The Face of Family Estrangement
Detachment Brokers
A Roadmap for Change


Lawrence Rubin (LR): You may be known to our readers as the founder of Gay Sons and Mothers. But they may not be familiar with how extensively you’ve been trained and how long you've been practicing as a psychotherapist with a personal interest in working with gay men and their mothers.
Rick Miller (RM): I'm a gay man who grew up really appreciating the bond and love of my mother. And, in hindsight, as an adult, what it meant for me was that I got to be myself. She didn't necessarily know that I was gay, or maybe she did, but she never forced me to do anything differently than what I did.
And growing up in a world in the 1960s where it was prescribed, this is what boys do, having a mom who let me be me — and we did a lot of things together — was pretty miraculous. I hear so many stories about people growing up whose parents abused them or forced them to do things differently.
I wrote a book several years ago for clinicians about doing hypnosis with gay men. I thought it would be relevant to do the research or to seek out research about gay men and their mothers. I looked at the literature about gay men and their mothers to include in the book. You'd think this a cliché topic and that there would be way too much information to use. I couldn't find anything! I thought, I’ll write an article about this, and it ended up turning into video interviews. And from there, I started a nonprofit called Gay Sons and Mothers.
We are educating the public about the special bond between mothers and their gay sons and how she contributes to his sense of well-being in the world. It's a multicultural story that looks at strength, at disappointment, and is a very emotional topic.
LR: So, even before you and your mother had a conversation about being gay and you knew, you had no particular concern over sharing it with your mom. You didn’t worry how she would take it, how you'd be perceived, how you'd be treated. You were just free from the start to be you.
RM: Well, I was free to be me, but I didn't come out to them — meaning my parents, my mother and my father — until I was 21. So, it was interesting that I had the freedom to be me, but I didn't feel 100 percent free to be me because I waited longer to come out than I probably needed to in hindsight. Today, many kids are coming out at a much younger age to their parents. Of course, the world is very different.
LR: If you intuitively felt accepted by your mom and weren’t censored or limited in any way from being you — you haven't talked about your dad — why do you think it took you as long as it did to become public about it?
RM: Well, so, it was the early 80s. So, AIDS was hitting the press big time, and I suppose on one level, I was protecting her or them from thinking that something would happen to me, which, knock on wood, did not happen. I was afraid that I'd be rejected, and, not to sound callous, they were paying for my graduate school education, and I just made a mental note in my mind I was going to wait until I finished school to come out, which is so stupid.
Knowing my parents, of course, they wouldn't have done anything differently. It took them a while to come around, a month or so, which I thought was horrible at the time. But I look back and I think that my parents had to go through their own grieving when I came out to them. Of course, they knew I was gay long before I came out, but hearing it was definitive. And it took them a short time to acclimate and appreciate it. I was incensed at the time. And, often, I say to children and to parents, it's okay to grieve.
LR: Incensed about?
RM: They were not 100 percent supportive the second I came out to them. And the first thing my father did when I came out was to become a little weepy saying, “the world is unfair, and I'm worried about what that will mean for you.” I took it as supportive, for sure. And then he kind of changed the tune for a bit, and that is when things turned ugly, and again that lasted a few weeks and then everything turned around.
LR: Smooth sailing with your parents and especially your mom ever since.
RM: Yep. And I had a partner that I was moving in with at the time. So, what I did, which I shouldn't have done, was when I came out to them, I told them that I was moving in with the person they knew as my friend all at once, so that threw them a little bit.
LR: Overload! Going back to the second part of the earlier question about your foundation; how do you think clinicians can benefit from awareness of it?
RM: There's so much inherent in the videos that we share through Gay Sons and Mothers. It's not only about the relationship between a mother and a son, but that part in and of itself is so affirming. Clinicians can watch stories of sons and their mothers and appreciate what it is being gay. And it's not only mother in these interviews. Families are talked about. Extended families are talked about. Culture and religion are addressed in these videos.
So, there's a lot there, and, when mothers are struggling with their kids, I send them videos from Gay Sons and Mothers. On our website, there's a link to our Instagram page. We have a YouTube page. Sons watch. Most people — therapists included — watch these videos and have a deep emotional resonance around the issue of being included, being loved, being supported, being rejected. It's hard not to feel something when you're watching videos pertaining to these themes.
LR: A connection. How would you respond to a therapist or to a non-therapist who’s visited your site and says, “Yeah, well, what about gay sons and their fathers?”
RM: There's way more information in the literature about gay sons and their fathers than there is about gay sons and their mothers. And if there hadn't been any with fathers, I would have pursued that, as well. I grew up with a great relationship with my mother. I had the fame of saying to my siblings, “Mommy likes me best.” It carried me through. So, it seems completely perfect that that would be the focus of my work.
Historically, mothers in the 1970s — or even earlier in the psychiatric and the medical field — mothers were blamed for making their sons gay. And, so, with the lack of literature out there, what's missing is that mothers have the power to raise sons who are mentally healthy, just from being a good enough mother. And, so, that premise is so important to me that I've focused exclusively on mothers and sons.
The issue of fathers and extended family is embedded in the work anyway. So, this project, Gay Sons and Mothers, is inclusive of the entire family. And we're also expanding beyond just gay sons and mothers. We're talking about trans children and all sorts of things.
LR: How has your advocacy and clinical work been informed by your own personal evolution?
RM: Oh, gosh, that's such a big question, but I think I can get there. I came out in 1983 — I was already a clinical social worker. In the 1980s, AIDS was emerging, and gay men were dying in big cities, and people were afraid. Homophobia was on the rise because people were afraid of catching AIDS. I was working in the AIDS field, doing volunteer work at this time, and I started working with the gay community from the start.
Boston, where I lived, was a progressive place. So, I was known in Boston as being an out gay male therapist. I mean, there was no web at that time, but anyone who knew me would know that I was gay. But I was also practicing in a very conservative place, Boston, Massachusetts, very hierarchical, very psychodynamic. So, in the professional world that wasn't the world of AIDS, I worked in a hospital. I kept a very low profile, and I felt like I didn't fit in the hierarchy of psychiatrists, psychologists, social workers.
I'm a social worker, and looking back at my evolution and my history, I wish I had put myself out there more because the contributions that I'm now making to the field in the last ten years as a writer, as a teacher, as someone who's done Gay Sons and Mothers, if I had the confidence to do some of this earlier, I would have done more research focusing on gay men, on gay men and their mothers, gay families. And I think I could have made a bigger contribution to the field.
What happened for me is I started my private practice in the mid 80s, and I switched to full-time private practice. So, I left the hospital. I left the agency where I was doing AIDS work, and basically, I hid in my office with the door closed for decades. And I was very successful in private practice, in part because of my clinical skills, in part because of my personality, and I got to hide.
Once I wrote my first book and I started teaching about working with gay men, I could no longer hide. And, at the time, I was probably 52 years old — 10 years ago. And I'm really glad it happened, but it forced me beyond a comfort level that was really important and good for me, and I wish I did that sooner.
LR: So, you came out of the closet before you came out of the office. I can see that your personal story could be used as an exemplar, not only for gay therapists, but for gay men, whether still not out or out. I would imagine that you don't impose your story on others. But by living it and being genuine, as you've always struck me, you are an unintended role model.
RM: Well, thank you for saying that, and it served me very well in my practice. I grew up in an upper-middle-class family with well-being and mental health and good physical health. And, to me, that's how everyone lived in the world, and that is so not the case. And so, as a gay man who had a sense of self, who worked with gay men, I served as a role model to other gay men, to all my clients really but specifically to other gay men who didn't have the good fortune that I did or didn't have the personality that I did.
So, my being outgoing was a very good clinical skill, and, fortunately, in my early 20s, I was in therapy with a therapist who was gay, who had a very good sense of himself, who had a great sense of humor, and who allowed me in the process of therapy to love myself. If I had chosen one of those uptight, analytical therapists in Boston instead, I don't know where I would be right now.
When I was looking for a therapist, I was given the name of eight different people. Back in 1983, I was calling their answering machines. On some, I was hanging up because I was frightened by them. Others shamed me through their tone, and thank God, I didn't work with them.
LR: What are some of the clinical challenges you've found in working with gay sons and their mothers?
RM: Long before I ever knew I'd be working with gay men and their mothers, I had a gay male client who was really struggling with confidence. He grew up in the projects outside of Boston, and his father left the family, and deprivation was a big part of his upbringing. So, one day, for whatever reason, I had his mother join him in a session and it was like the heavens opened up.
I understood him so much more, and the bond and the strength of their relationship was amazing. It helped so much in the clinical work. He was a catalyst that led to this project, Gay Sons and Mothers. Every now and then, I'd have another mother and son together, but it wasn't why they were in therapy. Once I started working on this project, various people consulted with me, families for help with their families. For some, in the field of psychotherapy, for others, through the nonprofit where, for free, I just consult with people and help them along.
What's been interesting is one mother and son that I'm working with right now in therapy are enmeshed with each other, and they're seeing me every two weeks. On certain days, it feels like couples therapy and I really have to work with them to detangle and let go of their expectations with each other. And, so, this is a divorced mom with an only child who's gay, and they expect each other to meet needs that goes well beyond what they should be for a mother and a son.
This isn't the case in all circumstances, but I think it's a great example of how it can be a bit of a burden on both ends to have this close bond that goes kind of way too far on both ends.
LR: So, enmeshment is one of the challenges. I imagine acceptance is another.
RM: So many gay men are way too careful, and they're not coming out to their families as soon as they might, or they give absolutely no details about their private lives to their families who really want more from them. So, that is another challenge, that in being careful, even once they come out, being careful continues to be their MO, even when they don't need to be, and people want more from them. They want to hear more details about their day-to-day lives or what they struggle with, or are they in a relationship with someone?
LR: And I wonder if these particular men are so cautious and close to the chest with their families, if they're even more so outside of the home.
RM: Correct. I'm working with a bunch of men in their 50s, let's say in their 60s, who came out in an era where it wasn't okay to be gay. And even though it's fine now and they have jobs where they are out, they, without even realizing it, are kind of slipping into modes of privacy and protecting themselves because it's a habit that's been with them through their life.
LR: I was going to ask you a little bit later about working with elderly gay men. But this seems like a good point to interject the question of, “what are some of the clinical challenges in working with elderly gay men whose mothers, I imagine, have long passed?”
RM: The most significant challenge is that they grew up in an era where they couldn't be out, where it wasn't safe, and many older men were kind of forced indirectly or even directly to live conventional lives and got married and had children without even questioning the freedom of living life as a gay man.
I had a great-uncle who was gay, and he never came out to my family. When I came out to my parents, they said, “Well, Paul has lived a good life. So, we know that you'll live a good life, too.” But this great-uncle, my grandmother's brother, was in his 80s when I came out. And he said to me, “I really appreciate that you have freedom that I didn't have, and I hope that you will keep my secret from your family because I just don't feel comfortable being out there.”
LR: Well, I wonder if that fear of abandonment, being cast out by remaining family is that much greater to an elderly man?
RM: He had an incredible social network. He lived in Washington and was cryptographer for the CIA because keeping secrets was something that they did well. So, he had the love of a community of people, and my mother, his niece, and us, meaning my mother's children who were generations below him. And he was still worried about our knowing. It was just a pattern that was ingrained for the time with which he was raised. It's that simple.
LR: Can you imagine taking homosexuality, or any significant part of your identity, to the grave?
RM: When he died, my mother and I went to Washington to clean out his house — he saved everything. There was a pile of letters that his gay friends wrote to him in the 1950s and the 1960s about falling in love with men that they met in cruising areas in parks, and how they couldn't tell their spouses and how tortured they were.
We were cleaning out his house with three of his close friends. My mother came to me, without saying anything, handed me the pile of letters, and I read them. And I thought poor Uncle Paul would die if I kept these letters, so I shredded them and threw them out. And it is my biggest regret because in these letters was the reality of gay history lived by all these men.
But, in my desire to be loyal to my great-uncle, I threw them out. And this was maybe three or four years after I had come out. I was still living in a careful way and more worried about loyalties. If I had these letters now, what they would mean? Oh my God.
LR: What clinical challenges have you experienced working with gay sons of mothers from other cultures, the Caribbean culture, the Asian, the Southeast Asian, or even African, where homosexuality is shunned and punished, sometimes even fatally?
RM: In these cultures, homophobia is rampant and masculinity and norms around masculinity are such that fathers are not accepting of their gay kids. Religious norms are such that being gay is a sin and these are beliefs that communities buy into without questioning. So, fathers are often emotionally and physically abusive to their sons. Mothers are forced to choose between their husband or their child.
Some mothers choose their husband over their child. I had a guy that I interviewed who was Latino, and his mother said to him, “First comes God, then comes your father, and then comes you.” So, when he came out, they sent him to an aunt's house far away to Texas where he would somehow have a different life for himself. He ended up responding to a personal ad from someone who he didn't know at the time was a human sex trafficker, and he became a victim of human sex trafficking. It's a tragic story, and he's now an advocate for all of this. But his parents kicked him to the curb and still don't accept him.
LR: Have you worked with men and mothers and their parents from other cultures, where the parents themselves were afraid of being sanctioned, punished, or harmed?
RM: You're saying that with a great degree of sensitivity and attunement. Most situations, that is exactly what the parents are feeling, but they don't recognize that in themselves. What they recognize is what they're supposed to believe, and that's what they've gone along with. I've worked with Mormon families who have rejected their children. I've interviewed a Latino Mormon man whose mother read his journal and packed up his bedroom one night and put all his belongings in the garage and said, “You're not going to live here anymore. What you're doing is a sin.”
Eventually, they came around and made up years later. These horror stories unfortunately exist. Some families that are less severe than the examples I gave don't let their kids come to family holidays. They insist that they not come out to extended family that there’s all these conditions. There's a woman named Caitlin Ryan who’s done a lot of research through her organization called the Family Acceptance Project. Her work shows that LGBTQ family members can gain acceptance with their children or their siblings through being exposed to other people that give a message that it's okay.
And that's essentially what we're doing through Gay Sons and Mothers. We're sharing stories saying, “Look, we're out in the world and everything is fine.” And as family members realize that it's okay, they are far more accepting of their gay children. So, that's the message that we need to get out into the Latino, the Asian, the Black communities, and the best way that they're going to accept it is by hearing stories through people like themselves.
If they're hearing from a gay social worker who's White that it's okay, maybe some percentage of people will listen to me and be comforted, but they're going to hear it most from another father who's found through his own experiences that it's better to have a relationship with their child than to reject them.
And that's essentially what we're doing through Gay Sons and Mothers. We're sharing stories saying, “Look, we're out in the world and everything is fine.” And as family members realize that it's okay, they are far more accepting of their gay children. So, that's the message that we need to get out into the Latino, the Asian, the Black communities, and the best way that they're going to accept it is by hearing stories through people like themselves.
If they're hearing from a gay social worker who's White that it's okay, maybe some percentage of people will listen to me and be comforted, but they're going to hear it most from another father who's found through his own experiences that it's better to have a relationship with their child than to reject them.
LR: I imagine there’s a significant number of these families that don’t make it successfully through therapy with you. This young man is left feeling just as isolated and rejected as before.
RM: Right. Or the young man will stay in therapy and build his own community, but, unfortunately, not with his family, outside of the family and elsewhere. That said, I am a family therapist. I’m a couples therapist. I'm totally optimistic. I never give up on families reuniting. And, last year, I worked with a fundamentalist gay man in his 30s, really successful in his career and in his life. But he didn't come out until his 30s to please his parents. I had three joint sessions with him and his mother, with the hopes of bringing them together. He never thought it would happen.
I met with her alone first, and she was talking about the Bible and blah, blah, blah, blah. They didn't stick with the sessions, and eventually started talking to each other. A couple of months ago, she was potentially diagnosed with cancer, and that's what brought them together more than anything else. And I wish it could have been sooner.
LR: How would you advise straight therapists working with gay men, beyond the standard of “unconditional acceptance?”
RM: You raise a very important issue about unconditional acceptance, and many well-intentioned straight therapists try way too hard with their gay clients. In my life, socially, I'll go to a party, and they'll say, “Oh, do you live where all the gay people live? And do you know so and so, and so and so, and so, and so?”
LR: Gay Jewish geography.
RM: Exactly, and often I do. But therapists who try to promote unconditional acceptance and convince their clients that they're gay-affirming and then offer, “Oh, I have a neighbor who's gay,” which actually may induce a lack of trust. The best way to promote unconditional acceptance is to simply say, “I’m straight. Are you comfortable working with me? I am accepting, and I've worked with other gay clients. But, please, if you feel any bit of discomfort, let me know. Let's talk about it.” To me, that's unconditional acceptance, and that's more welcoming than doing a sales pitch that ends up sounding like a microaggression more than anything else.
So, my mentor, Jeff Zeig, accepted me for who I was, and he’s a straight man. There was something so profound in that experience for me. Was he the first straight man that accepted me? No, but it was wonderful to have a mentor who didn't care if I was gay, didn't pathologize me, and said, “Write a book about working with gay men, the field is lacking this information.” It was so validating. And so, what he did for me, which all therapists ideally do for their clients, is embrace, love, support, and send me out into the world to be successful.
That is unconditional love, and that is what straight therapists can do for their gay clients. And what I say in the work that I do is you're giving your clients a bigger gift of healing than you would even recognize because your clients are coming into your office with their presenting problem, whatever that happens to be. It may have nothing to do with being gay. And, through the love and the acceptance and the respect that you're showing to them, they're getting additional healing from the experience of being in your office.
So, frequently, when people want a referral to a therapist who's a gay client, frequently I'll say, “Why don't you work with a non-gay therapist? Because there is extra work that you can have done, as a result.” Some people will do that, some people won't.
LR: I used to think it important to be colorblind, but we must see color to validate the experience of the “other.” that idea. Similarly, one can’t be gay blind, because being blind to that does not suggest acceptance. It suggests walling off and not affirming that person, not accepting that person. So, I imagine that a clinician working with a gay person has to be very cognizant of the stories, the history that this person brings into therapy.
RM: Yes. The words that are coming to my mind are cultural competence. And that's what we need in the field these days. And I, too, did the same that you just described. I worked with an Asian gay man and a Black gay man, and I cringe when I think to myself or I even probably said things aloud that it's not as bad as you perceive it to be, which is absolutely not true.
LR: It’s not affirming.
RM: Right. The best thing that we can do is to hear the experiences that our clients are bringing to our offices and trust that to be true. The other best thing that we can do to become culturally competent is to go to workshops or watch videos like this or read a few books or speak to your gay friends and family members about their experiences to get educated. It's not hard to do. I find that in our field of mental health there are many people who are well-educated and liberal in their thinking, so that they feel like they have all that they need to know.
But their gay clients are testing them indirectly and don't feel safe because they're presenting a norm that may be uncomfortable. The other thing that I found, and I've mentioned this to you before, is that the field in general, of course, is run by metrics and numbers. And the most successful clinicians and teachers in the field have large numbers of followers and huge turnouts to their conferences. When I teach, sometimes I get 20-25, maybe 40 attendees, if I'm lucky, at a big mental health conference. Well, that's not good for the conference.
So, I'm not advancing as I'm teaching about working with LGBTQ people. And there are very few courses offered at huge conferences, which is unfortunate. So, my advice to people who are organizing conferences is to put us in panels with other people, and that way we can kind of gain exposure and educate people.
LR: So, the idea of a gay-affirming therapist is more cliché than anything else I would think because if you're not a person-affirming therapist, you're not going to be a gay-affirming therapist. Am I getting it, right?
RM: Yeah, yeah. And I mean, interesting. A clinician that's worked a lot with the gay man or the LGBTQ population by nature is gay-affirming. I know through conversations with a person who has worked a lot with the LGBTQ population is gay-affirming, and they've cultivated acceptance and skills that are affirming and comfortable. As a person, are you a gay-affirming person? I'm not asking you that. I know that you are, but I'm asking people who are listening to this. Do you understand what it's like living life as an LGBTQ person in today's world?
And if you're honest with yourself, maybe there are things you don't understand, and there's ways of getting information. If you pretend that you are, you're fooling yourself. People are going to see beyond that.
LR: They’re going to catch up.
RM: So, when you go to therapy, you should be talking about your sexual life. Many gay clients, out of shame, won't even broach the idea of sex with their therapists. Or, when they talk about sex, their therapist winced because they don't believe in open relationships, or they think that gay men are too sexual, and their biases are coming forward. I h
Learn how to see. Realize that everything connects to everything else
— Leonardo Da Vinci
The internet in the late 1990s was exciting because you could research topics including sports, education, and entertainment and stay in contact with old friends. In retrospect, however, when working with adolescents at a local PHP and IOP, I/we ignored the impact of Myspace and other social media websites that encouraged cutting and suicide. We attributed the increase in behavior to peer influence and the impact of dysfunctional family relationships.
Today, social media’s algorithms and influencers have more of an impact on the family than we are willing to acknowledge. It has been argued that social media’s algorithms entice family members who use social media to spend more time on the app than with their own family or friends. As a clinician who works with families in private practice and schools, it has become increasingly clear to me that social media’s algorithms and influencers often occupy the “empty chair” in the family sessions.
It was evident to me while watching the hearings in Washington, DC a year ago that social media companies will not change their algorithms and will not share them for everyone to understand. The Netflix documentary The Social Dilemma had many former social media employees expressing eye-opening concerns. The film revealed how tech companies hire psychologists to make a persuasive algorithm to increase the appeal and use of their apps.
Unfortunately, Congress appears powerless, unwilling, or both, to make changes due to the powerful lobbying groups. Some have said that Congress is waiting for the UK’s Parliament to take the lead in regulating this industry.
Social media makes money by showing images or comments that their algorithms “say” are interesting and encourage consumers to “like,” “comment,” or “share.” Social media companies have also learned the more divisive and inflammatory the post, the more views and money there is to be made.
Well-designed apps continually boost the user’s connection by showing information, comments, or images that they have discovered are of interest. Showing an opposing view or people from a different “virtual tribe” will decrease the views/time spent on the platform and decrease money for the makers of the app. The app creates a virtually closed system that does not allow any “disliked” information or contradictory views.
If different members of a family “like” different apps, or different posts on the same app, each member of the family may conceivably align with a virtual presence against their actual brick-and-mortar kin or friend. As a result, algorithms have the power and potential to intensify the already-present pattern of conflicts within a family system or relational circle. Disconnection, chaos, conflict, and exacerbation of individual and/or family pathology may follow.
Influencers have always been present in our society. For many years, our influencers were teachers, family members, neighbors, friends, supervisors, actors, news anchors, and other people in our community. We would ask our immediate community personal and embarrassing questions. Many times, adolescents and young adults would get personal and difficult questions answered by building up the courage to approach someone face-to-face in their community.
Building up the courage to ask questions taught us how to manage our fear and anxiety. Navigating face-to-face relationships also teaches us how to manage embarrassment, frustration, anger, resentment, and rejection which is an important step in our development. Non-virtual relationships also allow us to feel emotional and physical closeness that is missing in social media/virtual relationships.
Today, our society is teaching the belief that anxiety is a bad thing that needs to be kept at bay. We in the field know that anxiety is not the problem. Arguably, anxiety is a result of the person’s core belief and/or what is going on in a relationship that will not change for the better. Because of this, adolescents and young adults are narrowing their non-virtual relationships because it is the path with the least amount of risk.
When asking intimate or difficult questions face to face, we learn how to manage proximity and closeness in our family and friend groups. We learn who in our family and friend groups has earned the privilege to be asked these intimate questions. We learn who can keep our personal life private and who may have the better answer, which builds friendships and family relationships.
Social media triangulates family and friends to find the immediate answer and connects people to a tribe that challenges them the least. Many believe decreasing their non-virtual relationship decreases their anxiety, but it actually increases their isolation from their community and increases their anxiety when meeting someone face-to-face. Also, virtual relationships give the illusion that all of these important ingredients are present on social media.
Family members are turning to influencers as if they are therapists/experts with answers (good therapy doesn’t give answers.) Or they are turning to politicians that they must blindly follow (good politicians allow debate.) We know the politicians who are at the extreme right or left posting inflammatory statements get the most views.
These influencers are making statements encouraging family members or friends to pick sides, skipping the process of face-to-face discussion with follow-up questions or reflection that occurs in non-virtual relationships. When a person stops exchanging ideas with their family members or friends, it creates a dangerous virtual closed system.
During my training at the Minuchin Center for the Family, I was always asked, “Whose shoulders is the adolescent standing on?” One year, a family I was working with agreed to meet with Dr. Minuchin for a consultation. Dr. Minuchin said to me after the consultation, “You will fail because the system of care erodes the boundaries of the family.” It became evident that each of the six members of the family relied on their own individual therapists to reinforce their view of how everyone else in the family was toxic.
This taught me the importance of understanding the family map in addition to evaluating if different family members were in coalitions with other therapists, social workers, and/or even agencies. It was an important step to understanding the map and identifying where the coalition(s) across generational boundaries occurred with the family and larger system.
In many of the sessions, other families were able to overcome their symptoms once they began to work on their relationships and change their relationships with the systems of care. It was exciting to see when the system of care noticed their triangulation with the family. Other times it was sad to see how systems of care did not see how they were triangulated against family members.
Today, influencers are present in the family session as seen by the virtual coalitions that the member(s) must maintain as if they were their closest friends in order to be a part of their tribe/team.
Families are always ahead of the researchers and therapists, but do we listen to the pieces together as therapists? The following are the themes/symptoms families have discussed in my own family therapy sessions as well as those of colleagues in the wider clinical world. Each of these impacts adolescents, and, in turn, how they impact the adults in their home. On both sides of the relational equation, social media has a powerful impact, and not always for the good of individual and shared relationships.
When one or more family members are engaging in excess screen time from two to sometimes more than six hours a day on social media, the research shows there is an increase in symptoms of depression and/or anxiety. If someone has this much daily screentime, they are displacing healthier activities or hobbies such as walking, sleeping, drawing, painting, mindfulness, and gardening, to name but a few. And this displacement impacts the interactions in the family and community by isolating them.
Algorithms encourage constant social competition and comparison, and as such function as social currency between peers and family members. Adolescents typically feel that they are on stage competing to increase their position in the “hierarchy” with peers and/or parents. They continually compare themselves to peers at school and other families.
The algorithms that draw them in make it difficult for them to turn off the social app and get away from the stresses of adolescence. Jockeying for competition and comparing their lives to others may at times backfire, leaving them feeling poignantly and painfully alone. Again, this constant competition and comparison mirrors similar interactions in the family that can contribute to increased anxiety and depression.
The adolescents I’ve worked with discussed how they feel lonely and alone. They feel lonely when they are not supported or perceive they are not supported by family or friends, and feel alone when they have little face-to-face contact with peers like we all experienced during COVID.
The two-dimensional views people experience when using Zoom as the primary source of connection do not “feed the soul.” There is no substitute for good eye contact and close physical proximity. The irony is social media was created to decrease feeling lonely and alone but actually amplifies it. In family sessions, many, if not all, talk about how they feel lonely and hoped that social media would fill this void but were unsuccessful.
Adolescents typically think they are invisible or always on stage. These polar positions can occur on the same day for any adolescent. They think they are invisible when they are spending more time on their phones not getting enough likes and/or views, whatever that means to them.
This causes them to work harder on their online stories and identities, decreasing the proximity with their non-virtual friends. Many adolescents begin to look for the “genuine” or “real” friends, determining they are only present in social media and not in their own hometown or within the family walls. In the family, these themes are very common when there is already a pattern of disengagement (invisible) or enmeshment (always on stage).
The adolescent also thinks their peers are waiting for them to make a mistake so it can be posted online. This position makes them feel as though they are always walking into the cafeteria for the first time as a freshman in high school. Adolescents are supposed to make mistakes, struggle, learn about relationships with typical external distractions (friends, family, media, work, and politics). But does social media fill the lonely times when the adolescent and young adult are reflective and recoup?
Being invisible or always on stage prevents the adolescent from developing close connections with peers, teachers, coaches, or other family members. This results in adolescents seeking temporary relief from asking a “person” and instead getting information from social media.
Information on the app is monitored by the algorithm and is not as embarrassing or stressful as asking a family member, friend, or teacher. This is where social media begins to enter the family, impacting the adolescent development and challenging their family’s belief system.
The algorithm also motivates the adolescent to seek select information that aligns with their narrow/closed view about politics, friendship, religion, sexual identity, sexuality, gun laws, suicide, mental health, or any other hot topic.
The Atlantic, 60 Minutes, Pew Research, the New York Times, and the Wall Street Journal have done a great job discussing all the different ways social media has triangulated members of our families. The New York Times article on suicide, “Where the Despairing Log On and Learn Ways to Die,” by Megan Twohey, or The Wall Street Journal essay, “TikTok Diagnosis Videos Leave Some Teens Thinking They Have Rare Mental Disorders,” by July Jargon are exemplars.
Social media focuses on the “person” and navigating them to topics they are interested in and picking what tribe to belong to. The information is flowing into one part of the family system and not to the whole family which triangulates family members against virtual friends or influencers. This occurs if the family is already in a state of constant conflict or conflict avoidance. A recent 60 Minute piece discussed how China does not allow TikTok to bring up divisive topics to their children or adolescents.
For the adolescent to decrease feelings of anxiety and depression, they must work for the “likes” and “views.” They will be trying to affirm their sense of self, but many times they will be accused of bragging and will feel they are not good enough when comparing or competing with others.
Body image and feeling unattractive are especially amplified by social media’s filtering app. Many plastic surgeons are reporting an increase in adolescents wanting to get surgery to look like their filtered self. Current data shows that 55% of surgeons report seeing patients who request surgery to improve their appearances in selfies, up from 42% in 2015. They want fuller lips, bigger eyes, and smaller noses. “This is an alarming trend because those filtered selfies often present an unattainable look and are blurring the lines of reality and fantasy.” (1)
When I’ve met with families and these themes come up, I have encouraged them to discuss these themes which have allowed me to see the systematic position of each family member, system of care and the influencer/algorithm.
Every family has its struggles and at times feels out of control when it goes through a stage of what Monica McGoldrick calls its family life cycle. I have seen this especially when a family enters my office as it is attempting to (re)adjust to the needs of their childhood, adolescent, or young adult. Now add the influence of social media to one or all members of the family, the spiraling becomes more intense.
The importance of free and voluntary play with children to teach them how to give and take has been well documented. There is no substitute for non-virtual relationships in the early stages of childhood. Antithetical to this, algorithms require constant attention, taking the time away from connecting with others face-to-face.
Whether it is the child who requests to go on the smartphone or the parent who gives the child a cell phone in social situations (i.e., play dates, restaurants, long car rides, it decreases the opportunity to negotiate, argue, entertain themselves, compromise, and resolve conflict. This “tech choice” leads to delaying the development of the family and prevents them from moving to the next stage of a family with an adolescent.
There comes a point in families when adolescents are told they are no longer a child, yet neither are adults. For some adolescents, not knowing the initial stages of voluntary and free play puts them into limbo looking for answers. The adolescent and family know on some level they are missing the tools for non-virtual relationships.
First, this is where the social media’s algorithm and influencers potentially intensify the family’s struggle. When the adolescent looks to social media for the answers, this intensifies conflict. Naturally, the adolescent wants to grow away from the family. They want to connect more with peers.
The adolescent in families with intense enmeshment/disengagement and different forms of coalitions struggle the most. This is where social media’s algorithms direct the adolescent to find a group. The algorithm pulls the adolescent in to spend more time on their app, resulting in the app making money and the adolescent searching for connections separate from the family.
However, virtual connections encourage the same patterns of enmeshment/disengagement and the different forms of virtual coalitions. These intense virtual connections are sometimes in opposition to the non-virtual relationships of the family and/or community.
Secondly, this social media generation has grown up learning to communicate more virtually and less in person, especially during COVID. Many adolescents have decided that they would rather communicate virtually. It is hard for some adolescents to look into someone’s eyes, read body language, and feel the energy of being in proximity because it makes them anxious. Look at any lunchroom at any local high school. If the school allows students to be on their phones during lunch, adolescents prefer to spend time on their phones working to maintain a social virtual hierarchy.
Social media offers a prime context for navigating these tasks in new, increasingly complex ways: peers are constantly available, personal information is displayed publicly and permanently, and quantifiable peers’ feedback is instantaneously provided in forms of ”likes” and ”views.” (2). Many of us who grew up before social media can only imagine if our mistakes were on a permanent record and followed us around for the rest of our lives, never allowing us to move forward.
Thirdly, the family does not have a chance to limit the adolescent’s time on the apps because the social media’s algorithm encourages constant attention, reinforces isolation from family and non-virtual friends.
Many parents have approached me saying, “The phone is their lifeline to manage their anxiety,” or, “The phone is the only way they connect with their friends.” During these moments, I have found it useful to explore how the whole family has come to the belief that the social app has become a way to maintain the homeostasis of the family.
I often ask families about their virtual and nonvirtual family maps. I think it is important that we ask the family about their social media involvement to understand the virtual map of the family. Do families understand the impact of the social media algorithm? Do families know how to get out of the social media web? Do we ask each member of the family who they talk to virtually or non-virtually when they are struggling?
In initial evaluations, I often explore if the family is aware of how many hours they are spending on the social media apps. It is important to assess if the family is aware of how much social media raising/influencing is involved in the marriage, parenting, and sibling subsystem. Some providers want to focus on social media addiction, but the algorithm is not like any other “addiction.”
The algorithm allows many of the family members to covertly — and sometimes overtly — bring influencers into conflict with different members in the family. These virtual relationships amplify the family’s symptoms, and unfortunately today’s therapists use the medical model to diagnose the adolescent symptoms, further pathologizing and pushing the relationships in the wrong direction. This narrow view further sets the enactments, reinforcing the enmeshment, disengagement, and coalition patterns.
Non-Virtual Family Map
It is hard to shift our medical model training from a focus on the individual’s (child, parents, siblings) deficits to one that acknowledges strengths and competencies within individuals and the family system. When individual therapy does not make significant change, families often turn to family therapy as a last resort.
After experiencing this different approach, they often express frustration that they were never given the opportunity to move forward together, instead deferring to the experts for the correct intervention and diagnosis.
Structural Family Therapy was so different in the 1970s and 1980s; it was transcendent. While many new theories of family intervention have reached the mainstream, so too have many reverted to focusing on the individual. When starting individual therapy with the adolescent, I have found it important to ask the adolescent to overcome the algorithm on their own without their parents’ involvement. As family practitioners, we need systemic thinking more now than ever to approach the intense cultural impact of algorithms and influencers.
Below is a “traditional” family map that does not consider social media. It represents a compilation of families I’ve seen in therapy, rather than any one family. The symptoms include those typically seen in family practice — poor school performance, school avoidance, vaping, drinking, and using drugs.
From a system’s orientation, the symptoms are a result of the functional and dysfunctional interactions within the family system.
.png)
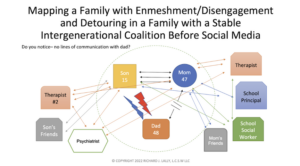
It’s hard for me to understand how therapists begin assessment and treatment without considering or involving the whole family. Some clinicians might say the conflict is too high, and it would only impact the adolescent negatively. Others might assume from the start that one or both parents are not willing to work or are too busy. Some might even be unaware of the importance of beginning from the position that families do not have the strength to make change.
Sometimes therapists and school staff buy into and reinforce the belief that the child or teen is the problem. In the case of this particular map, Mom “reportedly” goes to her private therapist while the son sees his own therapist. Mom and son separately complain about dad to their respective therapists and to the school staff. When mom and son voice frustration about dad and each other in the individual therapy session, disengagement with dad is reinforced. Mom and son are trying to get the type of connections from the system of care that they cannot get with Dad.
While this disengagement takes place, the son turns to his peers, attempting to pull away from mom’s enmeshment, activating her to pursue more. At home, Dad complains that his wife and son always bring up their therapist who agrees that he is unavailable and/or flawed. When this occurs, Dad becomes more distant and angrier, feeling like he is the odd person out.
When Mom gets angry at dad, she turns to her son and vents to him which activates him to challenge his father about money, drinking, and the way he treats her. At other times, the son may jump into the conversation when the parents interact about money, drinking, or the way he treats Mom.
When I attended graduate school, the common exercise was to map the triangles in the family system. Based on the above map, there are at least 24 triangles that are activated in the family-school-mental health system. The 24 triangles are:
These 24 triangles are at the same time difficult for adults in the family to appreciate, even harder for an adolescent, and deeply challenging for the clinician to manage. In those triangles within the family where cross generational coalitions are activated, the symptoms in the family increase. I have often been challenged whether to discuss the impact of all these cross generational interactions with the family and whether it is important to differentiate the healthy, less healthy, and unhealthy ones from each other
On top of the above complexity, other questions arise like “where did the boundaries go?” The therapist must keep in mind how the boundary between the family and the outside world becomes invisible and the symptoms become more intense, to the point more professionals are recruited to “fix the dysfunction.”
I have also had to maintain awareness of how managed care’s enforcement and reinforcement of the medical model has influenced me and other members of the community of care, including other therapists, psychiatrists, physicians, and schools. This reinforcement has an impact on the family’s interaction with the son focusing only on his diagnosis and the correct medication, while failing to address the family relationships.
As mom turns to the school and the system of care for answers, things are not changing. She reports that her son is getting worse. Mom blames dad’s aloofness and dad blames mom’s overindulgence. Mom increases calls to the psychiatrist. The psychiatrist adjusts the medications frequently. The frequency of crises increases and the boundaries between the family and the outside world are dissolving due to the interaction between the family and the system of care.
The number of alliances increases between different family members and different professionals as more professionals/agencies are pulled into the drama. Professionals unintentionally begin to write/rewrite the individual’s and/or family’s stories, especially when utilizing the medical model.
With more stories, there are more opposing interests for each family member. This phenomenon between families and agencies is a result of a collision when both parties collaborate to uphold sociocultural trends. The goal is not only to interrupt multiple unhealthy alliances with existing professionals/agencies, but to also prevent new transactions from developing. (3)
This phenomenon was usually seen when the system of care worked with economically challenged families. We now see this also occurring with families of significant means because they can afford an individual therapist for each family member and psychiatrist(s) if needed.
As we look back at the map, it is now easier to understand that because the family has already identified what they think is the problem, it really needs to address the triangle between mom, dad, and son. It doesn’t really matter where to begin. A clinician can enter through mother-son enmeshment and coalition, father-son disengagement, or parental/marital disengagement.
It might also be useful to address the system of care coalitions between the therapist and school with the mom and son. Having the family identify how to change the interaction between the whole system allows them to move forward. It may be a challenge because getting directives from an expert, rather than looking within their own system, is what they have come to expect.
Using a Virtual Family Map to Identify Issues in Families
Before talking about the influence of social media on the family, it is important to acknowledge some of the “players” in social media. The system of social media has many parts. Social media success is dependent on an algorithm, which encourages frequent interactions by virtual and non-virtual friends.
The frequent interactions result in the shareholders receiving monetary return on their investment, the employees maintaining their jobs and bonuses, and the advertisers increasing the visibility of their product resulting in increased sales. The influencers are dependent on social media to reach as many people as possible to receive income from the app. There is a lot of pressure to have an effective algorithm to support social media.
As you next look at a map depicting the interactive nature of the family and social media, it is important to keep in mind that the 24 triangles from the non-virtual map are still present, and the family boundary is already disintegrating with the school workers, friends, and therapists to seek help with the identified patient.
Now in addition to these non-virtual professionals and friends, the family is inviting social media’s virtual friends and influencers to seek help with the identified patient. Clients (and non-clients) often turn to virtual friends and influencers to provide the same connection as non-virtual friends, but these connections are void of physical closeness. Children and adolescents believe a virtual relationship can replace a non-virtual relationship. But all virtual relationships are void of physical closeness in which touch, eye contact, and a warm smile can feed the soul.
The family can turn on a social media app at any time of the day or night and the outside world is invited into the family, increasing the number of triangles exponentially. From the clinical perspective, it is critical to examine what actions (social competition, social comparison, loneliness, etc.) in the family trigger a member(s) to invite social media into the family. The therapist must also discuss how social media algorithms are activating/triggering the member(s) of the family to turn to an app to surf or post an event. This increases the time spent on the smartphone to maintain these virtual friends, non-virtual friends, and influencer relationships.
At times, social media decreases connection with non-virtual relationships and increases the connection with virtual friends and influencers. In the therapy session with this particular family, some members discuss how they rely on virtual friends and influencers more because “they understand me more than the friends in my own town/school.”
The adolescent believes these virtual figures want to listen to them more than family and non-virtual friends. It is important to ask the family what influencers and virtual friends provide that their own family members or non-virtual friends cannot. This allows the clinician to address the patterns and interactions in the family.
In the map below, I do not draw the number of different social media apps, influencers and virtual friends who are involved with the family. However, I do recommend when meeting with families, to draw each app, virtual friend, and influencer to show the number of triangles the family is managing or attempting to manage. For simplicity’s sake, I use one (black) box to represent all the social media apps and one box for all influencers and separated mom and son’s virtual friends.
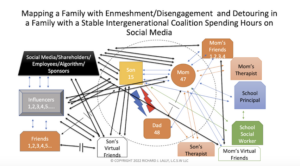
Husband, Wife, and Social Media Triangle
What is the impact of social media on marriage? The wife turns to social media and influencers to figure out how to “fix” her marriage. The wife tries to talk to her husband about what she has learned about marriage on social media. The husband discounts the wife’s attempts to “educate him about marriage.” She eventually gives up on the marriage and “wants to focus more” on her son. She also tries to connect with previous friends and boyfriends from past life because she feels lonely and alone “looking for a connection.”
What you will see in this triangle, and all the triangles which involve social media, is a substitution of a virtual relationship for a non-virtual relationship whose connections are full of conflict or conflict avoidance. The virtual relationships convey an illusion of meaningful connection, but the person(s) feels alone and lonely because it lacks the important ingredients for a fulfilling relationship.
Mother, Father, and Social Media Triangle
Now the wife stops working on the marriage and focuses on parenting. The husband is not aware of this decision, focusing on “making money to provide food, clothing and shelter.” The father continues to feel alienated, disconnected, and disempowered, becoming angry towards the mother and son. The mother turns to school staff, therapists, non-virtual friends, virtual friends, and influencers for ways to “fix her son.”
This fosters more of an enmeshment with son, and disengagement with Dad. The son turns to school staff, his therapist, non-virtual friends, virtual friends, and influencers. Each family member describes a feeling of disconnectedness trying to overcome the feelings of being lonely/alone. Dad voices his frustration, complaining that he is “old school,” and they are “hypnotized by that damn phone.”
Mother, School, and, Social Media Triangle
In this triangle, mom calls the teachers and guidance department for support. She has frequent phone calls with the guidance counselor because the guidance counselor “is an expert with adolescents.” As you can see, dad is left out of the interactions with the school.
After a few months, her son’s behavior is not changing, and mom is frustrated with how the school is not helping her son. Mom begins to turn to social media looking for answers. Mom spends hours on the app talking to non-virtual friends, virtual friends and reading/commenting on influencer’s posts. Mom displaces healthier activities with time spent on social media. Mom begins to complain that the school is not meeting the goals set out by the Individualized Education Plan (IEP). Mom cites information from influencers from social media and the internet. The tension rises between the school and mom.
Schools today are under tremendous pressure to perform. Schools are understaffed, and do not have the mental health training or support to bring in a countercultural systemic approach into the schools despite the money being put into schools after COVID-19.
Parents, Son, and Social Media Triangle
Mom is spending hours on social media looking for answers to why her son is struggling. She also spends time looking for connections. The son also spends hours on the app interacting with non-virtual friends, virtual friends and reading influencers’ posts.
Mom pursues the son, but he only is aligned with her to challenge dad’s limit setting. When the parents attempt to be aligned, the son acts out more. We see the son increase his conflict with parents, who struggle due to their enactment/conflict avoidance with each other on how to help their son. This results in the father leaving and the mother turning to social media to find answers or overcome feelings of loneliness.
When the family interactions are in intense conflict or conflict avoidance, many children, adolescents, and young adults get most of their answers from non-virtual friends, virtual friends and influencer’s posts. The son is seeking temporary relief by getting information and trying to affirm a sense of self.
The non virtual, virtual relationships, and influencers introduce beliefs that are the opposite of the family’s beliefs and further impact the self-esteem of the adolescent. The son discusses what he learns from social media of what “real parents are like.” The decrease in face-to-face communication with family increases his anxiety, depression, irritability, and intrusive thoughts. This also confuses the family of how their family member can “think so differently.”
Son, Non-Virtual Friends, and Social Media Triangle
The son in the session discusses constant social competition/comparison, working for social currency, and thinking he at times is invisible to his non-virtual friends. The son gradually believes his non-virtual friends “don’t understand.” He believes he cannot turn to his parents because “What do they know?!”
The son begins to engage in the same interactions with his peers as his parents and avoids turning to his peers for support. The son begins to spend more time on social media with virtual friends and influencers to seek select information that matches a narrow/closed view, hoping to avoid conflict/interaction. The son then turns more to virtual friends and influencers for answers. Again, this increases his time on his smartphone and increases the family’s sense of not being good enough for each other.
Remember, the son believes there is “less stress” getting information from a stranger, pop culture icon, or a virtual friend than an enmeshed mom, disengaged father, or face-to-face with a peer(s). However, the decrease in face-to-face communication with family and non-virtual friends increases his anxiety, depression, irritability, and intrusive thoughts.
Despite the time spent on social media, the son feels alone/lonely, looking for emotional, face-to-face and physical connection, but does not have the words to express these thoughts to each other.
Mom, Therapist(s), and Social Media Triangle
Dad continues to be absent from the triangle that involves the therapist. The mother attends her own therapy and attends her son’s sessions to discuss what new information she has seen on social media.
She reviews with both therapists what she has learned on social media about new treatment, new medication, and new diagnoses. She advocates with all providers that her son is incorrectly diagnosed, hoping that would help him with his symptoms. The quality of training of the therapist determines their response to entertaining or challenging mom’s research. This may result in mom seeing a new therapist.
The individual therapists and psychiatrists are not looking at how the parents avoid “getting on the same page.” They are reacting to reports by mom about the son’s behavior. Mom and dad are unable to interact differently because they have not figured out how to work together to decrease their son’s phone usage to increase his time with non-virtual friends. The professionals are avoiding addressing the parent’s avoidance!
Mom, Psychiatrist, and Social Media Triangle
Dad is absent from the triangle that involves the psychiatrist. Mom becomes disgruntled with the psychiatrist. She begins to challenge the psychiatrist’s diagnosis and medication recommendation. The psychiatrist recommends if mom is not satisfied with his assessment, she seek a second opinion. Mom begins to look for a psychiatrist who agrees with what she has read on social media.
Son, System of Care, and Social Media
The son is seeing his individual therapist 1-2 times a week and his psychiatrist once a month. He is also spending 2-8 hours on his social app each day. The therapist has not assessed the hours the son is spending on his phone. The app is only showing views/opinions/likes/images that interest him.
The son begins to complain that the therapist does not understand him and challenges his therapist saying, “This doesn’t help.” When the therapist explores the son’s statement, he begins to discuss information from “reliable sources” from social media and influencers. He too begins to diagnose himself and discusses medication that can help. When the system of care discusses reliable sources such as universities and professional journals, the son becomes irritated saying “I don’t want to read them.”
Son, School Staff, and Social Media
Not only does the system of care increase their sessions, but the school staff increase their time with the students. The number of triangles with the son in the school increases between the child study team, teachers, and administration.
The teachers are pursuing him to get his work done — offering to meet him before school, lunchtime, and after school to complete his work. He never shows. The son is seen in class on his phone. Some teachers ignore him, and others nag him. When a teacher challenges the time he is on his phone, he tells the teacher other instructors let him do it.
The social worker is calling him down to discuss his avoidance of work and disruptive behavior in the classroom. Only when the son becomes overwhelmed, he discusses with the school social worker his home life and that medication is not working. The vice principal is meeting with him to give him detentions. The son feels frustrated with the school stating, “They are only doing this because it is their job.”
Son, Non-virtual Friend #1, Non-virtual Friend#2 with Social Media
The son leaves school to go home to continue to work on his non-virtual relationships on social media. It becomes evident that in social media apps, the same social stressors occur online like in school. It is exhausting to navigate being included and avoid being excluded at school and online. The son and non-virtual friends are jockeying for social currency and social position, never getting time off to charge their own social battery.
The son and non-virtual friends stress about the images they post. They are anxious about what the image means to them and others. The son is trying to understand the unspoken rules for posting and the reaction by his peers regarding the image. The son worries if the image appears “authentic” and will help him maintain his position inside the social media group or if a new group be formed without them.
Son, Non-virtual Friend(s), and Virtual Friends
The son struggles connecting with his non-virtual peers. He is not getting feedback from his non-virtual friends about his art and his physical appearance and finds out they have different chat rooms that do not include him. (Remember, he does not want feedback from an overly involved mom or detached father.)
He begins to look for feedback about his art and physical appearance from virtual friends. When looking for connection outside the non-virtual friend group, he states he is looking for virtual friends who are nonjudgmental.
But as time went on, it began to mirror the non-virtual group. Some of his virtual friends on social media become competitive and attempt to increase their social currency on this platform. They do this by making fun of his physical features and his art. This mirrors some of his non-virtual friends’ behavior. The son frantically searches for another virtual peer group that he believes will not activate anxiety by not challenging his views, providing a stress-free venue.
As the son increases his time searching for virtual peers and influencers over non-virtual friends — reinforcing a closed system, increasing isolation at school, and decreasing time to sleep at home. His virtual relationships are now more important — increasing time spent on the app and continuing to strive for more likes and views.
Lack of face-to-face contact with family and non-virtual friends fosters more of a virtual enmeshment with virtual friends. He describes them as “nonjudgmental” and “more accepting.” This further increases his self-doubt and increases his feelings of loneliness and creates a virtually closed system (Virtual Enmeshment).
Son, Virtual Friends, and Influencers
The virtual group is important to maintain when avoiding contact with his parents and non-virtual friends. The son describes his virtual friends as more “authentic” and describes his non-virtual friends as “fake” and “not genuine.” However, some of his virtual friends on social media become competitive and attempt to increase their social currency.
The son frantically looks for another group that is an anxiety and stress-free venue. This further increases his self-doubt and increases his feelings of loneliness. This increases the symptoms of anxiety and depression when waiting for approval from virtual friends saying, “They are the only ones who understand me.”
As the son looks for new virtual friends, he and his virtual (and non-virtual) friends look to influencers for answers on how to portray themselves. Influencers work hard to establish and maintain their position in their virtual community. The influencers are working hard to make money and increase their viewership. The influencers often ask adolescents to agree with their beliefs and recommend products they are selling. The influencers work hard to appear on the “right side” of an issue.
As the son tries to replicate the beliefs of his preferred influencers, he looks for fellow virtual friends that have done the same “research.” They notice the more they make comments in opposition to a belief, it increases their views and likes.
As the symptoms in the family increase in intensity, the members increasingly must decide who to align themselves with in the virtual and non-virtual triangle. The therapist highlights this and encourages the family to discuss and identify the boundaries of virtual and non-virtual triangles that maintain these alliances/symptoms. This allows a family to discuss non-virtual triangles that are underutilized, which reinforce healthy boundaries that benefit the family.
Using Exploring Questions to Make Circular Statements
Much has been written about joining, unbalancing, and mapping in SFT. One of the beautiful ways Structural Family Therapy (SFT) uses language is by employing circular statements to connect the family member’s behavior in the system. When SFT enters the family, the systems therapist uses the family’s own observations to connect their interactions.
It is important today to make a circular statement to widen the lens in which the family sees how all virtual and non-virtual relationships impact the relationship in the family. Below are some examples of circular statements using the words used by each family member.
I agree with you, Mom, that as long as you do not have a voice with Dad and work together, your son will not stop posting explicit images on Snapchat
Dad, as long as you sound like a drill sergeant, Mom will not find her voice as a woman and work with you as a wife and mother of your son who will continue to believe he must mirror images on Instagram
Mom, I agree that the harder you work, the less Dad helps you with parenting your daughter— your daughter will have to turn to influencers about how a woman should look and act
Peter (son), as long as your mom is worried about the frontstage appearance, she will fight with your father who is more concerned about your backstage struggles with you and your mother
What do your virtual friends give you that you cannot get from Mom, Dad, or your non-virtual friends?
Many are worried about the continued increase in suicide, suicide attempts, and mental health issues in the family and how Congress is powerless to challenge these companies. Many providers are not looking at what has changed in our lives in the past 25 years.
Relationships are becoming more complicated than ever. Many families and therapists are unaware of the impact of the system of care and less aware of the impact of the ubiquitous “algorithm.” It is hard to understand how the algorithm works because it is important for these companies to keep the algorithm secret for fear of losing profit.
We must also remember that each influencer, virtual friend, and nonvirtual friend has their own family map. Just as many professionals do, influencers understand how their stories, views, and images echo in the family.
Are families aware of the alliances that occur with virtual and non-virtual friends and influencers? Are we aware that when more virtual influencers and friends enter the family, more alliances increase establishing social hierarchy, increasing social competition and social currency? Are we, the clinicians, aware that influencers and virtual friends unintentionally/intentionally begin to write/rewrite stories in the family and permanently on the internet?
We must begin to understand that with more stories, there are more opposing interests for each family member. This phenomenon between families, virtual friends, nonvirtual friends, and influencers (social media) is a result of collusion when all parties collaborate to uphold their preferred sociocultural trend.
The goal is not only to highlight and interrupt the multi-alliances with existing social media but to highlight the transactional pattern in the home that maintains this pattern. Remember, a virtually closed system impacts all family members, whether one or all are using these platforms excessively.
References
(1) Susruthi, R., Myara, Maymone, B. C. & Vashi, N. Selfies-Living in the era of filtered photographs. JAMA Facial Plastic Surgery. 2018 20:6, 443-444.
(2) Nesi, J. (2022) The impact of social media on youth mental health: Challenges and opportunities. North Carolina Medical Journal, 81(2), 116-121.
(3) Colapinto, J. (1995) Dilution of family process in social services: Implications for treatment of neglectful families. Family Process. 34:59-74.
Questions for Reflections and Discussion
How has social media influenced your personal and family life?
How does the author’s premise resonate with you and the way you practice family therapy?
How have you integrated social media and app use into family therapy?
In what ways do you agree or disagree with the role of social media in family systems?
© Psychotherapy.net 2023
Information is a difference that makes a difference.
— Gregory Bateson
In nature, it is said that whenever there is a poisonous plant, there can be another nearby which contains its antidote. When it comes to helping families, the same is true that for every problem identified, the resources for resolution can be present somewhere in the family’s ecology.]
Unfortunately, especially for underserved families, competition among divergent treatment philosophies, practices, and limited resources create an unintended conspiracy within the mental health and social service delivery systems — perhaps a benevolent one, but one which nonetheless curtails the identification of systemic homeopaths. The unfortunate consequence of this inability to use potential “antitoxins” naturally present within the client’s ecosystem is inefficiency for the service delivery system, stressed-out workers, high turnover, burnout, and a spiral of reduced possibility in which hope’s grasp is tentative at best, and non-existent at worst.
Mental health and social service clinicians working within the childcare system must search for strengths and solutions that are present, though perhaps hidden, in clients’ ecosystems. The approach is based on systems thinking and the idea gleaned from the practice of Structural Family Therapy (SFT) that change in any system, whether it be a family system or a social services agency, is best affected by the lived experience of doing.
Crossword puzzles as a paradigm stresses thinking and doing as an “out of the box” means to a problem-solving end. This practice mines the strength-based belief of creating a “virtuous circle” — one which recognizes clinicians’ and supervisors’ capacities and creativity, like those of the families they serve.
In resource-poor environments, when the goal of training is the enhanced ability to search for strength, this is not simply a training “add-on.” Rather, it is a foundational principle that requires the same persistence and consistency that Minuchin and other family therapists demonstrated was present in the natural environment in which clients and their families are embedded. The naturally occurring strengths in clients’ ecosystems can be uncovered by robust “doing,” which is an optimistic and energetic search for resources and resilience within both the family and the larger ecosystem of change.
Like the proverbial butterfly catcher with net in hand, human service organizations have long been involved in a quest to capture the elusive chrysalis of change. What distinguishes efforts at reform and the ability to succeed is an ecological, “whole systems” approach. Children, families, problems, and possibilities are viewed in toto — economics, social, political, educational, gender, vocational, racial, location, class, and psychological elements are all in play. It acknowledges the margins and builds accountability.
The human and fiscal expense of doing otherwise speaks to the futility of programs that do not account for the organic and sometimes chaotic environment that families attempt to survive and thrive in.
As the 19th century Prussian Field Marshal Helmuth Carl Bernard Von Moltke reminded us, “No plan survives contact with the enemy.” In this instance, the enemy of high-quality service delivery is the tendency to replicate the existing system rather than undergo the reformation needed to absorb the family’s own healing powers.
Another systemically inspired practice that infuses underserved families with greater choice, and ultimately health, is collaborative case planning. This time-honored intervention gets all the major players to the table — including the family — and in the process, becomes a kind of exercise in agency topography that borrows from the tradition of Hartman and her colleagues, who pioneered ecomapping of family systems for adoptive placements.
By using the wide-angle lens of mapping families in all their contexts, resources and potential pressure points can emerge for their potential effect on the child and family. From the agency perspective, efficiency and collaboration are increased with an ecomap; everyone can see who is doing what and when and how it is being done. As a form of “observational therapy,” an ecomap can have the same heliotropic potential. However, as business has learned, outcomes can be improved, but not always for the reasons one might think.
Unfortunately, the promise of systemic work and its healing potential as envisioned by therapists who worked in the family trenches is not always realized in the battles to transform larger systems. For clinicians in the human services, or for those who train them, the pitch of a systemic perspective too often mirrors the president throwing out the first ball of baseball season — well intended, lots of hoopla, but doesn’t reach the plate. Without a clear picture of where they fit in the larger service-delivery system or a sense that they can make a difference, workers can feel overwhelmed, disempowered, and disheartened.
The financial cost to the system in turnover and lost productivity can be measured. The loss of wisdom, the discontinuity of care, and the loss of hope, however, are beyond calculation. In that regard, the experiences of child welfare clinicians mirror the isolation that can permeate the system within which they work and the families that they treat.
It is for this reason that systems of care were re-designed to “wrap” services around families and to minimize the dilution of family processes that occur as a by-product of traditional service delivery. In a sense, “wrapping” can enrich underserved families with a wider net of resources in the way families of higher classes can choose their providers and supports more selectively.
In tracing the strands of effective, systemically inspired service delivery, there is one constant thread: strengths. Thank goodness! But just as it was found that a rising economic tide does not raise all boats, so too can the tidal waters of strength not elevate the all-too-often porous vessels of bureaucracy.
What is amazing is how far a little strength can go, even in conditions that are wanting. There are, after all, some quite beautiful plants that flourish in the shade. Sadly, however, in the wrong bureaucratic hands, even strengths-based practice can invite the agency equivalent of Frankenstein picking flowers with the little girl — it’s a nice idea, but eventually the monster kills it.
How, then, to help clinicians to see that “It’s the difference that makes a difference”? Is there a way to aerate the sometimes root-bound tangle of the childcare bureaucracy so that its ability to heal can be given the room to breathe and prosper? How to give clinicians — especially those just out of school — the understanding and confidence to “trust the process” of searching for strengths, both within disrupted families and the systems designed to serve them? Moreover, are there ways to create a culture of caring and learning transfer so that clinicians see themselves as “action agents” within the larger bureaucratic tangle?
Part of the answer lies in family therapy’s history and co-development with cybernetics — the study of how systems developed the concepts of circularity, non-linearity, recursion, the process of self-correction, and the ways family and organizational systems maintain stability/homeostasis while balancing that with change and transformation. Gregory Bateson and his colleagues at the Mental Research Institute (MRI) in California, along with other early adapters, were the pioneers in this new way of thinking that set the stage for family therapy as we know it today.
Using a notion central to Structural Family Therapy (SFT) about strength and extending it to conceptualizing strength as a verb can be unintentionally overlooked when children and families in dire need get lost within the morass of bureaucracy. The SFT concept of healing is more about thinking of strength as a verb. It’s not so much a matter of finding strengths within the family’s ecosystem as it is strengthening the resources that are hiding in the weeds, so to speak. In that regard, it is more of a leap of faith — that whatever challenges a case presents, health can prevail.
Businesses and non-profits share a challenge: getting their message through environmental “clutter,” or the glut of choices that compete for our attention. How, then, can human service organizations solve the multiple staff training dilemmas they face?
The skills and belief set needed are interwoven and important: ensure the safety of the child and family, reduce decision clutter, increase the active search for strengths, attend to and nurture family connections, expand the problem-solving lens to include extended family, community and idiosyncratic, home-grown resources, and get paperwork in on time. One path on the way toward answering this organizational koan is this: increase experiential capital by linking the worker and their day-to-day decisions with the larger mission of the organization.
Bridging the gap between what we know and what we do, however, is no small feat. In Why Didn’t You Say that in the First Place: How to Be Understood at Work, Richard Heyman unravels this knotty problem with a question and a refreshing answer: “Why is it that ‘a picture is worth a thousand words?’ The picture is not talking about something — it is the thing the talk is about.”
From this perspective, to truly “get” the uber-goal of searching for strength and translating that into action, workers must experience the “felt sense” of search and discovery —finding something where apparently nothing exists. This experience is analogous to an “enactment” in SFT, in which the family is guided by the therapist in an interactive experience between members that is designed to offer them new opportunities to use underutilized strengths.
Many consider enactments to be the heart of Structural Family Therapy. The value of enactments is two-fold. First, as a “real-time” assessment tool, and second, for their change-producing potential, both of which scaffold nicely for training in human services.
Enactments between family members during therapy can principally occur in two ways, either spontaneously or through the therapist’s direction, and they are used in two ways, to assess family patterns and to promote change. Spontaneous enactments are readily available ways of interacting that might be thought of as familial “tells” (like the poker player whose nervous smile foretells the bluff), showing habits of relating in which relational organization is embedded. While some might consider these patterns to be so deep as to be unconscious, another way to think of them is as learned ways to relate and survive in the world.
The persistence of patterns can transcend the pull of context. Habituated behaviors tend to reveal themselves in multiple settings— a therapist’s office, a restaurant, school, work, or home. The persistence of these patterns can be linked to the tendency to reduce anxiety through prediction and habit. As the pioneer family therapist, Virginia Satir notably said, “Most people would prefer the misery of certainty over the misery of uncertainty.”
Like an artist who steps back from the picture they are painting, clinicians have the capacity to use themselves differentially, moving in and out of the family system to gain perspective. Minuchin described this as “use of self,” in which the therapist positions themself with the family from “proximate, median or distant” perspectives.
Harry Aponte has written about how therapists can make use of their own personalities, family of origin, and life experiences to guide clients during enactments in the “then and there” of limiting patterns so that they experience themselves and one another with increased possibility and hope.
Like a music student first learning scales as a prelude to improvisation, experiential training can evolve into a more responsive, “whole systems, both-and” approach in which requirements and innovation can co-occur. For example, when supervisors at one county office of a state child welfare agency were asked about their staff’s training needs, their response was, “To be able to think on their own/to think outside of the box.”
Their request comes from the experience of guiding their workers through the complicated bureaucratic and interpersonal seas of child protection. As Mumma wrote in his insightful piece about his agency training in systems work, “Taking these concepts (ways of thinking) and making them work in a particular agency setting is the real work of training.” The analogy of crossword puzzles can make that work a bit easier.
Just thinking about all the aspects of a case — its who’s, what’s, and how’s — can be a bit overwhelming. Cases in the investigative and early treatment stages, particularly for newer clinicians and social workers, may seem all forest and trees, abounding with unanswered questions.
Over the years, agencies have found genograms, ecomaps, and structural maps to create a set of “blueprints” that graphically represent families and agencies in a way that quickly sorts out relationships and priorities. These tools have been essential in widening the practice/thinking lens to include others who may have clues to potential resources.
The rise in “manualized” treatment and the emphasis on evidence-based treatments has helped to sort through these difficult choices and prescribe “best practices.” While this is a necessary step in the right direction — much like learning scales is in music — it can be insufficient to encompass the unpredictable nature of cases. There needs to be a “both-and” approach that brackets safety, consistency, and growth with improvisation. Thinking in terms of crosswords can do just that.
In its own way, a blank crossword puzzle graphically resembles a complex clinical and, in this case, social services-related case — lots of questions, some inter-related, some not, and just to make it interesting, a few black boxes. As President Clinton said in the crosswords-based movie, Wordplay:
Sometimes you have to go at a problem the way I go at a complicated crossword puzzle. You start where you know the answer and you build on it and eventually you unravel the whole puzzle. And so, I rarely work a puzzle with any difficulty, one across and one down all the way to the end in a totally logical fashion. A lot of difficult, complex problems are like that. You must find some aspect of it you understand and build on it until you can unravel the mystery you are trying to understand and then you build on it and eventually you unravel the whole puzzle.
When one acts as if the answers are there, though perhaps hidden, the puzzle’s resolution moves from the shakier, contingent ground of “if” it will be resolved, to the more possibilistic ground of “how.”
Do you think I know what I am doing?
That for one breath or half-breath I belong to myself?
As much as a pen knows what it is writing,
Or the ball can guess where it’s going next.
When a case opens in child protection, the most compelling, sometimes unanswerable question is “Who will keep this child safe?”
If an injury has occurred in the home, the prima facie answer may seem obvious: “no one.” In this instance, unless resources are surfaced, the child will need to be placed outside of the home, “in the system.”
Starting the exploration of strengths from a crossword paradigm assumes that like the printed puzzle, all the answers may not be initially apparent, but once safety is established, one can begin to answer the eternal risk-safety dilemma: Can the person(s) who caused or permitted harm now be responsible for safety? If one only looks at the alleged abuser, then the likelihood is that the answer to the question will be “no.” If more contextual factors are also considered, so, too, are possibilities.
The work becomes both retrospective and prospective, invoking Einstein’s dictum, “You can never solve a problem on the level at which it was created.” The “who” and “when” questions are now also answered by “how.”
The “how” to find and fill those potential strength-based empty boxes begins with questions like “Who else watches the kids when you go out?” or, “When you are having a rough day, who do you talk to?” or, “Who are some of the people you count on?” These ground-level questions are more than a set of techniques, they are the personal implementation of a larger policy that has the capacity to both be safe and value the child’s primary connection.
Like the Zoysia grass, the grass/weed whose initial plugs merge over time into a uniform carpet, training from a Crosswords perspective can grow the seeds of organizational interpersonal attachment. One way to underscore the marriage of mission and method is to give training participants a felt sense of difference.
The enactment of possibility begins when participants fill out a blank crossword on their own. After five minutes of working alone in silence, the trainer helps the participants process their “silent” experience at multiple levels: What did you notice? Did you fill in the boxes you knew first, or did you have a system? What did it feel like? Did any of you get stuck? How did you get out of that — what did you do? Typically, people report a range of answering strategies — some very methodical, “I do every ‘across' first, then I start with the ‘downs,’” others more radiant, “I just see which ones I know and then go from there.”
Next, the trainer asks the participants what it felt like to do the puzzle. What did they notice about their mental/emotional and physical states? “It was quiet.” “I kind of got into it.” “It was frustrating.” “I felt tense.” “I was worried other people would see how much I didn’t know.” “I kind of enjoyed it.” “It’s like Solitaire or Wordle, I just got lost in it.” All their answers provide abundant raw material to talk about their work, their stresses, successes, and the strategies they use to problem solve. And it sets the stage for helping them think “out of the box” by using the other boxes.
To widen the lens, the trainer may provide another enactment. This time, they can ask participants to form small groups of six or fewer, telling them that they have another five minutes to work on their puzzles, but this time, together. People begin to talk, share their answers, laugh, and fill in the blanks as they see how quickly they can solve the new crossword together as a team.
When the time is up, the group is asked to process their experience and compare it with doing the puzzle alone. Inevitably, they notice the energy level, productivity, speed of producing answers, and their own internal experience of connecting while connecting the dots. In future puzzling cases, this brainstorming model can supply added, shared resource clues to support and, most importantly, help the clinician in their search for resources within the family and larger system.
Materials Needed: Copies of a Crossword Puzzle
Total Amount of time: 10–20 minutes
Lessons Learned: Start with strengths within and around the family, fill in the answers you know to discover the answers you don’t.
One does not need to know all the answers to get all the answers.
A “wrong” answer is eventually corrected by the context of right answers.
Just like a case, one does not know all the answers when starting — answers emerge over time often from unexpected sources.
Persistence pays off — but so does taking a break and getting help.
The first time I (LPM) met Kyla and her mother, Teresa, was across a cold table in an institutional room. Kyla had been in the residential treatment facility for almost ten months following a series of escalating behavioral incidents in her previous foster home. I thought back to my meeting with the family’s caseworker, who told me that Teresa and her partner Linda’s relationship was volatile and created an unsafe environment in the home. Kyla’s father, according to the caseworker, was out of the picture.
During my first several months working with the family, I felt as if very little progress had been made. Each week, I’d pick Teresa up and drive her to the residential facility for family sessions. Dutifully, I went to family court, holding space for an equally enraged and devastated Teresa on the way home each time reunification was pushed back. I consistently showed up for the family, and despite good rapport with both mother and daughter, Kyla’s behavior remained a challenge and our family sessions felt focused on the crisis of the week, as opposed to addressing underlying family dynamics and struggles.
One day, Teresa unannouncedly brought her partner Linda to session. From that point, treatment changed almost immediately, as both Kyla and Teresa seemed more engaged and open during family therapy, and we began to focus less on minor incidents and more on boundaries and communication within the family system.
Still, somehow, it felt like a piece of the family puzzle was missing. I could sense that Teresa and Linda were holding something back, particularly when we discussed their co-parenting practices. This final piece fell into place one day when I went to pick up Teresa and Linda and Robert, Kyla’s father, eagerly and unexpectedly hopped into the van. It quickly became clear that Robert had been actively involved with the family all along.
I finally could see the full picture of the family structure and their dynamic. Teresa, Linda, and Robert were in a polyamorous relationship. Robert had been understandably hesitant to engage with the child welfare system out of concern that the polyamorous relationship would be condemned, and reunification denied.
The case that had “simply” been presented to me as an unreliable mother with a violent partner unable to meet the emotional needs of her unstable daughter was actually one where a child had three caring adults who wanted to support her. With all the pieces in place and the entire family finally engaged in treatment, meaningful therapeutic work ensued, Kyla’s behavior improved, and she came home.
“The solution to pollution is dilution.”
Using crossword puzzles as a conceptual framework and training method opens workers and the organization to both the learned and the lived experience of complexity, strength, possibility, and the importance of connective relationships when working in child protection. We know that systems can mirror the systems that they treat. For instance, In Child Welfare, the insidious nature of poverty is such that it can quietly, but inexorably, leach into the soil of good intentions in such a way that the attachments between worker and family, workers and other agencies, worker and supervisor, and workers themselves, can suffer the pollution of despair.
This is not to say that using crossword puzzles will wall off the effects of these potential systemic toxins. It is to say, however, that healthy, connected relationships can be grown and nurtured and, over time, create “the difference that makes a difference.”
***
The author would like to thank my friends and colleagues who helped me fill in the blanks, both across as well as up and down. A special thanks go to Lauren McCarthy (LM) for providing the case of Kyla.
While it can be isolating, mental illness is not an isolated experience. It affects more than just the individual: it impacts friends, family, spouses, significant others, and co-workers. I recall working with a married man who developed Major Depressive Disorder around the time his wife had their second child. He became emotionally distant, socially isolated, lethargic, couldn’t focus, took time off work to the point of being fired, and lost interest in sex. His wife struggled bitterly. She felt completely overwhelmed with the care of two young children. Her husband, on whom she once depended, was no longer contributing. She felt like she had to care for him as well and try to keep the family financially afloat since she was the only one working. Despite the challenging circumstances, she tried to keep their intimacy intact, but he had no interest in sex, going out, connecting with their friends, and he struggled to track during conversations. As you can imagine, this put a strain on their relationship, which they eventually ended. Neither one of them wanted the divorce, but the wife hit her breaking point, and her husband couldn’t find the energy to fight for the relationship. This is a sad story that is reflective of how mental illness impacts a marriage, a career, parenting, and personal finances.
When working with clients, I try to keep in mind the relational impact of mental illness in all its facets. Mental illnesses, like depression, affect the individual in every sphere of their life, including the social/relational. The above example illustrates how lonely the man felt, and how inexpressible his psychological and physical experience was to his wife. There were no words that existed in his mind or in their relationship for him to utilize. He and she were left in a wretched state of ambiguity. And despite her best efforts, she could not intimately access the depths of his depression. She, too, had no words. She couldn’t prevent feeling shut-out, as if she had been barred from his heart. Her dream was to feel unimaginable connection and joy at the birth of their child, but what she got was facing single-parenting while married.
Needless to say, there is a ripple effect of depression. The man’s relationship with his child will forever be changed. Certainly, it is within his grasp to foster a loving and connected relationship with his child, but he will have to do so with additional barriers due to the divorce, physical distance, child support, navigating co-parenting, and potential co-step parenting.
From my perspective as a clinician, problems are compounded when family and friends don’t understand the nature of mental illness, however, this is not always obvious to my clients and their loved ones. When trying their best to understand their loved one’s struggle, some may conclude that they aren’t trying hard enough, that they don’t care, or that they are seeking attention. Without information, without a sufficient explanation, bad interpretations fill the void, which only lead to judgment and alienation. As a clinician, I step into that void with accurate and compassion-filled information. My aim is to coach clients who are struggling with mental illness as well as their family members and explain that they may be tempted to personalize or create a negative attribution for their loved one’s behavior. It is tempting, natural, and understandable why they would do this, and yet, it is often a mistake in judgment. I try to explain that if their loved one had cancer, they wouldn’t take it personally or judge. Certainly they might have big feelings of sadness or anger at God or the universe, but there would be no assignment of blame to the diagnosed individual. They wouldn’t think, “Why did she choose to have cancer? They must want attention.” That would be absurd, and the vast majority of people would never think this.
So why would a wife, husband, partner, child, friend, or family member personalize a loved one’s depression, anxiety disorder, or phobia? I encourage my clients and their social network to make a genuine effort at understanding mental health disorders. It is natural to want to know as much as possible about a disease when a loved one may be diagnosed with a medical disease. As a clinician, I encourage clients to take that same impulse and learn as much as possible about their loved one’s mental health diagnoses. Ignorance only creates barriers to relationships, and my hope is to remove any barriers to social connection in my client’s way, as well as within their social network. A client is only as healthy as their community. Therefore, I want to empower clients to empower their communities, to mobilize those around them to seek out information and more deeply understand the psychological realities they are dealing with. And to find that middle ground of embracing the mental illness of your loved one but resisting the urge to define them by it.
***
Thinking back to my client mentioned earlier, I wonder how things would have been different if both the husband and wife had more awareness about depression. I wonder how the two of them may have pulled together, rather than apart, if they had known earlier on that the husband was being affected by a mental health disorder. If they had only had the words and concepts to understand not only the husband’s experience of depression, but also the relational impact that depression brought to their marriage and family. The wife was just as much a sufferer of depression as was the husband. This new understanding could have been a catalyst for collaboration, support, mutual understanding, and shared problem-solving.
If there is no plan, nothing can go wrong
Kim Ki -Taek — Parasite
It’s not the strongest of the species that survive, nor the most intelligent, but the one most responsive to change.
Charles Darwin
It’s recycling day, can’t we just put the kids outside on the curb?
Parent — Pandemic, week five
Dude!…You’re Glitching!
Fourteen year old girl on Zoom session
The pandemic has changed the larger world forever and will forever change the world of therapy. Our therapeutic ecology — how we practice our craft, where and with whom — will never be the same. It’s as if we’ve clicked into a science fiction show and can’t change the channel because we’re in it — clients and therapists have become talking heads, connecting as best we can and collectively feeling the fatigue attrition that accompanies the absence of being in person. The Grateful Dead were right: it’s been a long strange trip, especially for the empaths.
Michael is a single man in his thirties. He’s suffered a lifetime of painful shyness and being overweight. His job requires computer skills, so he spends most of his time in his cubicle, with little socialization on the phone or with co-workers. He’s described breaks and lunch as “torture.” Prior to lunch, he would get revved up with good intentions and then, he said, “I’m like Wile E. Coyote chasing the Roadrunner — I hit the wall.” One time, he got the gumption to attend a meet-up group for shy people, and no one showed. Yet, despite these challenges, he’s determined to be more social. Then, something happened. At our last Zoom therapy meeting, he was more confident and relaxed, like he’d just put on old slippers — smiling and even cracking jokes. For me, it was a kind of optimistic disorientation. At first, I thought that it was the combination of medication, his Wile E. Coyote resolve and hopefully some of the therapy that, like the British Baking Show, had produced a slice of Magic Pie. It wasn’t — it was the pandemic.
Because of “social distancing,” Michael paradoxically experienced being together with people while he was apart. Everyone now shared his life — now he could enter conversations with the knowledge that others also shared the taut, jangled wiring of his interior. It was as if he became an Italian apartment-dweller sheltering in place with his neighbors and singing together with them off their shared community of balconies, everyone listening with hearts joined in the absence of judgement and the voices of hope. Better still, because of the imposed distancing, Michael could now be safely social.
And what about therapists — what is this doing to us? Many are working from home. Those of us with children, pets or partners and who don’t have a home office have to find a “quiet space.” Ha! Good luck with that basement, people! Or, if we’re lucky and the landlord isn’t banning entry, we can go into our off-site office space — but that, too, has its own set of Zoomy consequences, not the least of which is “Zoom Fatigue.” By day’s end, sessions can feel like you’re in the front row at a lecture on sofa cushions where the speaker can see you. Just as you start to blissfully nod off, your head suddenly jerks back, and you snort loudly and say something weakly therapeutic like, “really..?” and then wipe the drool onto your sleeve — très embarrassing.
Zooming our client’s home space is not without merit. Back in the day when I was a probation officer in Cabin Creek, West Virginia, and then a social worker doing school evals, and then a research therapist on a project with heroin addicts and their families, I was blessed with being both witness and participant in the amazing diversity of the human condition. You learned to go with the flow and, you swam in the deep end of the family pool — dogs, cats, kids, babies, ferrets, frogs, multiple TV’s, radios blaring, grandparents, people who just showed up whom you didn’t know, dinner on the stove, or a silence that also spoke to you — all this before the age of the Internet. It was so powerful that when I first started my private practice, I would ask families to invite me to dinner and a family session at their home. “Now, we have Zoom — welcome to the shallow end. But we can all still learn to swim.”
You can observe a lot by watching.
Yogi Berra
Peter Lopez, a family therapist on the board of The Minuchin Center for the Family, is a home-based family therapist. On one of his Zoom visits, he wanted to speak to both parents and have an enactment with them that would increase the parent’s executive capacity and demonstrate to themselves and their kids that Mom and Dad were on the same page. In a moment of inspiration spurred by there not being enough headphones for everyone, he asked the parents to “move closer together so you can share…”
Another family therapist, a young woman who works with a diverse population of low-income families and mandated, substance-abusing high-risk teenagers, finds that being “in & not in” someone’s house can diminish her connection and, in some cases, embolden teens to challenge her — like the fifteen year old teenager who greeted her on FaceTime lying in his bed with his shirt off. “Would you do that in my office?!,” she asked, incredulous. “Uh, no, but I’m not in your office….” “Well, when we meet on Facetime, you are in my office!” And then, softer — “So when you put your shirt on we can start, and you can tell me how you’re doing.”
She still delineates the boundaries — for the kids she sees, her office is their safe space. To compensate for the in-person absence, she’s upped the amount of between-session “homework” that she and her clients then share at the next session. Trauma and disconnect are prevalent. A young girl being raised by her grandmother whose mother is absent provided a path in between sessions. Together they came up with an assignment to come to sessions with a weekly playlist of songs that emotionally spoke to the client. The girl picked “How Could You Leave Us?” by NF, which should come with a warning label and tissues — it’s remarkable.
We have to be inter-connected with everyone and everything.
Thich Nhat Hanh
You cannot solve a problem from the same level of consciousness that created it.
Albert Einstein
An informal survey asking therapists to describe their experience of practicing Zoom therapy in the pandemic seems to break into two distinct groups: one, maintaining a kind of Buddhist perspective of acceptance –— that life is suffering and impermanence in which every day is an opportunity to practice mindfully — to another, a bit less accepting — “I fucking hate it!”
Which begs the question — is there a third way? The short answer is “Yes.” And it’s not without precedent. Einstein’s quote is like learning a brilliant escape trick from a gifted magician. The magic is not what is seen or said but in what he doesn’t say. What he omits is the specificity of consciousness — it does not have to be higher or lower, just different. And we therapists are all about being different. To be effective, we access different aspects of ourselves that then activate different and more adaptive aspects of our clients. It’s what Minuchin described as the “differential use of self.” If we want others to be different, then we have to be different. For systems thinking and for family therapy, in particular, those differences in thinking were already in the works well before the pandemic.
Lynn Hoffman pointed out in Foundations of Family Therapy (1981) that “the advent of the one-way screen, which clinicians and researchers have used since the 1950s to observe live family interviews, was analogous to the discovery of the telescope. Seeing differently made it possible to think differently.” And by circular extension, thinking differently also comes from acting differently.
Up until now, we’ve relied on our in-session felt experience, one-way mirrors and videotaping to guide ourselves as instruments of change. One recursive emotional and visual distinction between the now and the then of the one-way mirror’s transformative introduction, is that families could not see the people behind the glass, nor could the people behind the glass see themselves being seen. Videotaping sessions, however, offered a “third” answer, giving therapists the capacity of “seeing” themselves and the family’s patterns in context. It shined a light on how to experiment with adapting interventions systemically and collaboratively. While inventing Structural Family Therapy, for example, Minuchin, Jay Haley and Braulio Montalvo invited family members behind the mirror. They recognized cultural and class differences between themselves and the “natural healers” from the minority community that they were training to be therapists. Minuchin realized that “in order to join, we needed to change.”
“With Zoom however, there is a binding irony that holds therapists and clients in its’ grasp. It is as if we share front row seats watching a mystery play”. The opening scene’s roiling dense fog and dim lights mask the fullness of detail, so we squint, holding our breath hoping to see what’s really there. We’re doing our parasympathetic best to figure out the plot. It’s the work of it that fatigues us and leaves us wondering if this is as good as it gets.
Therapy is therapy as therapy does, but how we use ourselves in this new environment re-boots an age-old clinical question; what exactly is both necessary and sufficient to produce change? Montalvo called the position from which we work “The possibilistic premise.” Meaning that regardless of the location of the family’s pain, we are still faced with respectfully challenging the system’s homeostatic “stuckness.” We know that we can effect those changes in person. When Zooming, however, it can sometimes feel as if we’re “Major Tom,” floating in space, attempting to weld the hull as we circle the earth.
So, as Bowlby, Susan Johnson, the Gottmans and our own families have shown us, the quality and kind of our earthly and relational attachments are important. While we may feel even more like Russian Dolls, breathlessly stacked within each other’s context and the context of the world writ large, it’s not a question of “if” we adapt and attach in different ways, it’s more a matter of “How?” Perhaps as Theodore Reik suggested, we should listen with greater clarity, not just with a “Third Ear,” but now with ear buds. We are finding ways to compensate for what’s lost with diminished sight and the absence of physical presence. Our adaptive make-up is yielding results. However because we are inherently empaths, we feel the absence of presence. But we shouldn’t feel bad entirely. Rumi’s poem, “Love Dogs,” reminds that “the howling necessity” implores us to “cry out in your weakness,” such that “the grief you cry out from, draws you toward union.”
It’s the end of the world as we know it, and I feel fine.
R.E.M.
After not seeing our granddaughters at our house for eleven weeks, my wife and I share a grandparental Folie à Deux — an ache like an old injury that we’d come to accept, now reawakened with every primitively crayoned coloring book that hung on our walls like an in-home Children’s Louvre. As grandparents of a certain age, now when my wife and I see all their stuffed animals in a pile, we silently share the Buddhist themes of impermanence and suffering. It feels like a Christmas Story staging of Toy Story — our precious time together is ghosted in front of us as a reminder to our mortal selves that “this is it.” This perfect time of their lives, full of wonder and imagination, is just another pandemic curtain closing on the “Duck Duck Goose” show. Now our own mortality is awaiting, as quiet mourners do when “joining” family and friends on a Zoom funeral.
Alone together.
Dave Mason
Then there’s this — amidst all the noise, people find themselves and others. I see a recovering alcoholic/substance abuser in his thirties. He’s been in recovery for seven years. He has a great sponsor and a solid home group. As the pandemic continued, he began to miss the in-person connection with his group and his sponsor. So last week, with the intent of doing “Step work,” he and his sponsor sat safely apart on his sponsor’s back porch. As night began to fall, he said that without any cues, they both simultaneously became silent and quietly surveyed the backyard as darkness fell. He said it was one of the best conversations that he’d ever had.
Like the scene from Little Miss Sunshine, when on their way to the “Little Miss Sunshine” contest, Dwayne flips out after finding out that his color blindness has just destroyed his dream of joining the Air Force, getting away from the “fucking losers” that constitute his family and having a life of his own. He’s profanely inconsolable. His mother says, “I don’t know what to do!” Then his stepfather says to Olive, “Olive, do you want to try talking to him?” Without a word or hesitation, Olive gingerly makes her way down the embankment, ignoring the dust scuffing up her red cowboy boots, and squats down next to her big brother. She puts her arm around Dwayne, leaning her head onto his shoulder. She doesn’t say a word. They both sit together as one in the silence. Quietly, as if whispering a confession, Dwayne says, “O.K., I’ll go.” He then helps Olive up the hill and says to his family, “I apologize for the things that I said, I didn’t mean them.” They load in the van and continue on.
“Off in the distance is a billboard, the message faded but visible, “United We Stand.” We can hope”.
“Where does the actor acquire the understanding that for the doctor takes years of study?"
-Theater Director, Peter Brook
Therapist, you are a performing artist, whether you realize it or not!
The moment a client enters your office, you are on stage, face-to-face with an audience, a scene partner, and a variety of characters you do not yet know how to play (after all, our clients both become and cast us in all of these roles faster than we can say, “How can I help you?”). And every move you make—or don’t make—influences the treatment, the play, the story you tell together.
“Like actors, as therapists our appearance, aura, voice, and relational responsiveness often leave stronger impressions on clients than the words we say or the techniques we use”. This is not to say that our clinical training is of no use; of course it is. But effective technique is less about what we do—less about reading a script by rote—and more about how we do it, how we use ourselves, how we perform our interventions.
When you watch actors performing in movies or plays, do you think about their techniques?—whether they used Strasberg, Adler, or Meisner? Probably not. You are more likely moved by the performers themselves—their ineffable presence, their use of self. Likewise, our clients are more affected by us than by our schools of thought—whether we studied psychoanalysis, CBT, or family systems.
No matter what kind of therapist you are, if you approach your work like an actor—or better yet, like a performing artist in your own right—I promise you will become more awake, alive, and engaged with your clients, while also having a greater capacity to care for yourself. I offer this promise as a psychotherapist who has used my experience as a trained, professional actor every day.
The skeptical reader may think that the words “perform” and “act” don’t belong in the therapy office. When I tell people that I use my training and experience as an actor more than any other resource as a therapist, they often take me to mean either that I’m “fake” with my clients, or that I deploy literal dramatic exercises in session. I’m not (or at least I try not to be) fake with my clients, and I rarely, if ever, use theatrical interventions in session, unless I believe they might be useful for a specific client in a specific moment. However, when I simply think about my clients the way actors think about their characters and scene partners, I enhance my capacity to dive into the deep end of their stories, beyond the words they speak—their “scripts”—even when I do nothing more than listen to them compassionately.
I may not end up doing anything radically different in session from what any other clinician might do instinctively. But by thinking of myself as a performing artist, as opposed to just a clinician, I find creative ways to join my clients in their emotional subjectivity, relate to them like a character who can help them grow, and allow myself to expand personally in the process.
Again, to be clear: “Acting” does not mean being fake, it means finding truth within a given set of circumstances. So, in that sense, “as therapists we are all actors: we use our selves (our primary instrument) to help bring other people’s authentic selves to life”.
Below is a pair of vignettes, each including a significant learning moment for me as an actor, and a corresponding revelation as a therapist. These dramatic/therapeutic narratives, illustrate how my use of self helped me to pursue the three main objectives that apply to the creative process of both artforms:
Other than having a teenager’s build, the only quality I seemed to share with Quigley was the determination to prove my worth. In my case, proving myself not only meant getting hired, which I did, but also finding some genuine version of this unlikely role within me. My greatest challenge was to make an empathic connection with Quigley’s bullish personality, his gratuitous language, and (most difficult of all) his obsessive, violent fantasies. All these qualities—or symptoms, if you will—made me extremely uncomfortable and seemed to alienate me from him, rather than to invite me into his emotional world.
My first task was to create a framework for my rehearsal process, within which I would have room to discover and explore who this person was, through trial and error—ideally without judging him. Rather than begin with preconceived acting choices for Quigley—much like therapists are often tempted to impose treatment interventions onto new clients—I needed to find a way to let him speak to me on his own terms. And since my head could not make sense of this boy, I had to find a way to access him viscerally—using my body, voice, and imagination.
As I began reading his crude and aggressive lines aloud at our first rehearsal, I imagined I was one of the bullies from my own high school past. I widened my legs, puffed out my chest, and spoke with an affected tough-guy bellow, straining to produce the intimidating, nasty persona adopted by so many males from my youth.
The result was what the kids call a “fail!” “My performance was cartoonish and over the top”; I’d created a caricature, not a human being. “Um, that’s a bit much,” my director said, with a penetrating squint of disdain in her eyes. Humiliation flooded my body and shut down my spirit. My effortful impersonation seemed to expose my limitations as both an actor and a man. I wouldn’t need to try so hard if I was actually talented or masculine enough, I thought to myself, further shamed by my inner critic.
But in the same moment, a window opened for me into Quigley’s inner, subjective life. I had unwittingly, but effectively, joined him in his debilitating self-consciousness, vulnerability, fear, loneliness—and self-hatred. His core intention wasn’t to intimidate and destroy other people, I realized. Those behaviors were secondary to his primary objective: to protect himself, validate himself, survive.
With those visceral motivations living in my body and mind, I could commit to Quigley’s macho expressions while maintaining an underlying sense of vulnerable truth. And as I played with this duality—grounded in my own fear of failure, and my instinct to overcompensate for it—I increasingly understood how he/I was motivated by a desperate need to be validated by other people. I could now bring a genuine version of him (and me) into the rehearsal studio with my scene partners, supported by the technical breathing and vocal exercises, as well as mind/body practices I had developed in drama school. (Again: the creative use of oneself is not a replacement for technique, but rather it informs the performer of what specific moves we need to make at any given moment in our scene work.)
By the time the production was on its feet, I was able to embody Quigley without extraneous effort: from his brusque introduction to his cathartic end, in which his mother and best friend hold him in their arms and thwart him from carrying out a violent attack on his classmates. Actors often try to force emotion and tears in high-stakes moments like this—not unlike therapists when we impose heavy-handed clinical interventions onto challenging clients we want to “fix.” As my actor friends say, we often try to “play the end of the scene” too hastily, rather than allow ourselves to be present in every step of the journey.
But I didn’t have to strain myself to find Quigley’s deep-rooted pain for this scene. All I had to do was surrender my feelings to my scene partners, with whom I’d cultivated a great deal of safety and trust throughout our creative collaboration. As we performed the climax of the play, Quigley’s taut energy thawed from my jaw, neck, and shoulders—where it had been deployed as a shield—and it dispersed throughout my body, accessing a range of other emotions. In fact, at one point I awakened to the insight that all along Quigley had been defending against, and overcompensating for, the absence of his father. It’s an abstract clinical exercise to analyze a data point like this about a person’s life, either in a script or a psychological evaluation. “But when we make efforts to join that person in all their subjective bodily, emotional, and intrapsychic complexity, we expand our capacities for empathy”, mutual recognition and creative transformative action, both on and offstage, in and out of therapy. Best of all, we learn to relate to that other person (character or client), no longer through the trailing edge of their transference, as the recipient of their resentment, frustration and fear, but through the leading edge of their transference—as the embodiment of their generative desire, longing, and hope.
Harry burst into my office each week like he was in a race against time; he wanted answers, and he wanted them fast. A straight, white, corporate millennial, he was used to instant gratification, and he expected no less from his therapy. He emphasized that he already understood himself “extremely well,” and that all he needed from me were “professional tips” to reduce stress in his highly successful life.
I was flattered; I’d been cast in the role of commercial guru, the kind who might dominate the American market with bestselling, confidence-inspiring catchphrases. Except I felt too slow, discursive, and insecure to play this part for Harry, more the man behind the curtain than the great and powerful Wizard of Oz. Each week, I expected him to look at me incredulously—much as I’d feared audiences would respond to me portraying a butch, gun-wielding teen—and see that my training and degrees were all a sham. I anticipated the day he’d tear back the curtain and expose me as the talentless hack I felt myself to be in his presence.
On the plus side, Harry showed up for our weekly “rehearsals” consistently, which spoke to the frame I had provided, which apparently made him feel safe enough to “play” with me. But each scene between us had a palpable yet indiscernible tension. First, he’d summarize his week, speedily and with the energetic poise of a cocky movie star—shoulders back, chest protruding forward, eyes sparkly with intense self-assurance. Then he’d present a dilemma—“I need to make more time for relaxation and balance,” for example. At this point, he’d look to me as if to indicate it was my turn to perform, and to prove I was a worthy scene partner.
I would then try to seize the spotlight, so to speak, masking my self-conscious insecurity with a commanding delivery of a line like, “I recommend yoga, three times a week. Put it in your calendar.” I was desperately trying to personify the omnipotent coach I imagined he wanted me to be. And though my “acting choice” arguably answered Harry by his own method, it felt as though I was trying way too hard to impress him—much as I had overcompensated in my bullish portrayal of Quigley, as I stumbled through my first few rehearsals of Hyperactive.
Eventually, I’d look back on these moments and realize how all these unnerving sensations could help tune me in to Harry’s complex internal world, and to join him there. But in the meantime, I felt blocked, like a superficial actor who failed to connect with his character on a deep personal level.
Over time, it became abundantly clear that Harry couldn’t be bothered with my attempted interventions. He’d wince disapprovingly at my suggestions and say things like, “Yoga never works for me. I just end up obsessing about the more productive things I could be doing with my time.” At the end of our sessions, “he’d stride out of my office with a proud posture, leaving me behind to reel in a slouch of inadequacy”. I couldn’t seem to reach him, no matter how hard I tried. I felt like the FBI agent Tom Hanks played in the movie Catch Me If You Can, endlessly chasing Leonardo DiCaprio’s slick and wily character, a master of escape.
This frustrating dynamic manifested in a number of ways between us, including our weekly schedule. Harry would frequently ask to alter our meeting times due to his ever-changing obligations, and I’d accommodate him more than I wanted. I did this because I was afraid to disappoint him. Not only did I sense he’d fire me if I didn’t manage to keep up with his demands, but more significantly, I had an inexplicable sense of dread that he’d erase me from his mind entirely if I let him down. Unwittingly, I was tuning in to Harry’s inner life. I could feel his deep ambivalence about trusting and depending on people vibrating within my own body. And as it turned out, my fears were not unfounded.
One day, after two years of working together, Harry raised the emotional stakes of our scene work. I was running behind (by about a minute), between notes and phone calls, and he had no intention of waiting; it was his time, and he’d enter my office if he wanted to. I was completely shaken off-center as he blasted through my door. Within the flicker of a second, my face flushed with a combination of shock and shame, but also disapproval and a smidge of anger.
As we made eye contact, Harry stopped in his tracks—and his reaction to me was startlingly evocative. While his body asserted its typical conviction, his eyes betrayed a doubt, fear, and deference that I’d never consciously sensed from him before. Since I was too caught off-guard to address this novel improvisation between us in the moment, Harry made a beeline for the couch and shared his latest dilemma as if nothing had happened.
The latest dilemma, it turned out, was that his long-term girlfriend, of whom he’d always spoken glowingly, had proposed to him. “It came out of nowhere!” he exclaimed wide-eyed. “I was totally thrown off my game. Shaken.” Hmm, like what just happened to me now? I thought to myself. “We’ve talked about getting engaged for a while,” he continued, “but I just thought when it happened, it’d be…different.”
“You mean you thought you would be the one who proposed?” I asked.
“Well, yeah,” he replied. “I mean, not because of gender roles and tradition and all that. It’s just…I would’ve made sure it was perfect.”
“What would you have done differently?” I asked.
His eyes squinted as he struggled for an answer. “I guess I just wish she…” he paused for a while, “seemed surer of herself?” As we talked, he realized that this proposal had surfaced an implicit contract in their relationship: that he was in charge of their major decisions as a couple. His girlfriend had gone out on a limb and broken that contract—and now Harry was struggling to understand why he didn’t feel safe following her lead.
Uncharacteristically, his body sank back into the couch as he stared blankly in silence for a while. Finally, he spoke again: “Maybe she’s not the right partner for me.” There it was, the confirmation of my underlying fear; if his long-term girlfriend was expendable, so was I.
“It’s normal to feel a range of emotions at a pivotal time like this,” I said in an effort to validate him. “I appreciate your confusion and doubt, and since your girlfriend seems willing to give you some time to reflect, I suggest we continue talking before you make any big decisions.” He seemed momentarily held by this, but as I watched him take a minute to shield himself with his typical smug poise before leaving the office, I understood deep inside that this sense of security was tenuous, for both of us.
“Harry colonized my mind for the rest of that day, much like a challenging character might consume me as an actor”. At home, I looked in the mirror and tried to emulate his self-possessed posture. As my shoulders dropped back and down, my chest expanded, and my eyes and mouth affected Harry’s cool-guy charm, I began to recall the unpleasant sensations I’d get when trying to play the part of his expert guru. The external posturing I would affect at those times didn’t feel grounded in confidence, but instead seemed to serve as a shield to my internal self-doubt and fear of rejection.
Suddenly, I understood that the same was true for him. The look on his face when he’d barged into my office earlier that day, and the months and months of tension between us, began to make more sense. And as I joined his mind/body experience of self, I realized that what he really wanted was not for me to catch up to him or project the same overcompensating confidence that he did, but to get ahead of him. He longed for me to become someone who could set boundaries with him, disagree with him, and ultimately, care for him—without getting caught up in the same debilitating self-criticism that plagued him. But how could I successfully embody these qualities in the therapy room, and become the character with whom Harry longed to relate?
I thought about the end of Catch Me If You Can, when Tom Hanks learns to approach Leonardo DiCaprio no longer as an elusive fugitive, but as a boy abandoned by his father. I thought also of Harry’s father, who’d died suddenly of a heart attack when Harry was a child. Gazing in the mirror and focusing on the sensations within, I rediscovered what I had first learned with Quigley: biographical details about clients and characters alike resonate within us much more richly when we embody them, rather than simply study or analyze them. I then shifted roles and explored ways that I could present myself to Harry that might make him feel safely held.
I drew inspiration from men, in my life and onscreen, who were both palpably strong and nurturing, including Tom Hanks, Robin Williams, and Barack Obama. I considered their physical groundedness, the clarity of their thoughts, as evidenced by the easy poise of their heads, but also, most significantly, their emotional openness, illustrated by the lack of tension and flow of energy in their chest region.
As I played with where I felt these qualities in my own body, I didn’t try to impersonate the men superficially, but to connect with the experiences in my life—like caring for my younger brothers when I was growing up and being a camp counsellor—that brought out the warmth and confidence Harry needed from me now.
“When Harry next raced into my office, I was prepared to get ahead of him, and relate to him with focus, calm, and an embodied sense of security”. As we revisited the previous session, I validated his anxieties about depending on his girlfriend (or any intimate “scene partner” in his life) and invited him to talk about the pressure he puts on himself to “be ahead” of other people, including me.
Throughout this session, there was more ease, vulnerability, and play between us than ever before. But it wasn’t what I said, so much as how I’d learned to be in the room with him, that made the difference. I was even able to recommend self-care activities like yoga, which he’d rejected in the past, in a way that he now responded to with complete openness—in theater terms, same script, better performance.
As Harry exited that day, he turned around in the doorway, took a moment, and then said through the shimmer of a tear, “Thank you.” I simply smiled in return, maintaining the combination of groundedness, strength, warmth, and vulnerability that we’d discovered together in our session.
While I waited for my next client, alone in my office, I reflected on the connection Harry and I had found, and I recalled an interview with Meryl Streep, in which she explained that in her view, her success as a performer was only as good as it was “the last time.” Thinking of our sessions ahead, I knew we could expect more tension, insecurity, fear, and doubt to manifest between us. But at the same time, I knew my acting training could help me perform on this different kind of stage, where we’d continue to explore various versions of ourselves together.
I initially felt I needed to be someone else in order to access both Quigley and Harry. Like so many actors and therapists, I am driven by the desire to please my collaborators, to be the “expert,” and to “get it right” on the first line reading. But at the same time, in order to connect with our clients, characters, and scene partners as performing artists, we must practice our craft with humility, patience, and the belief that we are enough. We must trust that if we show up to each “rehearsal” with the willingness to be fully present—along with our vulnerabilities, naivete, and deep self-reflection—we will give our creative partners what they need to be present with us as well. Especially if we engage each other in a process of imaginative, empathic play.
Through our respective play sessions, Quigley and Harry both showed me that their apparent toughness, butchness, and self-containment were part of me as well—keys existing somewhere within my instrument, even if I don’t embody them every day. But an even greater revelation for me in both cases, was that the idiosyncratic “soft” qualities that makeup my everyday self—and that I originally believed were obstacles to bringing both young men into the spotlight—turned out to be exactly what they needed to find hidden keys within their own instruments. By playing these untapped versions of ourselves—even, and perhaps especially, when we felt inadequate—each of us found a way to breathe, to integrate, and to become more fully alive.
Note: This article has been adapted from Mark O’Connell’s new book, The Performing Art of Therapy: Acting Insights and Techniques for Clinicians, and his article “Character Work: What Therapists Can Learn from Actors,” in the Psychotherapy Networker, March/April 2019 issue.
But there’s so much psychobabble and neuro-psychobabble out there, and the thing is if you say something is the amygdala as opposed to saying it’s anxiety or fear-based, you haven’t really upgraded the quality of the discourse. You just substituted one word for another. So the risk is that people who learn a half a dozen words about neuroscience think they’re neuroscience literate.
Learning neuroscience takes dedication. It takes work to get beyond the cocktail level of conversation and clichés. It took me ten years to feel like I had any sense of what was going on and I studied it pretty intensively. So I think we all have to be careful, but even more importantly, just because you know some neuroscience doesn’t mean you know anything more than the therapist who doesn’t. It’s really about how you use that information to upgrade the quality of the work you’re doing.
What I’ve been hoping for since I first discovered Buddhism in the 1960s, is that as the world gets smaller and as people from different cultures communicate more, the wisdom of the ancient Eastern philosophies will be interwoven with Western technology and we’ll come to some higher level synthesis of understanding and consciousness. I think we’re in a race between global destruction and global consciousness, so we’ll see who gets to the finish line first.
Evolution is a slow, meandering process. All you have to do is watch the Republican debates to see that. It reminds me of junior high school in the Bronx in New York where we used to engage in chop fights, which was all about humiliating the manhood of other guys just to get a one-up. It doesn’t make me optimistic about the evolution of consciousness, but we’ll see what happens.
LC: The risk with psychology and psychotherapy is that it can lean too much in the direction of helping people tolerate rather than fight against oppression. Self-awareness and self-compassion are crucial experiences and skills that we foster as psychotherapists, but there needs to be a balance there. You can’t become too much of a psychologist. There only needs to be a piece of you that’s a psychologist and there’s another piece of you that has to be willing to go out and fight for systemic change.
As I said before, psychologists tend to watch from the sidelines, and that’s why as a field it has relatively little impact. In fact, the profession gets a lot of bad press because there are plenty of famous psychologists who do staggeringly immoral and unethical things. They are the basis of the cartoon version of the therapist nodding their head and going, “uh huh.”
When I think of somebody like Gandhi or Martin Luther King, Jr., I think of the courage it took to walk into angry crowds. It’s so moving to me and such a powerful act. We can’t just be passive about these voices in our head and in society. We have to get angry because our anger and our assertiveness and our power are all interconnected. If you give up your anger, you give up your power.
But also there’s a different chemistry between different people. Someone who’s a good teacher for one person may not be a good one for another. Same thing with therapists. Every therapeutic relationship creates a new organism—a dyadic field— and sometimes it works and sometimes it doesn’t. The chemistry part we often don’t have any control over.
I don’t know where the technology to research that is going to come from but I think it’s on the horizon. We’ve got to get beyond thinking about brains as individual organs and think about how they weave into relational matrices so we can understand human connection and have a scientific view for the types of things that Buddhists and Hindu meditators and Tibetan scholars have been thinking about for the last several thousand years or so.
In the 1950s Carl Rogers was talking about how to create a healing relationship. Fast forward 65 years and now neuroscience is discovering pretty much what Rogers was talking about. Am I better off talking about it from that perspective than listening to Carl Rogers? I don’t know. But it makes me appreciate what Rogers says even more and in a deeper way when I can see it from this scientific perspective.
Each novel you read is a new way of capturing the universe, and they’re entertaining and stimulating and make you feel human. I feel the same way about the sciences, which is why I love reading E.O. Wilson’s work on ants, because I learn a lot about humans by reading about ants. So many things we do are very ant-like. Plus, ants are interesting.
Since then, my heart is more in the object relations world, I think mostly because it matches my personality and the type of relationships I like to create with people. But I’ve woven in neuroscience, attachment theory, a bit of EMDR, some meditation and self-awareness exercises. It’s a hodgepodge of all the different things that I’ve learned, but I don’t really feel like I’ve got a hammer and everybody who comes in is a nail. It’s more like I’ve got a toolbox of 30 or 40 years of things that I’ve been collecting and I try to figure out how to match as best I can to the needs and the interests of the client.
And what I’ve got to do is just learn the best I can and then sacrifice and move on. This is a very ancient Rig Veda philosophy—every day you wake up, you sacrifice the day before, you move on, you create a new reality.
Had I understood this, I would have spent a lot less time worrying about finding the truth and being acceptable to whatever godhead I happened to run into at the moment. I think idolatry is the problem. Idolatry and objectification.
Certainty leads to ideological beliefs that supersede humanity. At a less dramatic level, we get so enamored with our philosophies and our therapeutic beliefs that we miss our clients because we’re so convinced that we’ve got to convince them we’re right about the things we believe should be true.
Where the field is going to have to upgrade its sophistication and quality is in the areas of like pharmacology, epigenetics, psychoneuroimmunology, diet. All of the actual mechanisms that create and sustain our brains will have to become part of the dialogue about how we help people sustain and maintain health. This might just be my Eastern philosophy bias, but we’ll probably be moving in the direction of more holistic, integrated thinking and treatment—not just combining East and West, but integrating scientific discoveries into our case conceptualizations and treatments.
Finally, I hope that psychology becomes more integrated with education. I have a book series that I’m editing for W.W. Norton which is on the social neuroscience of education, and we’re pushing to have psychologists, neurologists, neuroscientists and educators communicate more so that the things we’re learning can be integrated into each field.
"When are we going to start a family?" asked my husband.
I felt a boa constrictor wrapping around my throat. For months now, the topic of children had evoked tension, leaving us powerless and detached from each other. The argument had become a tradition on Saturday mornings. We would sit in the living room in an awkward silence, avoiding eye contact, until my husband pierced the hush with what he deemed a simple question about our future.
My husband was comforted by having a plan. Three years into our marriage—my second—we were in our mid-thirties, established in our careers, and financially stable. For him the next step in our lives was to start a family, but his need for a plan set off a vicious cycle. I felt ignored and disrespected in our relationship and couldn't justify bringing a child into a fractured marriage. I craved connection and love and was not willing to commit to having a child until we resolved our relationship problems. My resistance made him more insecure and unsure of his focus, and he would ask me about starting a family as a way to relieve his anxiety. Unfortunately, his persistence pushed me away, leaving me feeling trapped and controlled and leaving him stranded without resolution.
“I felt immense pressure both from him and from society to conform and have children. Gradually, I isolated myself from my husband and emotionally shut down, as my sense of self and my voice vanished.” Feeling alone with no one caring about my thoughts and feelings, I believed I was not enough for my husband and that he had married me solely for procreation. Meanwhile, I was inundated with inquiries from our family and friends about when we would be parents.
My mother-in-law often phoned my husband's siblings to convey that her children were failing her since she did not have grandchildren. While growing up, my husband's mother talked a great deal about heirlooms—each piece of jewelry or china was a link between past and future generations. Grandchildren were an essential part of keeping the family traditions alive and to not have them meant the family had failed. She made it clear that my husband was not enough, just as I felt I was not enough as his wife. My resistance to the "plan" was a clear message to him and his mother that I would not conform.
His side of the family was not the only problem. My stepfather had the impression that all couples wanted children. He frequently dropped hints about what a joy they are, pointing to his grandson and saying things like, "See, aren't these fun and not so bad?" For him, family represented connection and closeness. Initially this was endearing but it soon became annoying.
While at a party, I declined an alcoholic beverage, which ignited rumors that I might be pregnant. When I heard the gossip, a wave of heat washed through my body. How dare my friends speculate? It was as if I were starring in the reality show, "When Will Wendy Pop One Out?"