead I kept to myself and read. It was my freshman year of high school when I checked off three months of not talking to anyone outside of school besides her."
It was nearing the end of the first session and besides forming the frame of therapy with the set weekly time and day, I continued to stay almost solely in the information gathering mode. By doing this, I stayed with Charlie as I let her know what she could expect from me and that she could refuse to provide any information she did not want to at any time by just telling me no. I assured her that the fact that she didn’t want to discuss something was enough of a reason to stop. During a pause in our dialogue, I wanted to tell her she was brave, that it wasn't too late for her to live life with happiness, but the immediate therapeutic silence won out.
Two reasons prompted me to keep my encouragement unspoken. Even though my optimism was sincere, I had no idea of how to create a plan of action for her, nothing specific on a clear behavioral goal level to point to as a potential defining path. Also, “I ran the risk of her perceiving my optimism as evidence of my failing to appreciate the magnitude of her pain”. The timing was off as what was relevant in that moment was that she endured hardship and was hurting and wanted these two points acknowledged without any competition. I was the port in the storm, and I was acknowledging her pain. Regarding adding anything more, this was one of those times when more would he the enemy of good.
Once we were there with the sadness of her early life out in the open, something shifted in Charlie, and she began testing me by admitting to a problem and then pelting me with a personal question. First, her voice inched up a register and she said, " I've never had sex. Not until three months ago when I met…his name is Daniel and he is not available. I knew he was married but I hooked up with him anyway. You would never do anything like that, would you?"
The way she stared at me in that moment I knew she wanted to see if I would judge her and was also letting me know that she was not afraid to shift focus and put me on the spot.
"You know, I can't really delve into my personal life, Charlie, but I’m curious. What makes you so sure about what I’d do? What makes you so sure that when or if faced with a mirage in the desert at a time when I’ve reached a breaking point, I might not try to drink the water?”
The staring continued but was now accompanied by silence.
“Look, I get it,” I said. “Sometimes the world makes professional therapists out to be mascots of all that's socially ideal, when in reality, I may be just as isolated as you. And capable of making similar choices."
"Sure, you are," she said, settling her gaze on my diploma on the wall.
“Was Dan…” I stopped myself for a second. I wanted to ask about Dan, but not have her feel defensive or think I was trivializing, “can you tell me about him?”
“I can’t. He’s a father, husband, son, best friend, author, researcher, gym rat, middle class. Cute, more than handsome. He needed braces and never got them. I can’t talk about him any more than that. Oh, except he’s my co-worker on certain projects we work together.” She was being vulnerable with me. “She was sharing something that hit on such a universal theme: unrequited love” of sorts. I saw an opportunity to bridge the gap between her and the general public by my relating. Since I was the mascot for the public at large, if I related, it would be a start to her being less removed, separated.
“Charlie, there are many things I would do differently if given a second chance. It sounds like we may have that in common," I told her. “And you have this is common with so many women and men”, I wanted to say, but didn’t for the sake of being too much the salesperson for society at large. She sat quietly. Then leaning forward, she said,
"Well, I hope you're nicer to yourself."
With that her eyes grew soft and she gazed at me with friendship. I chose not to hit any more balls back to her at that point. Instead I smiled, and told her, “Thanks.”
Being Both Therapist and Client
For her second appointment, Charlie sat again with hands folded and posture strong, and then began the session by telling me that my arms were again crossed, and I seemed like I didn't want to really talk with her. This test, I thought, may have been an attempt to obtain reassurance that she hadn't overshared at our last meeting. Perhaps she also needed me to know what it felt like to be evaluated, in case I was doing a similar thing to her. My reply, I decided, would be measured kindness, but I needed her respect too. Instead of saying "my guess is you're scared, but I promise, I'm safe,” I went with what felt like cliché boundary setting 101.
"You seem concerned about making sure I'm really interested in talking with you. I'll confess, I tend to be on the cold side temperature wise, you may see my arms crossed at times."
I decided then that giving her the overview of early therapy would be better than either continuing to spar or immediately picking up with what she said last session. I did this because I was concerned the deep, candid disclosure she made last time might be a sort of self-sabotage whereby she made herself too uncomfortable to return, while at the same time getting some small relief by having shared. She might even see my bringing any part of this disclosure up as challenging or even shaming. In other words, way too soon for the soufflé!
I kept going. "Now, it's time for us to get to recent history. Probably like your field, which I know next to nothing about, we need to create a baseline and the first step is getting all the remaining important information out on the table."
She looked frozen and I grew concerned that at any moment her critical parent persona would return to challenge me. So, I quickly continued. "Recent-history is an oxymoron. It's a phrase to encapsulate my question of what life is like for you. In the back of my mind at this point, is the question of why decide to meet with somebody now?"
She didn’t move and didn’t answer me for what might have been a full minute. Finally, she said, "Do you like to get lost in all these little lives around you or just dismiss them by the time you leave?"
"Ouch, wow." I said.
I resisted my own people pleasing tendency—the residue from my own family of origin-—and just sat there, with my eyes as expressionless as possible. “I wanted, in that moment, to address her need to matter”. I did my best active listening pose and moved slightly forward, leaning in to communicate non-verbally without looking overly deliberate, like a perched egret.
She stepped up.
"I had to take a shower to come see you and it was the first shower I took in days. After my co-worker ended things, I started drinking at night. Every night. He would call all through the night and the next day saying he was worried about me, but that I had to stop calling him and that he could no longer respond. I don’t remember any of my calls to him, but he once sent me a call log. He disconnected our private phone line, but we still talked at work. To get through it I made myself more available for the bigger overseas meetings and wound up spearheading our entire overseas communications. Others have the in-person meetings, but everything starts and stops with me. That’s how everything at work changed. I now only work from home, with little exception. My world is my phone and computer. I have no time to eat or bathe. I hardly go to the bathroom. But I always walk Yoda."
“Her dog, Yoda was her love supply and a reminder that kindness existed in the world”.
I took a deep breath and but before I could exhale, she continued, "So now you have the following: alcoholism with blackouts for over six months, so Alcohol Dependency on Axis I, abandonment by father, then death and bereavement, oh, emotional incest is missing in the DSM, clinging relationship with obsessive features with anger outbursts, I'm saving that outburst detail for next session, so, that gives us a rule out of BPD, attachment disorder, co-dependency and intermittent explosive disorder on Axis II. There. I laid it all out for you. And I'm sorry."
While some of her diagnostic summary was surprisingly on point, I did not want to discuss that. She next told me she was valedictorian of her doctoral class at one of the top ivy league schools and studied psychology for her electives. In a way it seemed like she wanted to impress me. In another, it was possible she was fearful of her own problems.
"What are you sorry for?"
She paused for a moment. Therapeutic silence sometimes feels so long.
"I guess I'm sorry I'm here."
My interpretation was that either Charlie concluded that based on my young age I would find working with her overwhelming, or she liked me and felt guilty for bringing in “darkness.” Maybe a combination of the two. She was used to being smarter than everyone else, being the one with the information as opposed to the one seeking it. I told her that for therapy, she was doing exactly what she was supposed to be doing—albeit in a much more organized manner! She allowed us this humor and laughed out loud. I told her about the multi axis of 1-IV and how it is the format for putting everything together to map out a problem and solution. She didn’t chime in about being familiar with this. I continued by saying that I'd like to develop this together with her in session.
My goal was to take away any perceived armor she may have assigned me and by unmaking the work, she would feel safer. I described the importance of ruling things out and stabilization. Those two terms would be the focus before anything else. I didn’t want to go right back into what she said about wanting to die because I wanted her to tell me electively. We spoke about the hierarchy of her more negative circumstances and when I asked her which was the riskiest in her mind, I was prepared for her to face alcoholism in tandem with her upfront style.
"Oh, probably that I am very suicidal at times."
Suicide Enters the Room
I tried not to appear shaken and went into question mode to assess suicide risk. With each new question I tried to communicate care without sounding patronizing.
“Can you tell me what that’s like?”
Long pause.
“Do you ever think about how?”
Long pause. It would not have surprised me if she knew about passive and active ideation, but I didn’t want to get into an intellectual conversation, so I did not use those terms or ask.
“No, just that I want quiet and then I drink and take Yoda and go to sleep.”
“Does anyone in your life now know or even have hunches about your pain? ”
“My best friend, my one friend who I’ve known since undergrad is a psychologist in Beverly Hills. She’s like family and I consider her, her husband and sons my cousins.” She then started laughing.
I wanted to bring things back to my questions about safety but knew that would be too schoolteacherish.
“Something about her work in Beverly Hills always makes me laugh. We don’t talk as often anymore. Southern California gets crazy.”
I let the rest of the session go towards her friend’s work and the “imperfections” of the people of Beverly Hills. She seemed to enjoy this.
The next session, Charlie was ready to focus. She painted a picture for me of her day-to-day life: wake up between six and seven a.m., brush teeth, splash water on face, walk Yoda or let him out in the backyard, feed Yoda, sign in online, make coffee, take out a frozen something to microwave. The next few hours would be a blur of vomiting, coffee, mild level of shakiness, combined with conference calls, emails and other various computer-based tasks. Then after Yoda's second trip outside and a few hours post-lunch, she would begin drinking vodka. Sometimes in Diet Coke, sometimes straight. She would do this slowly while still working all through the night. Voice communication typically ended completely by 2am. At this point, her drinking continued and eventually she would "wind up in bed" after a shower, energy permitting. Occasionally, she had visits by phone with her cousin in California.
“I kept thinking, "start where the client is at."” Because I was not hearing about deliberate self-harm on a planned or immediate level, self-care became my target pitch with Yoda at the center. If I pointed out that I was concerned about black outs, the level of her drinking, the level of her depression, she would have shut down, possibly discontinued and perceived me as a critical parent. I would wait for just one or two more sessions.
"You want to be around for Yoda. She's dependent upon you, right? I'm not out to preach sobriety. My goal is to help you get what you want and for you to be happy—or at least feel less pain. But, I need your help on this.” She gave me a look that indicated an inner reply of “bull” and so I added that her drinking is risky and dangerous and that seeing what she wants in her life, such as caring for Yoda, is a step towards sobriety because it would be a by-product of it.
She responded by shifting away from the here and now and going into her teenage years with her mother, when she would read her schoolwork to her mother, working to get an eventual smile. This would be followed by cooking dinner, cleaning up, watching TV with her mother and helping her into bed. Often, her mother would wake her during the night in tears and she would do her best to comfort her.
“I would pretend that my mother had pneumonia and my father was stuck working late.”
“So that made it a more comfortable situation. Very resourceful and creative. You worked with what you had.”
“I got good at creating alternate circumstances. I did this when I made my speech to our graduating class. I pictured myself as a scientist wishing them well. I had no family in the audience.”
I did zero redirecting and just let her lead. Eventually she paused, looking sad.
"Is it me, or does it seem that I have more to deal with than most people?"
I nodded, "You have been through a lot and pain is the by-product. And you're still here."
"So, what does that mean?" she asked, her eyes boring into me.
"It means you can give" —ugh! beginner's mistake—better to have asked her what it meant for her, but too late to shift. “You can give love to Yoda, to your cousin. To the world you live in and are part of.”
"Oh God, you're one of those people," she laughed.
Our time was suddenly up and despite the bomb she’d dropped, she left my office a little bit happy.
I hoped at this point that the therapeutic alliance, combined with Yoda, seemed enough for the time being to compete with any desire to die. My experience at that point of working with suicidal patients was limited to practicum work in a residential facility, where supervision of the patients was constant. On the one hand, my assessment was that her ideation was passive, and she was not at risk of intentional self-harm. On the other, she could possibly hurt herself unintentionally while under the influence of alcohol, or her tolerance for her pain could escalate along with a decrease in impulse control, making it tempting for her to torment herself. My next worry was along the lines of “who was I to determine such a thing?” I was afraid to trust myself, but at the same time, if I continued with that thought process, I would not be able to do my work at all. I needed to permit myself to trust my instinct. “I white-knuckled it until she returned for her next session”, convincing myself in the intervening days that she’d just need to avoid alcohol clumsiness or an impulse emotional reaction to something, such as a conference call where Daniel was a participant. Thankfully, none of that happened.
I did not disclose my concerns because I did not want to seem controlling, but in hindsight, this would have solidified my role as a professional and communicated care. A novice mistake, I wanted her to see me as an ally or possibly even a friend on some level, though I was not aware of this at the time. This personal state of mind may have interfered with expressing my concerns directly at that time.
Atypical of my work style, I placed stability and structure as the focus of the initial sessions and her life, while not touching the alcoholism-in-the-room. I was afraid that if I tried to finesse recovery beyond minimal references to it, she would terminate therapy. It seemed to work. Charlie made every meeting with me and was actively engaged in her therapy. I’d asked her to try expanding and deepening her support network and she tried. We talked about developing a curiosity of others and using this a fuel for practicing casual conversation. She reported more conversations with her cousin in California and she stopped and chatted enough to get on a first name basis with a couple of her neighbors whom she met while walking Yoda. My plan was for her to achieve a set routine of basic self-care, physical hygiene, and an emotional hygiene of having a “no fly zone,” where she dedicated a set space and time to be work-free, even if just a half hour in her living room. From this, we’d then work on social hygiene—a routine interval of basic conversation with neighbors or others. Once these forms of care were in place and working with me was more familiar, then the odds of a conversation about alcohol being productive were greater.
“But then one day this optimistic effort all came to a screeching halt”. Her drinking escalated once again after Daniel began refusing to answer even her work calls. She had been redirected to a new administrator every time she tried to speak with him. Sessions were never the same. Her depression was escalating and riding right along with it was active suicidal ideation. She attended therapy without fully emotionally attending. She had this blank stare and even left early a few times, telling me she needed to go. I increased her sessions to twice a week, and to my surprise, she complied, no longer leaving early. Her disheveled look returned and gone was the new ponytail and barrette she began wearing just a few sessions ago. I felt like I was watching a flower shrivel up in anticipation of the inevitable. I wished she had better care than what I was providing, to then have better results—less pain. I knew referring her out would be seen as abandonment. I also knew she had made progress.
Though she kept showing up, she was becoming more and more zombie-like in sessions. One day she had a mark on her cheek, but shrugged her shoulders when I asked about it. It matched dark circles under her eyes. Next I asked about her drinking and got the same shoulder shrug in response. And then I asked about wanting to live. Void of emotion, she shook her head no.
"But what becomes of Yoda?"
"I'm thinking about taking her with me."
That's when I knew I needed help.
I asked her to help me understand what that meant. She said that was a “nice try,” but that she had already said too much about it. She then said that she “must leave” but would be back for her next appointment.
The Ground That Was Gained
After Charlie left that session, I broke her confidentiality by speaking with the psychiatrist from her company’s HR network. I had a release from her original paperwork and did not mention this to her at her next appointment. She sat down, looking slightly more rested. I told her she needed intensive treatment and that residential detox and weekly group therapy were my minimum requirements for us to continue working together. She refused and tried to talk me into keeping things as they were. I terminated our work, making it clear she could contact me any time after completing the two requirements. She denied any ideation during this last session.
I felt a combination of self-serving relief from a challenge being taken away from me, second guessing what else could benefit her right then as some sort of discharge plan, and some faith that she had an inner resilience.
To me, this was not a complete failure because, in my experience, people never lose the ground they gained while in therapy. They may disregard it, but the experience of having learned cannot be deleted—it happened, learning happened. I knew this logically, but this was sad for me. The magnitude of her suffering, the factual collective meanness in her experiences of the world, felt sad to witness. I wanted to alter it, or rather, have her alter it, and for me to be able to provide what was needed to empower her to do this. No matter the logical argument that some progress was made, pain won that day. I felt sad, scared for what she might do—but I did believe she would survive. I questioned my motives—did I want to end the risky work for my own benefit? Though she could make it less risky with compliance. In a way, I did feel some relief, but not enough to acknowledge at the time.
Epilogue
Five years later, the mystery of what happened to Charlie would be solved quite by happenstance, when I ran into her on one particular sunrise. We literally crossed paths as I was headed to my car after a run. Charlie seemed happy and calm. She was walking her dog, a new puppy she introduced as Chewy, and told me she was married to an artist. We briefly joked about the unofficial pre-sunrise running/walking community. With the laughter in place, I smiled and said it was good to see her, and resumed my morning activities. I wasn’t able to grasp the meaning of that encounter at that time beyond an intellectual level. The significance was that this was someone who once wanted to die and now was walking her puppy, happily married and healthy in appearance.
I’ve thought often about the weeks it took for Charlie, someone so successful and yet struggling so much, to express her suicidal feelings to me. Since suicidality has an aspect of masking, it is only natural for a client to keep it hidden at first. We therapists get it—why would someone who feels so little power be eager to turn over the one thing they have control over? And to a stranger, no less? It makes sense that they’d feel it might be too early to know what this relative stranger would do with the information.
But then, what can we really do once a patient does make the declaration? Yes, we can thoroughly access the ideation. Is it active or passive? Longstanding or reactionary to something recent? If active, how likely is the plan to be attempted and, if passive, how likely to progress to active? But really, we are just people, with our own subjective views, painful memories and blind spots.
We have the capability as therapists to gain entry into our patient's lives, learn the particulars of how they see themselves, who they want to be, what they want in life, what they see as impasses, how they feel. We are given access to the personalities and relevance of spouses, partners, exes, family, friends, co-workers and neighbors. We offer validation to people who feel misunderstood. Sometimes we help them to connect the dots, making what feels confusingly fragmented into related parts that share a pertinent life-theme. We do this by offering clinical explanations for what they describe as struggles, helping them see the relationship between what they are experiencing and their own internal motivators. At once we are both the motivational cheerleaders and the "Keepers of the Gloom" (borrowing from Robert Plant). But at no time are we mystical fortune tellers and at no time can we clap with one hand. “When it comes to suicidality, we aren’t the only link to staying alive”. We’re one in a chain of a system of care that’s there not just for them, but for us too.
In retrospect, I told myself that breaking Charlie’s confidentiality those years before was supposed to feel like being clinically responsible. Despite my direction, at that time, I felt like I was some kind of a turncoat traitor, even as I was dialing. After some exchanges and being transferred, put on hold and transferred again, I was trading information with the director of human resources for the entire company. He was a clinical psychologist who had an Ivy league quality. From my Philly background, I placed his accent as having a familiar quality, from what I always saw as the “other” Philadelphia, and I later learned that he was adjunct faculty at Penn. I gave him a full overview of Charlie, her progress, her impasse and the status quo. I felt a phone version of “active listening” and from his prompting, I felt comfortable continuing. He continued to ask questions that encouraged more information from me. Finally, I had said it all. The specifics of what he said escape me now, other than one surprising thing. He said that he thought I would benefit from looking at why I accepted this case in the first place. His direction felt like it should feel uncompassionate, but it did not, rather it felt sincere and matter of fact. Surprised, sad, somehow oddly feeling vindicated, I thanked him for his time, and without asking the actions he would take-or not take, we ended the call.




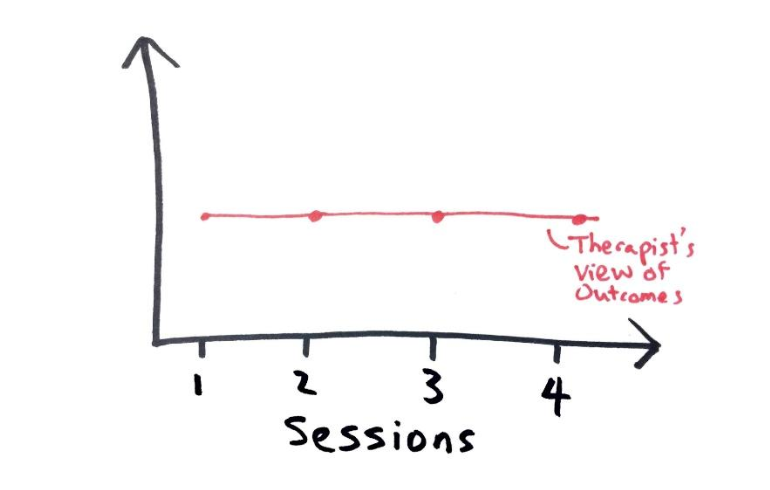
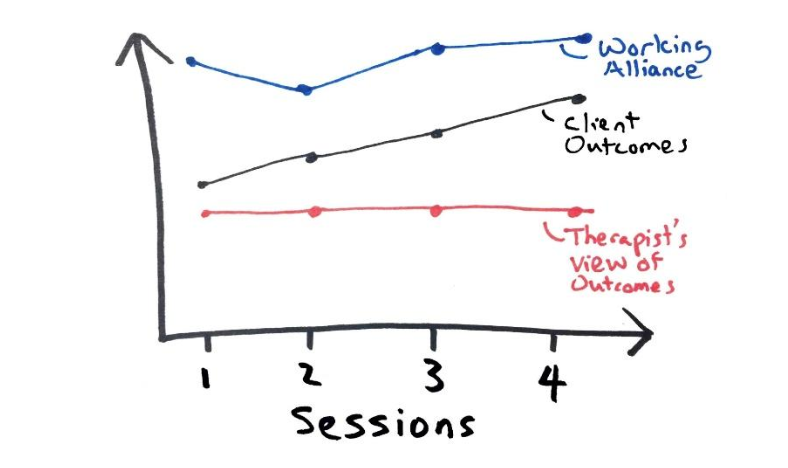




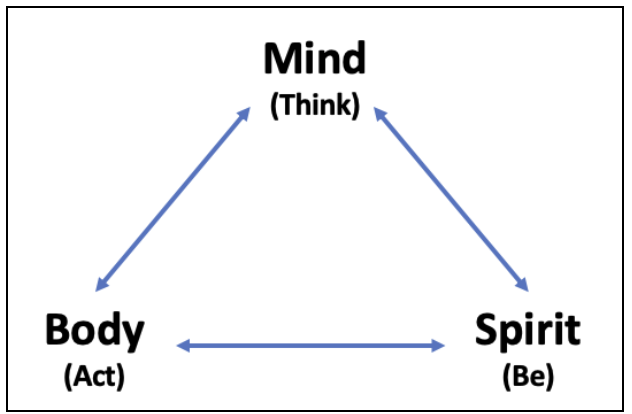 When I’m working with clients I often ask myself which of these paths might be most helpful to them at this point in their treatment.
When I’m working with clients I often ask myself which of these paths might be most helpful to them at this point in their treatment. We also worked toward taking care of tasks around the house that he’d been putting off and on building positive interactions with others since his relationships had suffered. Given his health challenges, we worked on ways to improve his sleep and eat more healthfully.
We also worked toward taking care of tasks around the house that he’d been putting off and on building positive interactions with others since his relationships had suffered. Given his health challenges, we worked on ways to improve his sleep and eat more healthfully.
