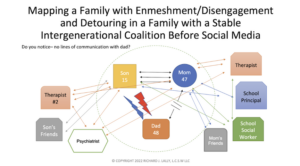
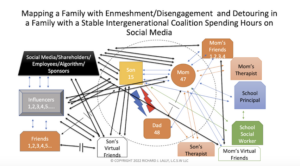
Case Background
Samantha, a 15-year-old African American young woman, was referred for psychotherapy by the hospital where she was taken after she was gang-raped while passed out at a party after drinking more than she ever had. This is Samantha’s first ever outpatient psychotherapy session, and she finds herself experiencing disorienting and, at times, overwhelming waves of depression and hopelessness as well as dissociative fugue states. Trying to calm herself, Samantha also finds herself involuntarily scratching at her arm and sucking her thumb, both of which give her a comforting sense of emotional and physical numbness.
Samantha’s friends describe her as a beautiful, kind, and honest person with a great sense of humor, an A student, and a star athlete. Samantha attends an exclusive private high school on scholarship; there, she is one of very few students of color. Her dream is to get a scholarship to an Ivy League university. When not studying or on the lacrosse field, she volunteers to help children and families in need in the community and for human rights causes. Older boys have frequently asked Samantha out, but she has never agreed because her parents are strict about dating and don’t want her to get entangled in a romantic relationship and lose her focus on college.
Samantha’s family lives in urban public housing, where drug abuse and community violence are common occurrences. When she was 10 years old, Samantha witnessed her older brother, Andre, get shot and killed. He was walking her home from school, and they were caught in the crossfire of a gang fight. At the time, she didn’t understand what had happened when he suddenly fell down and blood was all over the sidewalk around him. She tried to get him to wake up and get up, but he wouldn’t open his eyes, move, or speak. She remembers neighbors taking her home and her mother screaming and sobbing when told that Andre had been shot. Samantha recalls that her mother “never was the same” after that; She wouldn’t go out except to go to work and return home.
Samantha frequently found her mother seemingly in another world, sobbing and saying, “My boy, my boy!” After the shooting, Samantha’s father also started drinking alcohol to the point of intoxication several times a week. Samantha has learned to stay away from him when he is drinking because he changes from being a loving and kind man to an angry and violent person she doesn’t recognize.
Samantha’s parents kept their jobs; They worked long hours and encouraged her to get scholarships and do well in school and sports. Samantha feels very grateful but also guilty that her parents are stressed and working hard while she seems to be enjoying school and sports in a sheltered school setting. Girls in her neighborhood, though, call her an “Oreo” (because she is Black, but they see her as trying to act like a White girl) and have stopped being friends with Samantha.
At school, girls pick on the way she speaks, saying she sounds like a “ghetto girl,” and that she only got into the school because of charity or government handouts. She has a solid group of male friends but sometimes feels like she doesn’t really fit in with the other girls at school. Girls are also jealous of her because of the attention she gets from boys, which has made making girlfriends even more difficult. She has one close female friend, Lily, who is also on the lacrosse team.
At the end of Samantha’s junior year, after she had aced a very difficult AP (Advanced Placement) chemistry exam, Lily convinced her to go to a senior summer kickoff party. A graduating senior, Jack, who had been asking Samantha out since she was a freshman, was hosting the party and wanted both girls to come. After prodding from Lily, Samantha decided to “let loose” for one night and attend the party. Samantha told her parents that she was sleeping over at Lily’s. Jack made a big deal of Samantha’s being at the party and offered to “grab drinks.” Although he was enthusiastic, Jack had always been friendly and had never been aggressive in his pursuit of Samantha. Samantha had only experimented with alcohol, but she wanted the full party experience, so she decided to “go for it.”
Samantha began by slowly sipping on a drink, but then got pulled into a drinking game with Jack and his guy friends. She quickly became intoxicated. Jack asked her if she wanted to go somewhere quiet to talk, and Samantha agreed. Jack helped her walk precariously to his bedroom, and the moment she sat on his bed, Samantha passed out. Realizing that she needed to be taken care of, Jack went to find Lily. This took quite a while with the raucous party spilling over into all parts of the house.
When Jack and Lily returned, they saw four very intoxicated guys nervously coming up the hallway from the direction of Jack’s room. When Jack and Lily entered the room and turned on the lights, they saw Samantha sprawled out and mostly undressed on Jack’s bed, still unconscious. Lily called an ambulance and Samantha’s parents.
Samantha woke up in a hospital room with Lily, Jack, her parents, and a nurse. “What happened?” she mumbled. “The last thing I remember was being with you, Jack. Something’s wrong. I feel all numb but like my body’s been run over by a truck. Did we get into an accident?” The next several weeks were a nightmare for Samantha, and for her parents and friends. She felt depressed and scared because she could tell she had been assaulted, but she had no memory of it.
When she met with a sexual assault counselor working with the police and learned that one of the boys had confessed and that she might have to go to court if criminal charges were pressed, she felt terrified and like the whole world would know she was “dirty.” The sexual assault counselor got her an appointment with a female therapist who worked with girls and women who have been sexually assaulted. Samantha delayed starting psychotherapy for several weeks by canceling several sessions. Her parents finally insisted that she talk with the therapist and drove her to this, her first, psycho-therapy session.
Session Transcript, Annotations, and Commentary
After the annotated session transcript, I present a summary of Samantha’s observations and reflections on her experience in the session. Following this summary is commentary highlighting key themes and take-home points for handling this or similar crises, and questions for reader self-reflection.
THERAPIST: So, Samantha, tell me a little bit about you.
SAMANTHA: (Stares at her lap) I’m in school.
THERAPIST: Mm-hmm.
SAMANTHA: (Still looks down but glances furtively at the therapist) And I’m into my senior year. I like to play volleyball.
Therapist’s Inner Reflections: Samantha seems very withdrawn and in a lot of pain and emotional turmoil. She looks haunted; there’s definite fear in her eyes, and she’s glazing over and just barely holding it together. Looks like she’s heading for an emergency and a breakdown. I want to help her reorient to the present, so I’ll engage her in focusing on who she was before the rape with an emphasis on her physical self so that she can become more aware of her body and slow down the flood of ruminations that she appears to be experiencing.
By orienting to the strengths and abilities she had—and still has—this can help her do an SOS [as discussed in Chapter 5, SOS refers to slowing down and sweeping her mind clear, orienting to a thought that helps her feel safe, and self-checking stress level and level of personal control] and begin to feel more personal control despite the intense distress she’s feeling. I’m not going to introduce the SOS formally to her because that would seem too didactic and intrusive, but I can help her do an SOS and begin to focus herself by showing an interest in her interests and strengths.
THERAPIST: Excellent. I know that you know this—I met with your parents a little bit before you, so they told me that you have been a great athlete for a while. So, volleyball is now your favorite sport?
SAMANTHA: (Hunches over, looks at her feet, no longer glances at the therapist) Uh-huh.
THERAPIST: Excellent. Wonderful. Okay. And, um, I also know that things have been rough the past 3½ weeks . . . and that’s why you’re here today. So, I want you to know that—that we can work on this, that this is actually gonna be, um, a little bit hard at the beginning, but I know that you will—we will figure out ways that you can really overcome this terrible thing that had just happened to you. I’m sorry. So, because you’re a good athlete, I know that you work hard . . .
SAMANTHA: (Relaxes slightly) Mm-hmm.
Therapist’s Inner Reflections: I’m not going to ask her to tell me what’s triggering the distress for her because that probably seems obvious to her (even though it’s more complicated than she fully recognizes). By acknowledging the trauma in general terms, I’ve signaled to her that I do recognize what’s triggering her but that I’m not going to dredge up what’s happened or how she’s feeling because she’s probably trying very hard to not be aware of the shame and betrayal that I expect she’s feeling—and to not think about the rape, even though she probably can’t stop having intrusive memories, especially because she was not conscious while the rape happened. For the sake of Samantha’s sense of security in talking with me, which is very new and fragile — with this being our first session, the betrayal she’s experienced, and her damaged sense of self and efficacy—I’m going to emphasize her ability to accomplish difficult goals at this point.
THERAPIST: . . . and also your parents told me that you are a very good student, too.
SAMANTHA: (Looks up tentatively) Uh-huh.
THERAPIST: You have worked for—for everything that you have now. Right? And you really just have to finish your senior year the same way that you have, you know, have worked so hard your whole life to be where you are. So, your parents are telling me that they are concerned because you’re not going to school. Hmm. That has been really hard on you.
SAMANTHA: (Looks at the therapist, then down) I just don’t feel like going to school anymore.
THERAPIST: Mm-hmm. Yeah. So, tell me some of the reasons why you don’t want to go to school.
Therapist’s Inner Reflections: I’m sure there are many reasons that may seem obvious to Samantha, but I’m asking her to support this shift she’s just made from being passive and numb emotionally to being able to actively express her point of view. She’s engaging, even though the first signs are anger. Let’s see what more specific triggers she recognizes.
SAMANTHA: (Looks directly at the therapist, eyes blazing) I don’t wanna see certain people. (She sits back, strokes her ear reflexively with one hand, and sucks on the thumb of her other hand.)
Therapist’s Inner Reflections: The distress she’s feeling is intense. I see her doing several forms of reflexive physical self-soothing to tolerate the distress. As she does that automatically, she could put herself into a dissociative trance. I’ll support her intention of self-soothing and see if I can gently help her to do it consciously and to access other forms of self-regulation as well so that the self-soothing doesn’t lead to a dissociative shutdown.
Dissociation could lead to the healthy self-protective and self-assertive anger she’s understandably feeling to leak into her self-soothing in the form of unconscious or barely conscious self-harm. I’ll start by returning to the first part of the SOS: helping her focus on her breathing and being aware of her body.
THERAPIST: Mm-hmm. Mm-hmm. Okay. It’s hard to, to see some of your friends or your acquaintances? And now I can see that it is really hard, Sam, to just talk about this. And I can also see that your body is telling you that probably right now you need to be soothed. So, one way of doing it, and I bet it’s helping you, is by touching your ear—yeah? And sucking your thumb. We can explore other ways that can also be helpful. Can I show you some other ways? (Samantha nods.)
THERAPIST: So, let’s try to focus on your breathing, Sam. Can you breathe for me deeply? Can you feel the air coming in from your nostrils? Can you do it maybe one time? Can we try another one? (Samantha looks down and begins rubbing and then scratching her arm.) This is too hard. This is painful. Is the scratching helping you? Hmm. Can we explore other ways, too? (Samantha stops scratching her arm and instead rubs it more slowly and gently. She begins to tap her feet vigorously.)
So, I can see that you’re moving your feet. Can you feel your feet on the floor, Sam? Yeah? Can you tell me if your feet are warm or cold? Yeah. Let’s try to keep on moving your feet. Keep on moving them. Yeah. Can you move your other foot? Yeah. Alright. Can we breathe a little bit more? Let’s do three times this time. Okay? One . . . two . . . three.
SAMANTHA: (Shifts from rubbing her arm to scratching with increasing intensity; begins to hyperventilate.)
Therapist’s Inner Reflections: Samantha’s escalating into emotional dysregulation and what looks like a dissociative state. Helping her to relax may be unintentionally leading her to lose track of her ability to self-regulate, I need to stay with the focus on body awareness but step up and gently but firmly guide her with very specific small steps to doing so without hurting herself.
I think she needs to see what I’m talking about, both to be able to cognitively process what I’m saying and to reorient herself to being present and not alone but supported by me. I’ll keep the focus on her being in control of herself so that she doesn’t experience me as taking control away from her in the way that those boys did by sexually assaulting her when she was unconscious.
THERAPIST: And, instead of scratching, can you touch your other hand and your arm like this? How does that feel? Can you feel your arm? Can you feel your wrist? Yeah? Keep breathing. You’re in a safe place, Sam. Nobody’s trying to hurt you here. Okay. I like this. Do you feel that your body likes it? When you try to soothe yourself like that, how does it feel?
THERAPIST: (Samantha gradually breathes more slowly and deeply with a more relaxed torso and legs.) Nice.
Therapist’s Inner Reflections: As Samantha calms down and comes back into the room, I can feel the tension draining out of my body as well. I’m primarily focused on Samantha, but I’m noticing that it helps me personally to self-regulate by doing these simple self-awareness actions along with Samantha. Now I can help Samantha not only feel calmer but also safer and protected. I’d like to give her a hug myself to comfort and reassure her, but I know I’m not her mother (even though I’m thinking about my daughters and wanting to hold them when they’re upset or hurt), and she needs to know that no one will intrude on her in this therapy. So even through it seems kind of silly, it makes sense to help Samantha to hug herself, and she’ll know that I am contributing to that hug without intruding on her personal space in a physical way that could feel like a replication of the rape (and her brother’s murder).
THERAPIST: Nice? Alright. Have you ever given yourself hugs? No? Sometimes I give myself some hugs. Sometimes that helps me. Try it—maybe not here but later on. Okay? I’m wondering, you know, how we’re gonna find ways that soothing yourself is going to be part of your daily routine, and, at the same time, you can soothe yourself and only you will know that you’re soothing yourself. Alright? So, we did that sort of breathing a, a little bit of deep breathing, so you know that you’re breathing deeply because you want to focus on the here and now, putting your feet on the floor and making sure that you know that you’re feeling it, feeling your hands. Right? Feeling different parts of your body and focusing on, you know, where you are.
Therapist’s Inner Reflections: If I help Samantha connect these simple breathing and body awareness actions with her athletic skills, that can make this something she can do intentionally both to reduce the intensity of her hyperarousal and to tap into her self-confidence. And I will emphasize the core goal of keeping herself safe, which is what she feels she and her friend (as well as the boys who perpetrated the rape) failed to do. Then I can link the goal of being safe to her withdrawal, which is a problem and a symptom of depression because it keeps her trapped in survival mode but also is an adaptive attempt to protect herself.
THERAPIST: Okay? It’s almost like playing volleyball, you know? I bet that you’re so good at volleyball because you are actually practicing, and when you practice more and more, you get better and better, right? So, it’s the same thing here with our emotions. The more that we try to stay in the here and now, the more that you’re gonna feel a little bit safer. Okay? And, so, the more that you feel, you know, that you are in safe environments like—I bet that you’re spending a lot of time in your house right now. Is it—is your house a safe place for you? Does it feel safe? (Samantha nods.) Okay.
SAMANTHA: (Continues to visibly relax; makes tentative eye contact with the therapist) Yeah, it does.
THERAPIST: Okay. Are there any other places that are—make you feel safe? No? Only your house? Okay. Alright. So, tell me a little bit about what would going back to school look like. What do you think that you need in order to feel calm, in order to feel that you can soothe yourself utilizing healthy ways so you can go back?
Therapist’s Inner Reflections: Samantha now is associating the main goal of safety with calmer body feelings that represent a main emotion (feeling “nice,” which seems to mean that she feels a sense of peacefulness emotionally) and a main thought (that she is not trapped in horrible distress but has active ways to enable herself to feel better). With safety as a main goal that can organize her complicated emotions and thoughts, we can begin to explore her options for achieving the goal of protecting herself (and the related goal of returning to school and resuming her life and progress toward future goals, such as success in school and sports).
SAMANTHA: I have my best friend.
THERAPIST: Mm-hmm. Your best friend. So, tell me, what is your best friend’s name?
SAMANTHA: Lily.
THERAPIST: How long have you known Lily?
SAMANTHA: Since high school started.
THERAPIST: Okay. Since freshman? Wonderful. So, you’ve known her for 3 years now?
SAMANTHA: Yeah.
THERAPIST: Okay. And you can trust Lily? Has she been contacting you? Yeah? So, has she been supporting you these past 3½ weeks? Yeah? How does she support you? What is she doing to help you?
SAMANTHA: (Smiles shyly) She’ll check up on me like every day or so.
Therapist’s Inner Reflections: Samantha is such a resilient young woman! Without my bringing it up, she went right to what’s probably the single best way to begin restoring her sense of relational security, which had been shattered by her friend Jack’s neglect and the other boys’ betrayal and exploitation.
Samantha is a little fearful of trusting that her best friend Lily won’t also let her down or even reject her, but she can see that her friend is standing by her. The sense of being cared about and valued, and watched over in a helpful and nonintrusive way are clearly crucial for Samantha’s recovery. I’ll explore that as a potential path forward for her.
THERAPIST: Mm-hmm. Mm-hmm. Wow. So, is she actually contacting you quite often? Yeah. Alright. Have you been able to keep up with some of the work at school? No?
SAMANTHA: (Shifts back to a tense fetal-like position; withdraws eye contact) No.
THERAPIST: Alright. Okay. Is that something that you would like to do? Yeah. Okay. So, you’re a very brave young woman who has gone through a lot, and your body is very wise and knows how to calm and soothe you. So, I’m wondering if, for next week, maybe you can visit your friend Lily at her house before next week and see how that goes? Would that be something that you are willing to try? Is that something that you think that you can do?
Therapist’s Inner Reflections: That was a mistake and a close call. I jumped ahead by implying that I was urging Samantha to go back to school. I got caught up in the relief that Samantha (and I as well) was feeling when focusing on the security that her friendship provides. I’m glad I caught that by noticing Samantha’s nonverbal signaling and stepped back to suggest a much more manageable first step of just going to the friend but not facing the much larger set of stressors and triggers that she’ll encounter when she returns to school. One step at a time. I’ll help Samantha build a behavioral chain of small steps that can help her reengage with her relationships and her particular areas of strength and success: schoolwork and athletics.
SAMANTHA: (Looks thoughtful, determined, and then makes eye contact) Yeah.
THERAPIST: Okay. Alright. And I’m also wondering if you can start talking with Lily about some of the things that you can start doing at home or maybe with her, some of the schoolwork, especially about the good subjects that you really like and enjoy? Is that something that you think that you might want to focus on this week?
SAMANTHA: (Continues uninterrupted eye contact) Yeah.
THERAPIST: Alright. And the last thing, Sam. I’m also wondering, since you are an athlete and you got this—right—I’m wondering if there is anything that you can do this week that can help you to maybe jog a little bit or walk fast or—or do something like that around outside—around your house, where you can . . .
SAMANTHA: (Nods and continues to make eye contact) Yeah.
THERAPIST: . . . do some exercise?
SAMANTHA: Mm-hmm.
THERAPIST: Is that something that you think that you can do? Yes?
SAMANTHA: Yeah. I can do that. Yeah.
THERAPIST: Alright. Well, I’m really looking forward to seeing you next week. Okay? Thank you.
Samantha's Observation
In a post session interview, Samantha said that she had been feeling that she didn’t recognize herself anymore and that her parents didn’t look at her in the same way as before. She was ruminating constantly about the party, berating herself for being so stupid and wishing she had never trusted Jack and his “so-called friends.” She had secretly started cutting herself to make the pain and shaking stop and sucking her thumb to comfort herself. In the session, she initially felt physically tense because she didn’t want to have to answer more questions from another adult about the assault and about how she was feeling and coping now.
She was surprised and reassured when the therapist was very gentle and accepting, but then she felt that she let down her guard and started to space out: “I kind of went somewhere else.” She felt extremely embarrassed when she realized that she had begun to suck her thumb in the therapist’s presence, but she didn’t know how to make herself stop. She felt a strong urge to hurt herself when the therapist brought up the earlier experience of witnessing her brother being killed. Samantha described having felt a sense of confusion and shock related to witnessing her brother’s murder that she realized was very similar to how she had been feeling about being assaulted. That realization helped her to understand why she felt unable to stop thinking about the assault: “It was another time when I was powerless to stop something terrible from happening to someone I cared about, and no one else protected them or me, either.”
Samantha emphasized that she found the therapist’s guidance to be helpful in enabling her to be “more in my body” and more aware of the present moment and surroundings. She found being able to be more aware gave her a feeling that she wasn’t powerless, that she could “take back some control.” She also felt calmer and safer, which was very different than the brief feelings of relief that she’d gotten from sucking her thumb or cutting herself—and she also didn’t have to deal with feeling ashamed of herself and embarrassed, which had been making things much worse for her emotionally.
By the end of the session, Samantha was feeling a small amount of hope that, with the therapist’s help, she could talk about the assault and her brother’s murder and figure out how to not feel so terrible that she couldn’t stop thinking about those horrifying memories. She also had hopes of figuring out manageable steps she could take to work toward returning to school and “getting back to having a normal life.”
Commentary
As the session unfolded, the therapist clearly was focused on three primary goals:
- building an alliance and instilling hope by interacting with Samantha in a way that was nonjudgmental, accepting, nonintrusive, and responsive, and that facilitated a sense of relational security, resilience, active problem solving, and hope for solutions
- assisting Samantha in regulating her emotions and becoming nonjudgmentally aware of the understandable emotional turmoil she was experiencing by identifying and adapting her intuitive ways of coping with memories and emotions, and supporting her by affirming, highlighting, and drawing on Samantha’s many personal strengths
- assisting Samantha in setting and emotionally committing to an over-arching goal that reflected her current concerns and that enabled her to organize her complicated emotions and thoughts in a manner that provided her with a path forward to restore the parts of her life and the aspects of herself—as an outstanding student and athlete, and as a valued friend—that she had relied on as a source of inner security, pride, and hope for the future
She also helped Samantha to orient (the “O” in SOS) by highlighting her ability and interest in sports. And she helped Samantha track not only the intensity of distress she was feeling (using body feelings rather than verbalized emotions as the guide) but also her sense of personal control (again using breathing and tactile self-awareness as a practical way to feel in control).
A common challenge faced when working with clients in or on the verge of crisis is establishing rapport and trust while determining how— and when—to best help the client disclose the memories and emotions that are causing severe distress. In the post session interview, the therapist confirmed that she was aware of recent traumatic events that had occurred for Samantha but did not ask Samantha to talk about those events. This signaled to Samantha that she could trust the therapist not to be intrusive, which was crucial in light of the traumatic violation Samantha had experienced and the many questions that she and others were asking her about what happened.
By alluding to the events, the therapist also was communicating indirectly to Samantha that it is important to consciously recognize the triggers that remind her of the traumatic events. In addition to simply being in therapy (which almost inevitably brings up memories), the therapist identified other key triggers, including going to school and Samantha’s experiencing distress in her body. Rather than inquiring about the specific triggering stimuli and circumstances, the therapist immediately focused on helping Samantha to respond to triggered distress with body awareness and breathing.
Doing so communicated to Samantha that conscious recognition of triggers does not mean that there is any pressure to dwell on or even talk about the traumas, the triggers, or both that elicit trauma-related memories. In this way, the therapist helped Samantha to recognize—rather than simply react to—current triggers for distress as well as the trauma-related memories. Samantha’s reaction of increased d










.png)