It’s morning. The alarm goes off, the coffee pot goes on, you decide what to wear, and ready yourself for the day. Consciously, but most likely out of your conscious awareness, you expect today will be similar to yesterday, and tomorrow will be like today. The day’s events may differ, but most likely the routine will be pretty much the same. There is comfort in that.
But suddenly something changes. When a traumatic event occurs, your world is no longer the same, no longer the safe place you could count on. It can feel as if the rug has been pulled out, everything is flying in the air and has yet to settle into place again. And as I will discuss, one’s internal world, one’s sense of self, also can feel dramatically off kilter.
Trauma and the Reproductive Story
Trauma, as defined for the diagnosis of PTSD in the DSM-5, is “exposure to actual or threatened death, serious injury or sexual violence¹. We often think of it as a one-time horrific event—a car accident, an earthquake, a shooting. But reproductive trauma, specifically infertility and/or pregnancy loss, is cumulative in nature. For most patients, by the time they set up an appointment with a fertility doctor or with a mental health professional, they have already gone through a year of “trying” to conceive, and multiple losses. As one patient put it, every menstrual cycle felt like a “mini-death.” And indeed, the losses that patients experience—of their hoped-for baby, their own adult development as a parent, their hopes and dreams for the future, of what we refer to as their “reproductive story”—significantly affect their psychological well-being².
Another way to define trauma, and one that fits with reproductive patients, is to think about infertility as an event that causes the disintegration, not just of a would-be pregnancy, but of one’s entire inner world. It affects every aspect of one’s life: feelings about the self, questions about one’s purpose, concerns about relationships—with one’s partner, friends, family, the world—and worries about the future—how does and will one fit in, what is one’s legacy, what is the meaning of one’s life? These are clearly not minor concerns. Trauma, in general, can be thought of as an event that overwhelmingly shatters core beliefs and assumptions³. For reproductive patients, the narrative that they once held, often as an unconscious guideline for the creation of their family, is no longer tenable as originally imagined. The core assumptions they held about having a family are demolished.
As a clinician who specializes in reproductive issues, I have heard a wide range of stories from women over the years, some of whom proclaim, “I always knew I wanted to be a mom. Even as a little girl that was what I wanted to be. I even decided to become a teacher so I would have the same schedule as my kids;” some that are more vague, “I just thought I would have kids someday;” to some that were more ambivalent, “I didn’t think I wanted kids and then one day it hit me. I hope it’s not too late.” These stories often begin in childhood, as we ourselves are parented. The stories evolve over time and the subtle changes that are made to the narrative become subtly yet implicitly assimilated. It is when the story abruptly goes off course, when a woman can’t have children how and when she wants to, that the traumatic loss occurs.
As I have listened to my patients’ reproductive stories, I have taken note of their core assumptions about pregnancy. The more I, as a therapist, can understand what it means to them—how it enables them to fit into their cultural milieu, how it can make them feel they are on equal standing as an adult—the more I have been able to appreciate and begin to understand the depth of their losses. “Acknowledging their own internal narrative, I have witnessed how patients can begin to heal by attempting to “rewrite” their reproductive story”; they may not know exactly how the story will end at this point, but navigating and choosing how they move forward—especially given all the options that current reproductive medicine offers—gives them back a sense of control.
Allison and Core Belief Disruptions
Allison, 38-years-old, had experienced a recently failed IVF cycle. With only one other frozen embryo, she was planning to try another transfer, but was not sure what would happen if that one was unsuccessful as well. Financially maxed out, she and her husband were faced with some very challenging decisions. Should they try another retrieval using her eggs? Should they consider using an egg donor or embryo donation? Should they adopt?
Today, though, she came into session in tears and in a rage. As she grabbed for the tissues and started piling them up on the coffee table between us, I realized that before I even knew what was causing her such pain, “I was feeling helpless and overwhelmed by her emotional state”. I recognized that this was most likely how she was feeling as well. We sat silently for a few moments while she dried her eyes, and then she blurted out that one of her best friends just announced that she was pregnant—and did so via Facebook for the world to see. “She didn’t even have the decency to let me know privately. She knows what I have been going through. It would have been hard enough to find out she was pregnant, but to find out like this? And all the time I opened to her about my struggles, I thought she cared! I feel so betrayed. I don’t even know how long she has been trying for.”
As I comforted Allison by affirming her feelings about her friend, I began a mental list of all the assumptions she had held, and how many had been shattered by her fertility struggles. First and foremost, and a core belief nearly all people have before they start to try to conceive is, “everyone can get pregnant; it’s easy.” Many people assume that all they have to do is stop using birth control and voila! Indeed, it is so drummed into young men and women to “be careful” that it seems as if getting pregnant happens effortlessly. So often women with no fertility issues, and no sense of how their joking comes across, declare “all he has to do is look at me and I get pregnant!” Clearly this is not funny to people in the midst of a fertility work-up or a miscarriage.
Allison assumed that her friend had gotten pregnant on the first try. Whether this was true or not did not matter; to Allison it was simply unfair. One of her core beliefs, that “life is fair,” and that “the world is a just, secure, and reasonable place,” was disrupted by her friend’s pregnancy. Additionally, the belief that “my friends understand me and are supportive of me; I can trust them” was crushed. The challenge for Allison was to make sense out of this threat to her fundamental beliefs. Not only had she not been able to easily become pregnant, but a trusted friend had, and in the process, betrayed their alliance. Could it be mended? Could the earth right itself again and the pieces fall back into place? As a therapist who has observed the great strength and growth that reproductive patients exhibit over time, I knew it could. But right now, as the tissues continued to pile up in our session, things were not logical, the world was not fair, and I needed to listen to more of Allison’s shaken world. While I wanted to be present to the current dissolution of her reproductive story, I also wanted to encourage her to think about her strengths and resources.
Allison went on to talk about her last IVF cycle. “I don’t understand why it didn’t work. We chose the healthiest looking embryo—I didn’t care if it was a boy or a girl. In fact, I told them to just pick the best one and not tell us the gender. We had all the embryos tested. These were the two that came back normal, so it should have worked. Now we’re down to one.”
Allison and her husband had opted for an additional procedure after the embryos began developing called pre-implantation genetic screening or PGS. The test entails removing a cell from the embryo prior to transferring it to the uterus and checking to see if the chromosomes are normal. There is some controversy in the literature about this procedure, as it does not guarantee the embryos will develop normally. It certainly can weed out embryos that won’t develop, but there are some conditions in which the embryos can self-correct as they develop in utero, even with an abnormal result. The test is often very useful if the woman is of advanced maternal age (considered to be 38 and older) or if there is a known health risk.
“And I did everything!” Allison continued. “I went to acupuncture; I stopped eating gluten and loaded up on pineapple. And I was so good about resting for 48 hours after the transfer. I basically only got up to pee!”
I validated that Allison did do everything she could that was within her control. She did do everything right. Only, with pregnancy, doing everything right is still not a guarantee. This brings us to another core assumption, what I call the Santa Claus theory, and a significant part of people’s reproductive story: “If I am good, I will be rewarded for it (Santa will bring toys)” or, stated slightly differently, “if I work hard at something, I will succeed.” In our core belief system, the opposite of these assumptions is also true. So, as it goes, if I am not rewarded, I must be bad, or if I didn’t succeed, I must not be working hard enough. When people mention this in their reproductive stories, they often reference other people who they feel didn’t do everything right. I have heard numerous versions of how unfair it is when someone had kids and couldn’t afford them, or drank, or had them too young, or wound up getting divorced. I can recall one patient talking about her older sister who got pregnant as a teenager, had the baby, and then wound up living back at home as a single mom. My patient was adamant that she would never do it that way. She and her husband got married first, waited until they had finished college and had a steady income, waited until they could afford a house. In their minds they were doing it the right way, and “when they were diagnosed with age-related fertility issues (commonly known as old eggs), they were naturally devastated”. The assumption, “what did I do wrong to deserve this,” is one that runs deep.
The facts are that a woman between the ages of 20-25 has about an 85% chance of getting pregnant; by 30 years of age, the rate drops to approximately 60%; by 40, it drops to about 35%, and when a woman is 45, there is only a 5% chance that she will naturally conceive. People are delaying having children for many reasons, such as pursuing higher education, the ensuing student loans and financial debt, needing to move back in with parents because of debt, not finding the “right” person and many more. Many people also assume that reproductive medicine will be available to them, and are astounded by the cost as well as the rates of success. For women under 35 going through IVF, there is about a 40% chance of pregnancy; for those over 40, it drops to about 11.5%. So, although waiting until one feels established and able to take care of a child is smart, it also can come with risks if one waits too long. At 38-years-old, Allison’s ability to produce healthy eggs was definitely in decline.
When All Else Fails, Blame Yourself
Because reproductive trauma disrupts one’s fundamental beliefs about how the world is and how it should be, the search for reasons becomes paramount. This is especially true for individuals or couples who have “unexplained infertility” or a pregnancy loss for unknown reasons. Generally speaking, about 20% of infertility cases are unexplained, while the rest can be equally divided into female factors, male factors, or a combination of problems in both partners. In my clinical experience, the bulk of the feelings of responsibility fall on the woman when a pregnancy fails. This is likely due to the fact that she is the one carrying the baby and feels in charge of its care. Whether it’s an early miscarriage, an ectopic pregnancy, a stillbirth, or an unsuccessful IVF cycle, women not only feel like it’s their fault, but also want answers. Unfortunately, there are times when there are no answers.
“Allison’s failed IVF cycle was unexplained”. The embryo had tested “normal” and according to her embryologist, it had thawed well and was “hatching” when the transfer took place. Her uterine lining was in great shape. All systems were go. In a follow-up meeting with her fertility doctor, she was told that these things just sometimes happen, and that it was not her fault.
“How could it not be my fault? It was my body, after all! I wonder if there are things wrong with me that they just don’t know about. Or…if I’m just not supposed to have children.” She was crying again and pulling out more tissues.
In a desperate search for reasons, Allison was blaming herself. The assumption was that she had done something wrong. My impulse was to reassure her that she did not cause this loss, but I wanted to hear her reasoning. So, I asked why she thought she was not supposed to have children. “I know I never brought this up in here,” she began. “But when I was in college…well…” she hesitated, “…I had an abortion. I don’t know how you feel about that. That’s why I never brought it up. I know it was the right thing at the time. At least it was the right thing for me. He was not the right guy, or the right time. I mean, I was in my first year of college. I was just, well, experimenting. Can you imagine? It would have if completely changed my life. But now when I think about it I wonder if that was my only chance, that somehow I am being punished. That because of what happened then, I shouldn’t have children now, when I am really ready to be a mom.”
At this moment, Allison revealed another of her core assumptions: you get what you deserve. It is not uncommon for fertility patients to blame their current reproductive issues on what they perceive as past indiscretions. Whether it’s about partying too much in high school, or promiscuity, or as in this case, a previous abortion, their self-blame is not always rational, and almost never accurate. Searching for reasons, it felt more reassuring for Allison to blame herself for her current loss, than to believe it to be some random event. As paradoxical as it may seem, self-recrimination may actually bring some relief to the internal chaos of a shattered schema.
So many times, when couples are struggling with conception, they are given well-intentioned, but inaccurate advice to “just relax” or “my sister-in-law went on vacation and came back pregnant; maybe that’s what you need to do.” For fertility patients, this popular notion translates into: “you’re not doing it right.” Whether it’s about not being relaxed enough (and who is when they’re giving themselves shots!) or for having negative thoughts (i.e., “I don’t think this is going to work”), women may absorb this into their self-narrative. If only one could control conception through one’s thoughts! There would then be no need for birth control! And throughout history, women have conceived under extremely harsh conditions: during war, famine, following rape. These are clearly not times when women are relaxed. It can be helpful for the clinician to remind patients that conception is not a skill, but a biological process that has nothing to do with thinking.
“Self-blame that accompanies reproductive losses can be destructive and promote a downward spiral of negativity”. Depending on the strength of the blame and feelings of punishment, these adverse attributes can become incorporated into the very core of one’s being, leading to negative self-worth, an all-encompassing feeling of meaningless, and depression. Although important for patients to give voice to their deepest feelings of guilt and shame—doing so can actually provide relief—it is equally important that they are able to regain control and process their self-deprecation in a constructive way.
Grief-work, Coping, and the Reproductive Story
With gentleness, I addressed Allison: “You’ve really got a lot going on right now. Not only are you grieving the loss of this pregnancy, you are trying to make sense of your friend, and you are thinking back to decisions you made in college and wondering if you deserve what’s happening now. No wonder you’re feeling awful.” The message here was clearly supportive, but it was also meant to remind Allison that a failed IVF cycle is something to be grieved, compounded by the questions she has about trusting her friend and her own past decisions. Sadly, losses involving failed cycles and even early miscarriages are commonly treated as non-events by society at large, and sometimes even by medical staff. Because of how medically frequent these losses occur, they can become easy to dismiss—but clearly not for the particular woman it’s affecting.
Feeling disenfranchised in her grief, Allison needed to be able to label it as such and to understand that grief of a reproductive loss is not simple. “If you had a favorite uncle who passed away,” I continued, “you would have a store of memories, lots of photos, and people around you would understand how sad you are. But lots of people don’t really get how significant a failed IVF is. You have put so much effort into this—physically, financially, emotionally—it’s got to feel awful that you don’t have anything to show for it. And you’re not only sad, you’re angry. It’s not fair that this is happening when other people like your friend can get pregnant so easily. It’s also not fair that you got pregnant at a time that wasn’t right for you and that now, when it is the right time, you are struggling.”
I could feel the room sigh a breath of relief. Allison’s shoulders dropped and she nodded. She felt heard and understood. But the next step was to have her consider how to cope with these changes in her narrative. She needed to be able to compartmentalize her grief and have it coexist and intermingle with her strengths and resources.
Here’s where the concept of the reproductive story can help. Our patients come to us in crisis. They are in the middle of their reproductive story and don’t know how it is going to end. They can look to the past, understand how the story began, recognize their assumptions, and see how their hopes and dreams got thrown off course. They are certainly aware of the enormous pain they are in at present. And the ambiguity of the future—will they become parents, how will they get there, what happens if they can’t become parents—is causing significant stress and emotional pain. What they can’t see is how the experience of reproductive trauma can actually enhance their lives in the future, and produce a new and revised life story.
The Importance of Telling the Story
One thing we know that helps people grow beyond their traumatic experience is grief work. This entails feeling the range of emotions that naturally occur and being able to tell their story—to select people. Sharing their story is the essence of narrative therapy. The process reduces isolation, increases the sense of connection with others and creates a feeling of being understood. Additionally, telling the story without feeling judged allows patients to unburden that which they feel most ashamed about. Whether this happens in therapy (as with Allison) or outside of therapy is less important than the issues of trust and safety. Allison’s loss of trust in her friend compounded her already fragile self-esteem.
It has been suggested in research on trauma that there are two systems of storytelling?. One is for public consumption; the other is the story that we tell ourselves. That story, the one deep inside of us, is the one that produces haunting, intrusive rumination, and with it self-loathing and self-doubt. In therapy, we try to access that deep story. In order to heal, that story needs to be befriended and looked at in a different light. Allison’s previous loss through abortion filled her with immense shame. Had she not been struggling with infertility, however, that part of her history might never have resurfaced. But the failed IVF coupled with the repeated attempts to get pregnant the old-fashioned way overwhelmed her. The fact that she could open up about it in therapy and have it be received without judgment was an enormous step for her. Instead of continuing to be self-punitive, Allison was on the road to replace her harsh and self-punishing inner narrative with a more tender, kinder version. This is a process that takes time, as all grief does, as the gradual acceptance of a new story emerges.
I had three goals for Allison at this point. Although laid out here in numerical order, these therapeutic goals are not linear; rather they co-exist as part of the ongoing process that occurs as one assimilates the trauma into a new narrative:
1. Manage her emotions and reduce her negative self-talk. I encouraged her to express her feelings without the harsh self-critic that was so deep-rooted. Labeling what she was experiencing as grief helped to validate that her loss was real. I also encouraged her to reach out to others for support—carefully. I suggested some local peer-led support groups to contact so that she could find other people who would really have empathy for her story of trauma and loss.
2. Work on ways to craft new narratives, new schemas. Allison found it helpful to think of her reproductive story as evolving. She thought about her remaining embryo; what if it didn’t work? While some people take comfort in focusing on the present and not delving into the “what-ifs,” Allison needed to have a plan ready in the wings if her next attempt didn’t succeed. Although she had yet to make a firm decision about anything, giving space to contemplate the future was allowing her to think about a new narrative.
3. Recognize that her core assumptions about pregnancy, her relationships, and feelings about herself were changing. Trauma can be thought of as a turning point. There was the time before, and the time after. Beliefs about oneself and how the world works can significantly change. And, as will be discussed, post-traumatic growth following reproductive losses can be quite life-altering in a positive way.
Out of Loss There is Gain
There have been numerous studies focused on posttraumatic growth (PTG) and the positive gains that can arise from challenging life crises?. Whether it’s recovering from a life-threatening disease, surviving a car crash, or witnessing a mass shooting, people can grow, change, and appreciate life in profoundly different ways.
As we have observed with Allison, trauma challenges fundamental assumptions—about oneself, one’s relationships, and the fairness of the world. The disruption to one’s narrative or schema commonly results in negative responses such as intense anxiety, depression, anger, intrusive thoughts, and/or feelings of numbness. Physical reactions are also common: headaches, gastro-intestinal upsets, fatigue, or a general sense of not feeling well. While the consequences of trauma result in psychological and physical distress, personal growth can occur in its aftermath as well. There is a cognitive restructuring that occurs in order to rebuild a sense of the future, and focus on what it takes to cope and find meaning. It’s important to note that the ability to grow does not signal an end to the trauma, the pain, or the distress, but they live alongside each other to create a new worldview.
A greater appreciation for life in general is a common characteristic of growth after trauma. There is often a newfound sense of gratitude for the everyday, a not-taking-things-for-granted attitude. For people dealing with reproductive trauma, research has shown that when they do become parents—however they get there—they tend to have a better relationship with their children, with greater emotional involvement?. The speculation is that the parent-child relationship may be strengthened because of the great lengths it took to become a parent, and the appreciation for their family becomes heightened.
From clinical experience, I have seen infertility and pregnancy loss patients grow in extraordinary ways, whether they are able to eventually have children or not. So many who have been down this road want to “give back” as a result of their experience. One couple made memory boxes for other parents and delivered them to the hospital where their daughter was born still. Another woman took to Facebook to educate the community as to what to say, and what not to say, when someone is struggling with fertility issues. Others have taken the opportunity to reevaluate their careers; I have worked with many women in healthcare, including mental health professionals, who decide to change focus and specialize in working with reproductive patients. One nurse opted to return to work in obstetrics so she could be there at the front lines and provide care to those in need.
“As people balance feelings of loss with a sense of growth, the strength that emerges is distinct”. Knowing that bad things happen, that we are all vulnerable, and that—most importantly—we can get through it, increases one’s resiliency. A new core belief can develop: “I am a person who is tough, hardy, and can handle just about anything!”
The Reproductive Story Ends
Our reproductive stories have a beginning, middle and end. As discussed earlier, patients enter therapy in the middle of their story at a heightened state of loss and pain. Using the story as a therapeutic tool addresses the inner beliefs and core assumptions of pregnancy and how it was supposed to be. Whatever the trauma or loss that has brought them in to our office, this experience is clearly not how their reproductive story was supposed to unfold.
One of the pluses of using the reproductive story in treating patients is that they immediately get it. Although there is a great deal of psychological theory behind it, it’s instantly recognized and understood without any psychological jargon. Knowing that they are in the middle of their reproductive story, gives them a sense of a timeline. Where they had felt a loss of control, they can utilize the idea of their story to edit, rewrite, and come up with new possibilities. They can try on different endings: if I use an egg donor, how will I feel? Can I emotionally and physically handle another miscarriage? If we decide to stop trying, how will our lives have meaning?
The reproductive story allows patients to understand the personal meaning of pregnancy and family, and the depth of what is lost when the story and their core beliefs go awry. I have the opportunity to explore these narratives, and the trauma they have experienced opens doors to explore new possibilities in creating a family, and in the broader context of their lives. Although their reproductive trauma has changed them forever, they also can embrace the ways in which they have grown through the process.
Postscript
As for my work with Allison, over the course of the next several months she continued to progress in a constructive way, between grief and growth. She was preparing herself for her next IVF transfer with the one remaining embryo. In looking at options beyond that, both she and her husband agreed to “wait and see” and keep the option of using an egg donor on the table.
The day she walked into my office beaming I knew she was pregnant. Her blood test results came back with a really high beta and had doubled, meaning that the embryo was developing as it should. We celebrated, cautiously, as we knew that there are never guarantees with pregnancy. She was trying to enjoy the here and now, even though it was filled with anxiety about all the things that could possibly go wrong. I normalized this for her; everyone who has had a reproductive trauma is anxious about a subsequent pregnancy, another loss. Gone are the days of that innocent assumption that getting pregnant and having a healthy child is natural and easy. As I welcomed her into the next chapter of her reproductive story—pregnancy—I reminded her that whatever happened, we would get through it together.
References
(1) American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association: Arlington, VA, USA, 2013.
(2) Jaffe, J. & Diamond, M.O. (2011). Reproductive trauma: Psychotherapy with infertility and pregnancy loss clients. Washington, DC: American Psychological Association.
(3) Cann, A., Calhoun, L.G., Tedeschi, R.G., Kilmer, R.P., Gil-Rivas, V., Vishnevski, T., & Danhauer, S.C. (2010) The Core Beliefs Inventory: a brief measure of disruption in the assumptive world. Anxiety, Stress & Coping, 23:1, 19-34, DOI: 10.1080/10615800802573013.
(4) Van der Kolk, B. (2018). Trauma conference: The body keeps score. www.pesi.com.
(5) Tedeschi, RG & Calhoun, LG (2004) TARGET ARTICLE: “Posttraumatic Growth: Conceptual Foundations and Empirical Evidence”, Psychological Inquiry, 15:1, 1-18, DOI:10.1207/s15327965pli1501_01
(6) Golombok, S., Lycett, E., MacCallum, F., Jadva, V., Murray, C., et al. (2004). Parenting infants conceived by gamete donation. Journal of Family Psychology, 18, 443-452. DOI: 10.1037/0893-3200.18.3.443.


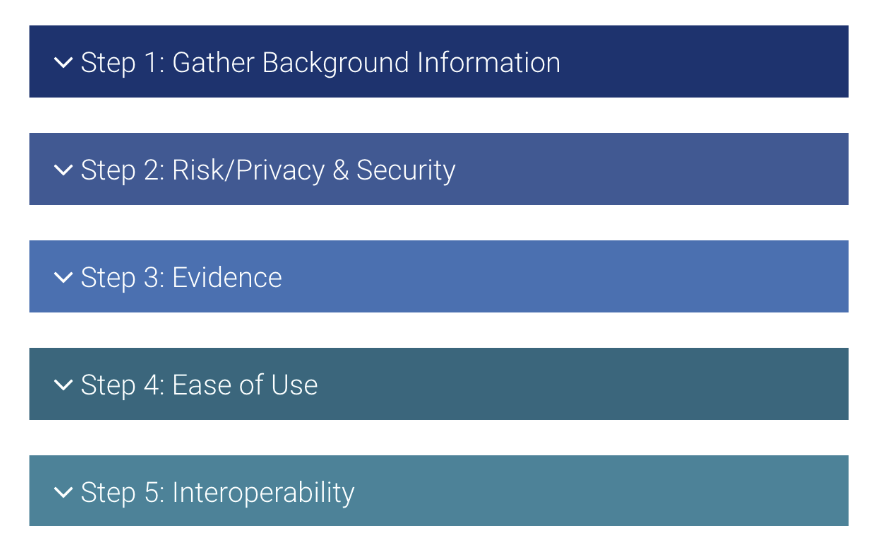 On the other hand, technology can be an important tool in our work. For my children and adolescent patients, using apps to track mood and sleep have yielded more cooperation than tracking those metrics on paper. Apps that track mood and anxiety symptoms can help individuals share their symptoms with their doctor or therapist. As professionals, we can guide our patients in choosing apps that best meet their needs. Apps are not regulated and there is little oversight into their creation or claims. We can help our patients become better equipped to choose apps that are helpful rather than harmful. The American Psychiatric Association has created guidelines to assist professionals in helping individuals choose the best mental health related apps. The APA has developed the App Evaluation Model that can help providers evaluate the appropriateness of an app with their patients. (see figure)
On the other hand, technology can be an important tool in our work. For my children and adolescent patients, using apps to track mood and sleep have yielded more cooperation than tracking those metrics on paper. Apps that track mood and anxiety symptoms can help individuals share their symptoms with their doctor or therapist. As professionals, we can guide our patients in choosing apps that best meet their needs. Apps are not regulated and there is little oversight into their creation or claims. We can help our patients become better equipped to choose apps that are helpful rather than harmful. The American Psychiatric Association has created guidelines to assist professionals in helping individuals choose the best mental health related apps. The APA has developed the App Evaluation Model that can help providers evaluate the appropriateness of an app with their patients. (see figure) 






